

Your Rheumatoid Arthritis Treatment Plan Explained
Managing rheumatoid arthritis has two main goals: feeling better today and protecting your joints for tomorrow. While finding immediate relief from pain and stiffness is a top priority, it’s just as important to focus on the long game. Uncontrolled inflammation can cause permanent damage, impacting your mobility and independence down the road. A proactive rheumatoid arthritis treatment plan is your best defense. It’s a forward-thinking strategy designed to slow the disease’s progression and preserve your joint health for years to come. This article will show you how to build a plan that balances immediate comfort with long-term protection.
Key Takeaways
- Think beyond medication: A successful RA plan integrates medical care with physical therapy, an anti-inflammatory diet, and supportive therapies to manage pain and protect your joints long-term.
- Be an active partner in your care: Assemble a healthcare team you trust and communicate openly with them; your input is essential for creating and adjusting a treatment plan that fits your life.
- Stay consistent but flexible: Long-term success depends on sticking with your treatment plan consistently, while also being ready to work with your doctor to adjust it when your symptoms or needs change.
What is rheumatoid arthritis and how does it affect your body?
Rheumatoid arthritis, often called RA, is more than just typical joint pain. It's a chronic inflammatory disorder where your body's own immune system mistakenly attacks your tissues. While it’s best known for affecting the joints, RA can also damage a wide variety of body systems, including the skin, eyes, lungs, and heart. Understanding how RA works is the first step toward effective pain management and finding a plan that helps you feel and move better. It’s about getting to the root of the inflammation to manage symptoms and protect your long-term health.
How the autoimmune response works
RA is an autoimmune disease, which means your body's defense system gets its signals crossed. Normally, your immune system is a highly effective guard, protecting you from bacteria and viruses. But with RA, it mistakenly identifies the delicate lining of your joints, called the synovium, as a threat. It launches an attack, sending inflammatory cells to the area. This friendly fire is what causes the synovium to thicken, leading to the swelling and pain you feel in and around the joints. Over time, this persistent inflammation can cause serious damage to the joint itself.
Common symptoms and affected joints
The symptoms of RA can vary, but they often start subtly. You might notice tender, warm, and swollen joints. A classic sign is morning stiffness that lasts for 30 minutes or even a few hours; it usually improves as you start to move around. Unlike some other forms of arthritis, RA typically affects joints symmetrically, meaning if your right wrist is bothering you, your left one probably is too. It most commonly targets the smaller joints first, like those in your hands, wrists, and feet. As the condition progresses, it can spread to larger joints like the knees, ankles, elbows, and shoulders.
How RA can progress without treatment
Ignoring the signs of RA isn't a good idea. Without proper management, the ongoing inflammation can permanently damage cartilage and bone. This can lead to joint erosion and deformity, making movement difficult and painful. The key is to get ahead of the damage. Research shows that early treatment can significantly slow the progression of the disease and even lead to remission, which is a period of low disease activity. Taking action quickly gives you the best chance to protect your joints, maintain your mobility, and continue doing the activities you love.
What are the goals of a rheumatoid arthritis treatment plan?
A good RA treatment plan is more than just a prescription. It’s a comprehensive strategy you create with your doctor to manage the condition from all angles. The main objective is to get the disease under control so you can live a full and active life. This involves tackling the immediate symptoms while also protecting your body from long-term damage. Think of it as a roadmap for your health, with clear goals that guide every decision you make with your healthcare team. The ultimate aim is to achieve remission, a state where your symptoms are minimal or gone completely.
Reduce inflammation and pain
The first and most immediate goal is to get your symptoms under control. This means focusing on reducing the inflammation that causes joint swelling, stiffness, and pain. When your body’s immune system is in overdrive, it creates inflammation that can make even simple movements feel difficult. A successful treatment plan directly targets this process to provide relief. By controlling the swelling, you not only feel better day-to-day, but you also begin to manage the other health issues that can come with RA. This initial step is all about finding effective pain management strategies that allow you to regain comfort and start feeling more like yourself again.
Prevent joint damage
While managing daily pain is essential, a truly effective RA treatment plan looks to the future. The long-term goal is to prevent or slow down permanent damage to your joints. Uncontrolled inflammation can erode cartilage and bone over time, leading to lasting changes in your joints. The main objective here is to lower your disease activity as much as possible. According to the Johns Hopkins Arthritis Center, the ideal outcome is reaching remission, which is when your symptoms essentially disappear. By proactively protecting your joints, you can preserve their structure and function for years to come, helping you stay active and independent.
Maintain mobility and function
Rheumatoid arthritis shouldn't stop you from doing the things you love. A key goal of any treatment plan is to help you maintain your physical abilities and continue with your daily activities. This is about more than just your joints; it’s about your overall ability to function at home, at work, and in your community. A good plan incorporates medical care along with social and emotional support to improve your physical capabilities. Whether it’s buttoning a shirt, walking the dog, or enjoying a hobby, the focus is on making these tasks easier and less painful. The goal is to keep you moving and engaged in your life, not sidelined by your symptoms.
Improve your quality of life
Ultimately, all these goals come together to achieve one main thing: improving your overall quality of life. Living with a chronic condition like RA can be draining, affecting everything from your energy levels to your mood. According to the Arthritis Foundation, a successful treatment plan aims to reduce pain and stiffness, slow the disease’s progression, and lessen the fatigue and weakness that often accompany it. It’s about giving you the freedom to live more comfortably and confidently. When your symptoms are well-managed, you have more energy and capacity to focus on what truly matters to you, leading to a happier, healthier life.
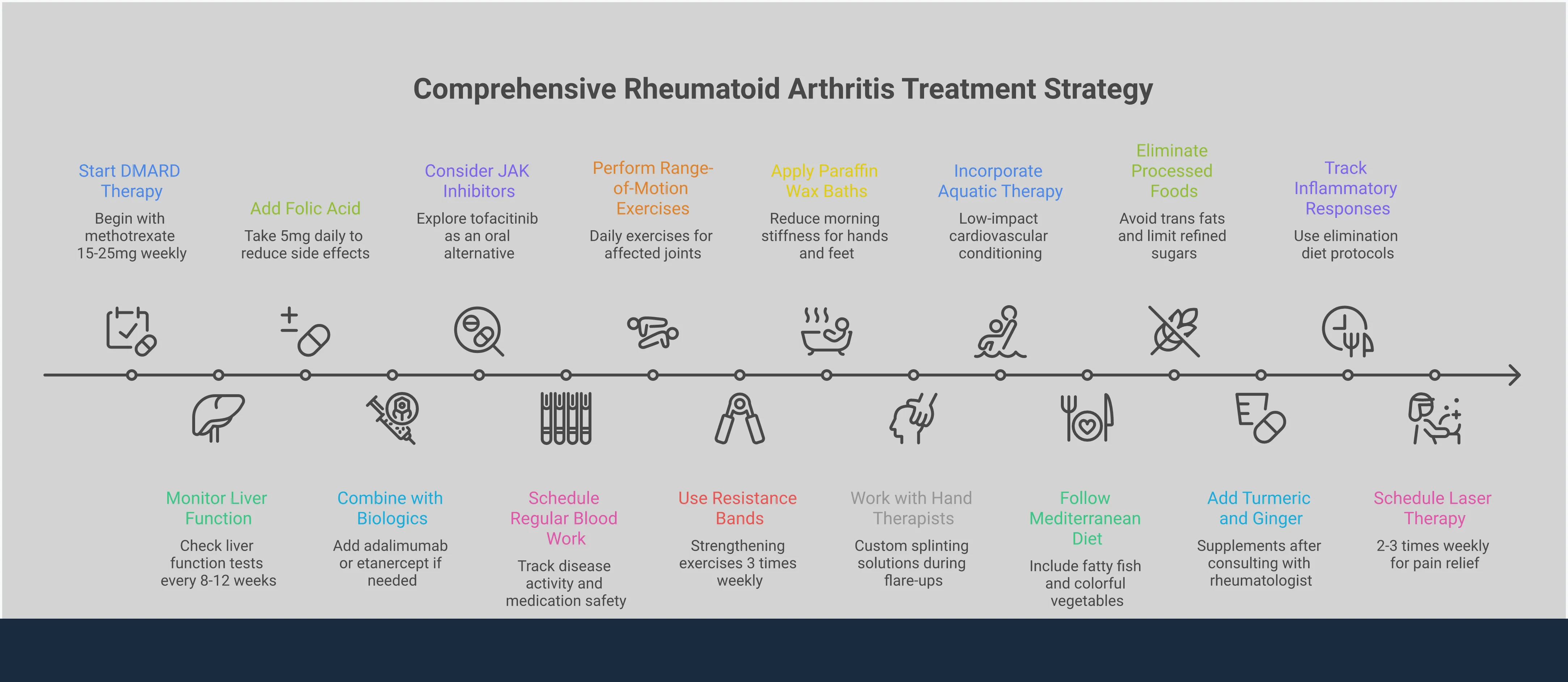
What medications are used to treat RA?
When you're diagnosed with rheumatoid arthritis, your doctor will likely talk to you about medication. This is the primary way to get inflammation under control, slow the disease's progression, and prevent long-term joint damage. The goal is to find the right medication, or combination of medications, that helps you feel your best and maintain your mobility. Think of it as building a personalized toolkit to manage your symptoms and protect your body. There are several categories of drugs your doctor might consider, each playing a different role in your overall treatment plan.
Disease-Modifying Antirheumatic Drugs (DMARDs)
Disease-Modifying Antirheumatic Drugs, or DMARDs, are the foundation of most RA treatment plans. Their main job isn't just to manage pain; it's to slow down the disease itself and help prevent permanent damage to your joints. Your rheumatologist will likely start you on a DMARD soon after diagnosis. The most common first-line medication is methotrexate. If that isn’t the right fit for you, other options like hydroxychloroquine or sulfasalazine might be considered. It can take a few weeks or even months to feel the full effects of a DMARD, so patience is key as your body adjusts to the new treatment.
Biologic therapies and JAK inhibitors
If traditional DMARDs aren't providing enough relief, your doctor might suggest adding a biologic therapy or a Janus kinase (JAK) inhibitor to your plan. These are more targeted treatments that work by blocking specific signals in your immune system that cause inflammation. Biologics, such as adalimumab or etanercept, are complex drugs derived from living cells. JAK inhibitors, like tofacitinib, are a newer class of targeted synthetic DMARDs that come in pill form. These advanced medications can be very effective at managing symptoms and stopping joint damage when other treatments haven't been sufficient, offering another powerful tool in your RA management strategy.
NSAIDs and corticosteroids for symptom relief
While DMARDs and biologics work on the underlying disease, you still need ways to manage day-to-day pain and stiffness. That’s where Nonsteroidal Anti-Inflammatory Drugs (NSAIDs) and corticosteroids come in. You’re probably already familiar with over-the-counter NSAIDs like ibuprofen and naproxen, which can help reduce pain and swelling. For more severe flare-ups, your doctor might prescribe a short course of corticosteroids, like prednisone, to quickly get inflammation under control. It’s important to remember that these medications are for symptom relief and aren't a long-term solution for stopping joint damage. They act as a bridge while your primary rheumatoid arthritis medications take effect.
How combination therapy works
Managing RA isn't always about finding a single magic bullet. Often, the most effective approach is combination therapy, where you take more than one type of medication at the same time. For example, research shows that pairing a traditional DMARD like methotrexate with a biologic can work better than using a biologic on its own. This teamwork approach allows your healthcare provider to attack the inflammation from different angles, leading to better outcomes. Finding the right combination is a collaborative process between you and your rheumatologist. They will tailor the plan based on your specific symptoms, disease activity, and how you respond to different treatment recommendations.
How can physical and occupational therapy help?
While medication is a cornerstone of managing rheumatoid arthritis, your treatment plan shouldn't stop there. Think of physical and occupational therapy as your hands-on support system, designed to help you live more comfortably and confidently. These therapies work alongside your medical treatments to address the daily challenges of RA, from joint stiffness to fatigue.
A therapist can show you how to protect your joints, build strength safely, and conserve your energy so you can focus on the activities you love. By creating a personalized plan, they empower you to take an active role in your own well-being. Integrating these practices helps you maintain your independence and improve your overall quality of life, ensuring your treatment plan is as comprehensive and effective as possible.
Use physical therapy to improve mobility and strength
When your joints are stiff and sore, exercise might be the last thing on your mind. But the right kind of movement is exactly what your body needs. A physical therapist can design a specialized exercise plan to help keep your joints moving and strengthen the muscles around them. This added support reduces the strain on the joints themselves, which can ease pain and improve stability.
Your therapist will teach you safe ways to move and perform exercises without aggravating your symptoms. They can also suggest helpful tools, like splints, to provide extra support when you need it. The goal isn't to push you through pain but to find a sustainable routine that improves your mobility and builds your strength over time.
Adapt daily activities with occupational therapy
Rheumatoid arthritis can make simple, everyday tasks feel like major hurdles. This is where an occupational therapist comes in. Their job is to help you find easier and less painful ways to handle your daily activities, whether at home, at work, or during your hobbies. They are experts in problem-solving the physical challenges of daily life.
An occupational therapist can show you new techniques for everything from opening a jar to typing on a keyboard. They can also recommend assistive devices that protect your joints from unnecessary stress. By making small adjustments to your routines and environment, you can conserve energy, reduce pain, and continue doing the things that are important to you with greater ease and independence.
Add simple exercises to your routine
Regular exercise is a powerful tool for managing RA. It’s not about high-intensity workouts; instead, the focus is on gentle, consistent movement. Gentle exercises strengthen the muscles that support your joints, which can help maintain function and even reduce the fatigue that so often comes with RA.
Think about activities like walking, swimming, or gentle stretching. These low-impact options get your body moving without putting excess pressure on sensitive joints. Even a short walk or a few simple range-of-motion exercises each day can make a significant difference in your pain levels, energy, and overall sense of well-being. The key is to listen to your body and find a routine that feels good for you.
Find the right assistive devices
Using an assistive device isn't a sign of giving in to RA; it's a smart strategy for protecting your body. These tools are designed to make life easier by reducing the stress on your joints during daily tasks. An occupational therapist can help you identify which devices would be most beneficial for your specific needs.
Common aids include splints to support your wrists at night or walking aids like canes to provide stability and take pressure off your knees and hips. You can also find a wide range of gadgets for the kitchen and home, such as ergonomic utensils or long-handled shoe horns. Using these supportive tools can help prevent joint strain, conserve your energy, and allow you to stay active and independent.
Which lifestyle changes support your treatment plan?
Your medical treatment is the cornerstone of managing rheumatoid arthritis, but your daily habits are just as important. The choices you make every day can have a big impact on your inflammation levels, pain, and overall quality of life. Think of these lifestyle changes as powerful tools that work alongside your medications to help you feel your best. By focusing on what you can control, like your diet, activity level, and stress, you take an active role in your own wellness journey. This proactive approach not only helps manage symptoms but also empowers you, giving you a sense of control in a situation that can often feel overwhelming.
Making small, consistent adjustments can lead to significant improvements in your symptoms and help protect your joints from further damage. These changes aren't about a complete overhaul overnight. Instead, they are about building a sustainable routine that supports your body and mind. From the food you eat to how you manage stress, these habits can help reduce inflammation and give you more energy to do the things you love. Integrating these practices into your life is a key part of a holistic approach to preventative wellness that complements your entire treatment plan and helps you build a foundation for long-term health.
Adopt an anti-inflammatory diet
While no diet can cure RA, what you eat can influence inflammation in your body. Adopting an anti-inflammatory eating style, like the Mediterranean diet, can be a great way to support your joint health. According to the American College of Rheumatology, "a healthy diet rich in vegetables, fruits, fish, and healthy fats supports overall health and may help reduce inflammation." Focus on adding more whole foods to your plate, such as leafy greens like spinach, colorful berries, nuts, and fatty fish like salmon, which is packed with omega-3 fatty acids.
At the same time, try to limit foods known to trigger inflammation. This often includes processed foods, sugary drinks and snacks, and excessive red meat. You don’t have to be perfect, just mindful. Every healthy choice is a step in the right direction.
Manage your weight to protect your joints
Maintaining a healthy weight is one of the kindest things you can do for your joints. Extra pounds put additional stress on weight-bearing joints like your hips, knees, and feet, which can increase pain and make it harder to move. The Johns Hopkins Arthritis Center explains, "Maintaining a healthy weight is crucial as it reduces stress on your joints, which can help alleviate pain and improve mobility."
Even losing a small amount of weight can make a noticeable difference in your pain levels and daily function. Combining an anti-inflammatory diet with gentle, low-impact movement is a great strategy for reaching and maintaining a healthy weight. This approach not only protects your joints but also contributes to your overall health and energy.
Improve sleep and reduce stress
Living with chronic pain can be stressful, and stress can make pain feel worse. This cycle also disrupts sleep, and a lack of restorative sleep can increase inflammation and sensitivity to pain. Breaking this cycle is key to feeling better. As the Mayo Clinic suggests, "Finding ways to lower stress, such as through deep breathing exercises or guided imagery, can significantly help control pain and improve your overall well-being."
Try creating a relaxing bedtime routine to signal to your body that it’s time to wind down. You could take a warm bath, read a book, or listen to calming music. Simple mindfulness practices or meditation can also help quiet your mind. Prioritizing both sleep and stress reduction is a vital part of your pain management strategy.
Quit smoking and limit alcohol
If you smoke, quitting is one of the most effective lifestyle changes you can make to manage RA. The Arthritis Foundation warns, "Smoking can exacerbate rheumatoid arthritis and may reduce the effectiveness of treatments." Smoking not only worsens disease activity but can also interfere with how well your medications work, making it harder to get your symptoms under control. Quitting can be challenging, so don't hesitate to ask your doctor for resources and support to help you succeed.
It’s also wise to be mindful of your alcohol intake. Excessive alcohol can contribute to inflammation and may interact with some RA medications. Enjoying a drink in moderation is generally fine for most people, but it's always best to discuss it with your doctor.
How do complementary therapies fit in?
While your medical treatment plan is the foundation for managing rheumatoid arthritis, complementary therapies can be a fantastic addition to your routine. Think of them as supportive tools that work alongside your medications and physical therapy to help you feel your best. These approaches focus on easing symptoms like pain and stiffness, reducing stress, and giving you a greater sense of control over your well-being.
Many people find that integrating these therapies helps them manage the day-to-day challenges of RA more effectively. From targeted treatments that address inflammation directly to practices that calm your mind, these options can round out your care plan. It’s all about creating a comprehensive strategy that addresses your body and mind. Before starting anything new, it's always a good idea to chat with your rheumatologist to make sure it’s a good fit for you and won’t interfere with your current treatments.
Try low-level laser therapy for inflammation
If you’re looking for a drug-free way to manage RA symptoms, low-level laser therapy (LLLT) is an excellent option to consider. This non-invasive treatment uses specific wavelengths of light to penetrate the skin and stimulate cellular activity in your joints. Clinical trials have shown that LLLT can be effective in reducing the pain, morning stiffness, and swelling associated with rheumatoid arthritis. By targeting inflammation at the source, it helps provide relief without the side effects of medication. Our approach to pain management incorporates this technology to help you find comfort and improve your joint function.
Apply heat and cold therapy
Sometimes the simplest solutions can make a big difference. Applying heat and cold are classic methods for temporary symptom relief that you can easily do at home. Using a heating pad or taking a warm shower can help relax tense muscles and ease joint pain. On the other hand, when your joints are swollen and inflamed, applying a cold pack can help reduce swelling and dull the pain. Alternating between the two can be particularly effective. It’s a straightforward, accessible way to manage discomfort during a flare-up or after a long day.
Explore massage and acupuncture
Gentle massage can be incredibly helpful for managing the chronic pain and stress that often come with RA. A trained massage therapist who understands inflammatory arthritis can help soothe sore muscles, improve circulation, and promote relaxation without putting pressure on sensitive joints. Similarly, some people find relief through acupuncture. This traditional practice involves placing thin needles at specific points on the body to help rebalance energy flow and reduce pain. Both therapies can be a valuable part of a holistic approach to feeling better.
Use mind-body practices to manage pain
The connection between your mind and body plays a huge role in how you experience pain. Practices like deep breathing exercises, guided imagery, and meditation can help you manage stress, which is a known trigger for RA flare-ups. When you’re less stressed, your body is better equipped to handle inflammation. These techniques won’t cure RA, but they can change your relationship with pain and give you a powerful tool for coping. Incorporating these practices supports your overall preventative wellness and helps you maintain a sense of calm and balance.
How to build and work with your RA healthcare team
Living with rheumatoid arthritis isn't something you have to figure out on your own. In fact, managing RA works best with a team approach. Think of yourself as the team captain, surrounded by experts who can help you manage symptoms, protect your joints, and live a full life. Your role is to assemble the right players and make sure everyone is working together toward your health goals.
Building this team is one of the most empowering steps you can take. It puts you in control of your treatment plan and ensures you have support from every angle, from medical care to emotional well-being. With the right people in your corner, you can face the challenges of RA with confidence and a clear path forward.
Find a rheumatologist to lead your care
Your first and most important team member is a rheumatologist. This is a doctor who specializes in arthritis and other diseases of the joints, muscles, and bones. They will be the one to officially diagnose your RA, prescribe medications, and monitor your progress. A good rheumatologist will act as the leader of your care, coordinating with other specialists and adjusting your treatment as needed. When you’re looking for the right fit, don’t be afraid to ask questions. You want someone who listens, explains things clearly, and makes you feel like a partner in your own care. The American College of Rheumatology has a tool to help you find a qualified specialist in your area.
Involve your primary care doctor and other specialists
While your rheumatologist focuses on RA, your primary care physician (PCP) is still essential for your overall health. They’ll manage routine check-ups, vaccinations, and any other health issues that come up. It’s important that your PCP and rheumatologist communicate about your care. Beyond your doctors, your team might include a physical therapist to improve mobility, an occupational therapist to help with daily activities, and a mental health professional for emotional support. You can also add complementary care providers, like our team at Laser Lab Therapy, to help manage inflammation and pain with non-invasive treatments like low-level laser therapy.
Communicate effectively with your team
Open and honest communication is the glue that holds your healthcare team together. To make the most of your appointments, try to prepare ahead of time. Write down your questions, track your symptoms in a journal, and be ready to talk about how you’re feeling, both physically and emotionally. It’s important to work closely with your doctor and be upfront about any side effects you’re experiencing or challenges you’re facing with your treatment plan. Remember, you are the expert on your own body. Your input is crucial for creating a plan that truly works for you.
Clear up common treatment myths
One common myth is that once you find a treatment, you’re set for life. The reality is that managing RA is a dynamic process. Your needs can change over time, and your treatment plan will likely need adjustments along the way. It’s a long-term partnership between you and your healthcare team. Another misconception is that you just have to live with the pain. With today’s advanced treatments and a comprehensive team approach, the goal is to minimize pain and prevent joint damage so you can maintain your quality of life. Don’t hesitate to speak up if your current plan isn’t working as well as you’d like.
What to expect when you start treatment
Starting a new treatment plan for rheumatoid arthritis can feel like a big step, but it’s also a hopeful one. Your journey toward feeling better begins with understanding what lies ahead. The first few months are all about working with your healthcare team to find the right combination of therapies that work for your body. This process involves some trial and error, regular communication with your doctor, and a little patience. Knowing what to expect can help you feel more in control and confident as you move forward with your plan.
Know the initial phases and timelines
When you first begin treatment, expect to be in close contact with your rheumatologist. It’s common for patients to have appointments every one to three months at the start. This frequent follow-up allows your doctor to see how you’re responding to the initial treatment and make adjustments quickly. This phase is about establishing a baseline and finding the most effective approach for you. Think of it as a partnership. Your feedback is essential, so be prepared to share how you’re feeling, what symptoms are improving, and any new concerns you might have. This initial period sets the foundation for your long-term care.
Why early treatment is so important
When it comes to RA, acting quickly makes a huge difference. Clinical studies show that starting treatment with specific medicines, like DMARDs, early on makes it more likely for your symptoms to ease up, a state called remission. Without treatment, joint damage can happen surprisingly fast. Getting ahead of the inflammation is key to protecting your joints and preserving your mobility for the long run. An early and aggressive approach to pain management not only helps you feel better sooner but also significantly improves your chances of achieving long-term remission and maintaining your quality of life.
Monitor your medication's effectiveness and side effects
Your treatment plan is dynamic, not static. A big part of managing RA involves regular check-ups with your doctor to see if your medicines are working and to watch for any side effects. This is where you become an active player on your healthcare team. Keeping a simple journal of your symptoms, energy levels, and any potential side effects can provide valuable information for your doctor. Open communication is crucial. If a medication isn't helping or is causing problems, your doctor needs to know so they can adjust your plan. This ongoing monitoring ensures your treatment remains both safe and effective.
Manage flare-ups and adjust your plan
Living with RA often means learning to handle flare-ups, which are periods when your symptoms suddenly worsen. Part of your treatment plan should include a strategy for these times. This might involve short-term medication changes, rest, and complementary therapies to reduce inflammation. It’s also important to work with your doctor to identify potential triggers for your flares, like stress or certain activities. Your plan is a living document; it will likely be adjusted over time as your needs change. Staying proactive with preventative wellness strategies can also help minimize the frequency and severity of these flare-ups, keeping you on a more even keel.
How to maintain your treatment plan long-term
Managing rheumatoid arthritis is a marathon, not a sprint. Once you and your doctor find a treatment plan that works, the next step is figuring out how to stick with it for the long haul. This isn't just about remembering to take your medication; it's about creating a sustainable lifestyle that supports your health and keeps your symptoms under control. Long-term success comes from consistency, open communication with your healthcare team, and the flexibility to adapt as your body’s needs change over time. It’s about building habits that become second nature, allowing you to focus less on managing your condition and more on living your life.
Think of your treatment plan as a living document. It will likely evolve as you learn more about what works for you. The key is to stay engaged and proactive. By committing to your care, you can prevent long-term joint damage, maintain your mobility, and continue doing the things you love. A successful long-term strategy often involves a combination of medication, lifestyle adjustments, and supportive therapies that work together to reduce inflammation and manage pain. It’s a partnership between you and your healthcare providers, where your feedback is just as important as their expertise. Let’s walk through the essential habits that will help you maintain your progress and feel your best for years to come.
Stick to your treatment for continuous care
Consistency is your greatest ally in managing RA. For most people, medications like DMARDs or biologics are the foundation of their treatment because they work to slow the disease's progression and prevent permanent joint damage. It can be tempting to skip a dose when you’re feeling good, but this can unfortunately trigger a flare-up.
Following your doctor's instructions exactly is crucial for keeping inflammation at bay. If you start experiencing side effects, don't just stop taking your medication. Call your doctor right away. They can often adjust your dosage or find an alternative that works better for you. Open communication ensures your treatment remains both effective and manageable.
Get regular check-ups and lab tests
Think of your regular appointments with your rheumatologist as essential tune-ups for your body. These visits are about much more than just refilling prescriptions. They are your opportunity to check in, discuss your symptoms, and make sure your treatment is still on the right track. During these check-ups, your doctor will likely perform a physical exam, ask about your pain and mobility, and order lab tests.
These tests help monitor your disease activity and check for any potential side effects from your medication. This proactive approach allows your healthcare team to catch any issues early and keep you ahead of the disease, ensuring your plan continues to protect your joints and overall health.
Know when it's time to adjust your plan
A treatment plan that works wonders today might need a few tweaks down the road. Rheumatoid arthritis can be unpredictable, and your body’s needs can change over time. That’s why it’s so important to pay attention to your symptoms and be honest with your doctor about how you’re feeling. If you notice your symptoms are getting worse or you’re experiencing more frequent flares, it might be time to adjust your plan.
Don’t be discouraged if this happens; it’s a normal part of managing a chronic condition. Your doctor may suggest changing your medication, adjusting the dosage, or adding a new therapy to your routine. Being an active participant in your care helps your team make the best decisions for your health.
Combine treatments for the best results
The most effective RA treatment plans are rarely one-dimensional. Research shows that combining different types of medications can often work better than using a single drug alone. But a truly comprehensive approach goes beyond prescriptions. It integrates lifestyle habits, physical therapy, and supportive treatments to address your symptoms from all angles. This might include an anti-inflammatory diet, gentle exercise, and stress-reduction techniques.
Adding non-invasive, drug-free therapies can also provide significant relief. Our services for pain management use targeted light therapy to help reduce inflammation and ease discomfort without side effects. By creating a multi-layered strategy, you and your doctor can build a personalized and sustainable plan that supports your long-term well-being.
Frequently Asked Questions
How do I know if my RA treatment plan is working? You'll know your plan is working when you notice a real improvement in your day-to-day life. Key signs include less morning stiffness, reduced pain and swelling in your joints, and more energy. Your doctor will also track progress with blood tests that measure inflammation levels. The ultimate goal is to feel capable of doing your daily activities with greater ease. It’s a combination of what the lab results say and, more importantly, how you actually feel.
Can I manage rheumatoid arthritis with just lifestyle changes and complementary therapies? While a healthy diet, regular movement, and therapies like low-level laser therapy are fantastic for managing symptoms and improving your quality of life, they work best as part of a comprehensive plan. Medications like DMARDs are currently the most effective tool we have to slow the disease's progression and prevent permanent joint damage. Think of lifestyle habits and complementary care as powerful allies that support your medical treatment, not replace it.
What's the difference between a flare-up and my treatment not working? A flare-up is a temporary spike in your symptoms, often lasting for a few days or weeks, and can sometimes be linked to a trigger like stress or overexertion. In contrast, if your treatment plan is no longer effective, you'll likely notice a slow but steady decline in your condition over a longer period. Your baseline pain might increase, or your joint function might worsen consistently. Tracking your symptoms can help you and your doctor see the pattern and decide on the right next step.
How long does it typically take to feel better after starting treatment? Patience is key when starting a new RA treatment. Medications for immediate relief, like NSAIDs or corticosteroids, can help you feel better within days. However, the core medications that address the disease itself, such as DMARDs, can take several weeks or even a few months to reach their full effect. Your rheumatologist will monitor you closely during this initial period to ensure the plan is moving you in the right direction.
Besides my rheumatologist, who else should be on my healthcare team? Building a well-rounded team is one of the best things you can do for yourself. Your primary care doctor remains essential for your overall health. A physical therapist can help you improve strength and mobility safely, while an occupational therapist can show you how to adapt daily tasks to protect your joints. Many people also find that including a mental health professional provides valuable support for coping with the emotional challenges of a chronic condition.
Frequently Asked Questions
Is light therapy safe for athletes?

Yes, light therapy is completely safe and highly beneficial for athletes. It promotes faster muscle recovery, reduces inflammation, and supports performance without the risks of medication or downtime. That’s why professional and amateur athletes worldwide rely on it to train smarter and recover quicker.
How many sessions will I need?

The number of sessions varies depending on the type and severity of your condition. Many patients notice improvement after 3–5 sessions, while chronic conditions may require ongoing care for best results. During your initial consultation, we’ll design a personalized treatment schedule tailored to your body’s response and recovery goals.




