

15 Ways to Manage Arthritis Pain Naturally
Dealing with joint pain used to feel like a choice between home remedies and prescriptions. The good news? You have so many more options now. Science has opened the door to innovative, drug-free treatments that help your body heal itself, without invasive procedures or side effects. Therapies like Class IV laser and red light therapy use specific light waves to reduce inflammation and repair tissue deep down. When you pair these with foundational habits like a healthy diet and proper exercise, you create a powerful plan to effectively manage arthritis pain and truly improve your quality of life for the long term.
Key Takeaways
- Combine different approaches for better relief: A single strategy is rarely enough for complex arthritis pain. You'll get the best results by layering different drug-free methods, such as gentle exercise, an anti-inflammatory diet, and targeted therapies that support your joints from every angle.
- Focus on inflammation for lasting comfort: Instead of just masking symptoms, effective management addresses the root cause of pain. You can calm inflammation through your diet, consistent movement, and advanced treatments like light therapy that work with your body’s natural healing processes.
- Get professional guidance for a personalized plan: You don’t have to figure everything out on your own. Working with a specialist like a physical therapist or light therapy expert removes the guesswork, ensures your routine is safe, and helps you build the most effective plan for your specific needs.
What is Arthritis?
When you hear the word "arthritis," you might picture a single condition, but it’s actually a broad term for over 100 different issues that impact your joints and connective tissues. According to Yale Medicine, arthritis is a leading cause of disability, characterized by symptoms like joint pain, stiffness, and swelling that can make everyday activities feel like a challenge. While it’s often associated with aging, arthritis can affect anyone, regardless of age or lifestyle. The key to effective management is understanding that not all joint pain is the same. Identifying the specific type of arthritis you have is the first and most important step toward finding a relief plan that works for you, whether that involves conventional medicine, lifestyle changes, or innovative, non-invasive therapies.
Understanding the Different Types of Arthritis
Because "arthritis" is an umbrella term, getting a specific diagnosis is crucial. The right approach for one type might not be effective for another. For example, managing an autoimmune condition requires a different strategy than addressing wear-and-tear damage. Knowing the root cause of your joint pain helps you and your healthcare provider create a targeted plan to reduce inflammation, manage symptoms, and protect your joints from further damage. Let’s look at four of the most common types you might encounter.
Osteoarthritis
Often called "wear-and-tear" arthritis, osteoarthritis (OA) is the most common form. It develops when the protective cartilage that cushions the ends of your bones gradually breaks down over time. Without that smooth cartilage, bone can start to rub directly against bone, leading to pain, stiffness, and reduced mobility. OA typically affects joints that bear a lot of weight, like the knees and hips, but it's also common in the hands and spine. While it can result from the natural aging process, factors like past injuries, genetics, and excess body weight can also contribute to its development.
Inflammatory Arthritis
Unlike osteoarthritis, inflammatory arthritis is an autoimmune condition. This means your body's own immune system mistakenly attacks healthy joint tissues, triggering widespread inflammation. This attack causes pain, swelling, redness, and stiffness that is often worse in the mornings. Conditions like rheumatoid arthritis (RA) and psoriatic arthritis fall into this category. Because it's a systemic disease, inflammatory arthritis can sometimes affect other parts of the body, including the skin, eyes, and internal organs, leading to symptoms like fatigue and fever. Managing this type of arthritis often involves addressing the underlying immune response.
Post-traumatic Arthritis
As the name suggests, post-traumatic arthritis (PTA) develops after a physical injury to a joint. A bad fall, a sports-related accident, or a car crash can damage the cartilage or bone, making the joint more susceptible to arthritis down the road. According to medical experts, this condition can appear years after the initial injury was treated and healed. The damage from the trauma accelerates the wear-and-tear process, leading to symptoms similar to osteoarthritis, including pain, swelling, and instability in the affected joint. Athletes and individuals with physically demanding jobs are often at a higher risk for developing PTA.
Gout
Gout is a unique and intensely painful form of inflammatory arthritis. It occurs when high levels of uric acid in the blood lead to the formation of sharp, needle-like crystals in a joint. The result is a sudden and severe attack of pain, redness, tenderness, and swelling, which often affects the big toe. These flare-ups can happen without warning, sometimes waking people up in the middle of the night. While the big toe is the most common site, gout can also affect other joints like the ankles, knees, and wrists. Management typically involves medications and dietary changes to lower uric acid levels and prevent future attacks.
Who is Affected by Arthritis?
Arthritis is far more common than most people realize, affecting approximately one in four adults in the United States. It’s a misconception that joint pain is exclusively a problem for the elderly. While the risk of developing most types of arthritis does increase with age, it can impact people from all walks of life, including children and young adults. Certain factors can increase your risk, such as genetics, a family history of arthritis, being overweight, or having a previous joint injury. Because it’s so widespread, finding a sustainable pain management strategy is essential for maintaining an active and fulfilling life.
Which Doctors Treat Arthritis?
If you’re dealing with persistent joint pain, your primary care physician is a great starting point, but they will likely refer you to a specialist for a precise diagnosis and treatment plan. Depending on the type of arthritis you have, you may work with one or more experts who specialize in musculoskeletal health. Building the right healthcare team is a key part of managing your condition effectively, as different specialists bring unique skills to the table, from medication management to surgical intervention.
Rheumatologists
A rheumatologist is an internal medicine doctor who specializes in diagnosing and treating musculoskeletal diseases and systemic autoimmune conditions. If you have a form of inflammatory arthritis like rheumatoid arthritis, psoriatic arthritis, or gout, a rheumatologist will likely be your main doctor. Their primary focus is on managing the condition with medications designed to reduce inflammation and suppress the overactive immune response that causes joint damage. They help you manage your condition for the long term, adjusting treatments as needed to keep symptoms under control.
Orthopaedic Surgeons
An orthopaedic surgeon specializes in the surgical treatment of bones, joints, ligaments, tendons, and muscles. You might be referred to one if your arthritis is severe, particularly if it’s osteoarthritis or post-traumatic arthritis that hasn't responded to other treatments. These surgeons can perform procedures ranging from minimally invasive arthroscopy to full joint replacements. However, surgery is typically considered a last resort. Most orthopaedic surgeons will explore non-surgical options with you first, including physical therapy, injections, and lifestyle modifications, before recommending an operation.
Common Medical Approaches for Arthritis
When you first receive an arthritis diagnosis, your doctor will likely discuss a few standard medical treatments to help manage your symptoms. These approaches are often the first line of defense in conventional medicine and are primarily focused on reducing pain and inflammation. They can range from simple over-the-counter pills to more targeted injections administered directly into the painful joint. While these methods can provide significant relief for many people, they are designed to manage symptoms rather than address the root cause. Understanding these common treatments is helpful as you build a comprehensive care plan that may also include complementary, drug-free therapies.
Over-the-Counter and Prescription Medications
For many people, the journey to arthritis relief begins in the pharmacy aisle. Medications are one of the most common ways to handle the daily aches and stiffness that come with joint inflammation. These options can be incredibly helpful for managing flare-ups and making movement more tolerable. However, it's important to remember that they primarily mask the pain. For sustainable, long-term wellness, medications are often best used as part of a broader strategy that includes lifestyle changes and therapies that support your body’s natural healing processes.
NSAIDs and Pain Relievers
The most frequently recommended medications for arthritis pain are nonsteroidal anti-inflammatory drugs (NSAIDs) and other pain relievers. Over-the-counter options like ibuprofen (Advil) and naproxen (Aleve) work by reducing inflammation, while acetaminophen (Tylenol) focuses on blocking pain signals to the brain. According to the Mayo Clinic, these are often used for pain that comes and goes. If these aren't strong enough, your doctor might prescribe a more potent NSAID. While effective for short-term relief, long-term use can carry risks, including stomach irritation and kidney issues.
A Warning About Narcotic Pain Medicines
While it might seem logical to use strong pain medicines for severe arthritis, experts strongly advise against it. Narcotic medications, also known as opioids, are generally not recommended for managing chronic arthritis pain. Research from orthopedic specialists shows that they don't work well for this type of pain and can introduce significant risks, including dependency and addiction. Furthermore, long-term use can actually make your recovery more difficult if you eventually need joint surgery. It’s better to focus on safer, more effective strategies for long-term relief.
Injections for Temporary Relief
When oral medications aren't providing enough relief, or if pain is concentrated in a specific joint like a knee or shoulder, your doctor might suggest injections. This approach delivers medication directly to the source of the inflammation and pain. Injections can offer significant, albeit temporary, relief that can last for several weeks or even months. This can create a valuable window of opportunity for you to participate more effectively in physical therapy or other restorative activities. However, they are not a permanent fix and are often used sparingly.
Cortisone Injections
Cortisone shots are a common treatment for arthritis flare-ups. Cortisone is a powerful steroid that works by dramatically reducing inflammation within the joint space. When injected directly into a painful joint, it can provide rapid relief from pain and swelling. This relief can help you move more comfortably and break a cycle of pain and inactivity. However, the effects are temporary, and there is a limit to how many injections you can safely receive in a single joint per year, as overuse can potentially weaken cartilage and tendons over time.
Hyaluronic Acid Injections
Another option, primarily for knee osteoarthritis, is hyaluronic acid injections. Hyaluronic acid is a substance that occurs naturally in the synovial fluid that lubricates your joints. The idea behind these injections is to supplement this fluid, helping the joint move more smoothly and with less pain. Sometimes referred to as viscosupplementation, this treatment is intended to act like a lubricant or shock absorber inside the knee. Patient results can be mixed; some people find significant relief, while others notice little difference. It's an option to discuss with your doctor if other treatments haven't been successful.
Can You Manage Arthritis Pain Without Drugs?
If you're living with arthritis, you know that managing the daily aches and stiffness can feel like a full-time job. While medication is a common route, many of us are looking for ways to find relief without the potential side effects or the feeling of just masking the problem. The good news is that there are powerful, effective, and drug-free ways to manage arthritis pain that work with your body’s natural healing abilities.
The goal of these approaches isn’t just to quiet the pain, but to address one of its root causes: inflammation. By focusing on reducing inflammation and improving joint function, you can build a sustainable plan for long-term comfort and mobility. Exploring these options can open the door to a more active, comfortable life, allowing you to get back to the activities you love.
How Natural Approaches Soothe Joint Pain
Natural approaches are effective because they focus on reducing inflammation and supporting your body’s ability to heal itself. Instead of simply blocking pain signals, treatments like light therapy get to the source of the discomfort. Photobiomodulation, the process behind laser therapy, uses specific wavelengths of light to penetrate tissue, decrease inflammation, and promote cellular repair. This helps calm irritated joints and improve mobility from the inside out.
These strategies often work best when combined. For example, pairing light therapy with gentle physical activity can be incredibly effective for pain management. The laser helps reduce the initial pain and stiffness, making it easier and more comfortable for you to move, while the movement itself helps maintain joint flexibility and strength.
What Are the Benefits of Going Drug-Free?
Choosing a drug-free path for arthritis relief is about more than just avoiding pills—it’s about pursuing a holistic approach to your health. The most significant benefit is sidestepping the potential side effects that can come with long-term medication use, such as digestive issues or dependency. Instead of just managing symptoms, you’re actively promoting healing and improving your overall joint function.
This approach also allows for highly personalized care. Your body is unique, and your treatment plan should be too. At Laser Lab, we understand that what works for one person might not be the best fit for another. Our philosophy centers on creating tailored plans that might include targeted laser sessions for specific joints or systemic light therapy to address widespread inflammation. It’s a safe, non-invasive way to find lasting relief and improve your quality of life.
What Are the Best Drug-Free Strategies for Arthritis?
Finding relief from arthritis pain doesn’t always have to start at the pharmacy. Many effective, drug-free strategies can help you manage your symptoms right from home. These approaches focus on soothing inflammation, improving joint function, and reducing the stress that often comes with chronic pain. Think of them as your foundational toolkit for feeling better. By integrating simple habits like targeted temperature therapy, topical remedies, and gentle movement into your daily routine, you can take an active role in your own comfort and well-being. These methods are accessible, easy to start, and can make a significant difference in how you feel day-to-day.
Soothe Joints with Heat and Cold Therapy
One of the simplest yet most effective ways to manage arthritis pain is by using heat and cold therapy. The key is knowing which one to use and when. Gentle heat, like from a heating pad or a warm bath, is perfect for soothing stiff joints and relaxing tight muscles. It works by increasing blood flow to the area, which can ease chronic aches. On the other hand, cold therapy is your go-to during a painful flare-up. Applying a cold pack helps constrict blood vessels, which can significantly reduce swelling and inflammation. A good rule of thumb is to use heat for persistent aches and stiffness, and cold for acute pain and swelling. You can find more ideas in this drug-free pain management tool.
Find Relief with Topical Gels and Creams
When a specific joint is aching, topical treatments can offer targeted relief. You can find many over-the-counter creams and gels designed to soothe joint pain. Look for products containing ingredients like capsaicin, which creates a warming sensation, or menthol and camphor, which provide a cooling effect that can distract your brain from the pain. Beyond creams, don’t underestimate the power of scent. Aromatherapy with lavender, for example, has been shown to lower levels of the stress hormone cortisol. Since stress is a known trigger for pain, creating a calming environment can be a simple yet powerful part of your pain management plan.
Ease into Gentle Stretching and Movement
When your joints hurt, the last thing you might want to do is move. However, gentle, regular exercise is one of the best things you can do for arthritis. Movement helps lubricate your joints and strengthens the muscles that support them, which takes pressure off the affected areas. You don’t have to run a marathon; simple activities like daily walks, gentle stretching, or swimming can improve your range of motion and reduce pain over time. In fact, clinical guidelines recommend supervised therapeutic exercise as a core part of managing osteoarthritis. Start slowly with a few simple stretches each morning to ease stiffness and gradually build from there.
Protect Your Joints with Braces and Assistive Devices
Sometimes, your joints need a little extra backup to get through the day, and that’s where braces and assistive devices come in. Think of a brace for an arthritic knee as a supportive hug—it helps stabilize the joint, which can significantly reduce pain and give you more confidence when you move. The same principle applies to your feet and ankles. Supportive shoes or custom orthotics can make a world of difference by distributing your weight more evenly, taking the pressure off sensitive areas. It’s all about giving your joints the structural support they need so they don’t have to work so hard.
This idea of support extends beyond just braces. Simple assistive tools can also protect your joints from unnecessary strain during daily tasks. Things like jar openers, long-handled shoe horns, or even a cane can help you manage activities that might otherwise cause a flare-up. Using these devices isn’t a sign of weakness; it’s a smart strategy for conserving your energy and protecting your joints for the long haul. By reducing the daily wear and tear, you create a better environment for other treatments, like light therapy, to work effectively.
How Can Exercise Relieve Arthritis Pain?
When your joints are stiff and sore, the last thing you probably want to do is move them. It’s a common feeling, but gentle, consistent movement is one of the most effective ways to manage arthritis pain long-term. Think of it this way: exercise strengthens the muscles that surround and support your joints. When those muscles are strong, they take a lot of the pressure and strain off the joints themselves, which can lead to less pain and better mobility.
Regular physical activity also helps maintain a healthy weight, lubricates your joints, and can even improve your mood and sleep quality. The key isn’t to push through sharp pain but to find the right kind of movement that feels supportive, not stressful. It’s about working with your body to build resilience. By incorporating gentle exercise into your routine, you can take an active role in your own pain management and find lasting relief. It’s a powerful, drug-free tool you have at your disposal every single day.
Start with Low-Impact Cardio like Walking or Swimming
Low-impact exercises are your best friend when dealing with arthritis because they get your body moving without jarring your sensitive joints. Walking is a fantastic starting point—it’s free, you can do it almost anywhere, and it helps build stamina and strength in your lower body. If you have access to a pool, swimming or water aerobics can feel incredible. The water’s buoyancy supports your body weight, giving your joints a much-needed break while still providing gentle resistance to strengthen your muscles. Cycling, whether on a stationary bike or outdoors, is another great option because its smooth, repetitive motion is easy on the knees and hips.
Improve Joint Mobility with Yoga and Tai Chi
Sometimes, the best movements are slow and intentional. Practices like tai chi and yoga are perfect for improving flexibility, balance, and your overall range of motion. Tai chi, often called "meditation in motion," involves slow, flowing movements that build strength and stability while calming the mind. It’s a whole-body approach that helps you feel more connected and in control. Similarly, a gentle or restorative yoga practice can help release tension in stiff joints and lengthen tight muscles. These mindful movements not only help physically but also reduce the stress that can make pain feel worse.
Support Your Joints with Strength Training
The idea of lifting weights might sound intimidating, but you don’t need to be a bodybuilder to reap the benefits. Building muscle is crucial for protecting your joints. Strong muscles act like a natural brace, absorbing shock and reducing the load on your cartilage. You can start simply with resistance bands, light hand weights, or even your own body weight. Aim to work your major muscle groups a few times a week, focusing on slow, controlled movements. This creates a supportive structure around your joints, making everyday activities like climbing stairs or carrying groceries feel much easier and less painful.
Arthritis and Exercise: Myths vs. Facts
One of the biggest myths is that you shouldn't exercise if you have arthritis because it will cause more pain and damage. While you should always listen to your body and avoid activities that cause sharp pain, avoiding movement altogether can actually make stiffness and pain worse. It’s important to learn the difference between the gentle ache of muscles getting stronger and the kind of pain that signals a problem. The "no pain, no gain" mentality doesn't apply here. Instead, the goal is to start slow, be consistent, and gradually increase your activity level as you feel stronger and more comfortable.
Exercises to Approach with Caution
While gentle movement is incredibly beneficial, it’s also important to be smart about the types of activities you choose. Not all exercise is created equal when you’re managing joint pain. The main things to be mindful of are high-impact activities like running, jumping, or intense aerobics. These movements can send a jolt through your joints, which can aggravate inflammation and pain. Similarly, certain strength exercises, such as deep squats or lunges, can place a lot of stress on the knees and hips. This doesn’t mean you have to avoid them forever, but you might need to modify them or focus on a smaller range of motion. The most important rule is to listen to your body. If an exercise causes sharp, shooting, or increased joint pain, it’s a signal to stop and reassess. It’s about finding what feels supportive, not what pushes you past your limits.
How Can Your Diet Reduce Arthritis Inflammation?
When you live with arthritis, your body is often in an inflammatory state. The good news is that what you eat can either worsen or improve this inflammation. While there’s no magic diet that cures arthritis, making thoughtful food choices can significantly reduce your pain and improve your joint health. Think of your diet as a powerful tool in your pain management toolkit. By focusing on whole, anti-inflammatory foods, you can support your body from the inside out, complementing other treatments and helping you feel more in control of your symptoms. It’s about creating a sustainable eating pattern that nourishes your joints and helps calm the inflammation that causes so much discomfort.
Fight Inflammation with Foods You'll Love
One of the most effective ways to fight inflammation is to load your plate with foods that have natural anti-inflammatory properties. Omega-3 fatty acids, found in fatty fish like salmon, as well as in walnuts and flaxseed, are fantastic for reducing inflammation and morning stiffness. Spices can also be your allies. Turmeric contains a powerful compound called curcumin, which can reduce joint pain and swelling by blocking inflammatory chemicals. Try adding it to soups, smoothies, or curries. Similarly, ginger root extract can decrease joint pain and inflammation with an effect that some compare to ibuprofen. Adding these foods to your regular meals is a simple, delicious way to support your joints.
Consider a Mediterranean or Plant-Based Diet
Instead of focusing on individual foods, you might find it easier to adopt a broader eating pattern known for its health benefits. The Mediterranean diet is a great example. It emphasizes fish, nuts, olive oil, whole grains, fruits, and vegetables—all staples that help fight inflammation. A plant-based diet, which centers on fruits, vegetables, legumes, and whole grains, can have a similar effect. These dietary patterns are rich in antioxidants and fiber, which help calm your body’s inflammatory response. The goal isn’t perfection but to shift your overall eating habits toward whole, unprocessed foods that nourish your body and help manage your arthritis symptoms over the long term.
Foods That May Worsen Inflammation
Just as some foods can help, others can make inflammation worse. It’s wise to limit or avoid foods that are known to be pro-inflammatory. These include refined carbohydrates like white bread and pastries, fried foods, and sugary drinks like soda. Red and processed meats, such as burgers and hot dogs, can also contribute to inflammation. Added sugar is a major culprit, as it triggers the release of inflammatory messengers in your body. You don’t have to cut these foods out completely, but reducing your intake can make a noticeable difference in your pain levels and overall well-being. Start by making small swaps, like choosing whole-grain bread or sparkling water instead of soda.
Arthritis Diet Myths You Can Ignore
It’s easy to get overwhelmed by conflicting advice about diet and arthritis. One common myth is that you need to cut out all nightshade vegetables (like tomatoes, peppers, and eggplant). While a small number of people may be sensitive to them, there’s no scientific evidence that they cause inflammation for most people. Another myth is that one "miracle" food will solve all your problems. In reality, a consistent, balanced diet is far more effective than relying on a single ingredient. The best approach is to focus on an overall healthy eating pattern, listen to your body, and notice which foods make you feel better or worse.
The Impact of Smoking on Joint Pain
While we often focus on diet and exercise, there's another lifestyle factor that has a huge impact on joint health: smoking. Smoking triggers widespread inflammation throughout your body, which is a primary driver of arthritis pain. It also reduces blood flow, starving your joints of the oxygen they need to repair themselves. This can speed up cartilage loss and make pain more severe, especially in conditions like osteoarthritis. The connection is so strong that smoking is a known cause of rheumatoid arthritis and can make the disease much worse after diagnosis. If you smoke, quitting is one of the most powerful steps you can take to protect your joints and reduce your pain. It's a foundational change that supports all your other efforts to feel better.
Can Light Therapy Help with Arthritis?
If you’re looking for a modern, non-invasive way to manage arthritis pain, light therapy is an excellent option to consider. Instead of just masking symptoms, this approach works at a cellular level to address the root cause of your discomfort: inflammation. The core idea is simple yet powerful: specific wavelengths of light are used to penetrate your skin and tissues, stimulating your body’s natural healing processes. This can lead to reduced pain, less swelling, and improved mobility in your joints, all without relying on medication or invasive procedures.
Light therapy is a gentle and effective way to find relief. It helps increase circulation to the affected area, bringing more oxygen and nutrients to your tissues to support repair. At the same time, it helps carry away waste products that can contribute to pain and inflammation. For many people living with arthritis, incorporating light therapy into their routine provides a way to actively manage their condition and improve their quality of life. It’s a forward-thinking strategy that complements other natural approaches, giving you another tool for effective pain management.
How Class IV Laser Therapy Reduces Inflammation
Class IV laser therapy is a powerful, targeted treatment that uses specific wavelengths of light to penetrate deep into your tissues. Unlike a surface-level treatment, this laser energy reaches the muscles, ligaments, and joints affected by arthritis. Once there, it stimulates cellular activity, which helps accelerate healing and significantly reduce inflammation. Think of it as giving your cells a direct energy source to repair themselves more efficiently. This process offers a potent, drug-free way to get relief right at the source of your pain, helping you move more freely and comfortably.
Easing Joint Pain with Red Light Therapy
While some treatments target specific joints, red light therapy can offer more widespread benefits. Our full-body red light therapy beds deliver gentle, healing light across your entire system. This is especially helpful for arthritis because it can reduce systemic inflammation, which is often an underlying factor in joint pain. Beyond targeting inflammation, this therapy also supports better circulation and can even promote more restful sleep—both of which are crucial for your body’s ability to heal and manage pain. It’s a holistic approach that supports your overall preventative wellness.
Get Targeted Relief with Deep Tissue Laser Therapy
When you have a specific joint—like a knee or a shoulder—that’s causing most of your trouble, deep tissue laser therapy can provide focused relief. This treatment allows us to apply therapeutic light directly to the area that needs it most. By concentrating the energy on a particular joint and the surrounding tissues, we can effectively address the localized pain and inflammation associated with arthritis. This targeted approach is perfect for speeding up performance recovery and getting you back to your daily activities with less discomfort.
What Other Therapies Can Help with Arthritis?
Building a well-rounded approach to arthritis care often means looking beyond a single solution. While light therapy is a powerful tool for reducing inflammation and pain, combining it with other hands-on treatments can create a more comprehensive and effective strategy. Think of it as assembling your personal care team, where each specialist brings a unique skill to help you feel and move better. These therapies focus on the body's structure, muscles, and energy systems to provide relief from different angles.
Exploring these options allows you to find what works best for your specific symptoms and lifestyle. For some, the targeted pressure of acupuncture provides immense relief, while others might benefit more from the guided movements of physical therapy. The goal is to create a supportive routine that addresses your pain, improves your mobility, and enhances your overall well-being. When integrated thoughtfully, these drug-free therapies can work together to support your body’s natural healing processes and give you more control over your pain management journey.
Using Acupuncture for pain management
Acupuncture is a practice rooted in Traditional Chinese Medicine that involves placing very thin needles into specific points on the body. The idea is to rebalance the body's energy flow, but modern research suggests it has tangible effects on pain and inflammation. Many studies have shown that acupuncture can help with arthritis pain, particularly for those with osteoarthritis in the knee. By stimulating nerves, muscles, and connective tissues, this therapy can prompt your body to release its natural painkillers. If you're looking for a targeted way to address joint pain without medication, acupuncture is a well-regarded option worth exploring.
How Massage Therapy Soothes Aching Joints
A therapeutic massage can feel like a welcome relief for stiff, aching joints. This hands-on therapy involves a practitioner manipulating your body's soft tissues, including muscles and connective tissues, to ease discomfort. The primary goals are to reduce swelling, alleviate pain, and improve flexibility. Beyond the physical benefits, massage is also incredibly effective for promoting relaxation and reducing the stress that often comes with chronic pain. While more research is needed to confirm its long-term effectiveness for arthritis, many people find that regular massages are a valuable part of their pain management routine.
Working with a Physical Therapist
When your joints hurt, the last thing you might want to do is move. However, the right kind of movement is essential for managing arthritis. A physical therapist is a movement expert who can design a safe and effective exercise program tailored specifically to you. They’ll guide you through exercises that strengthen the muscles supporting your joints, improve your flexibility, and increase your range of motion. This personalized approach helps reduce pain and improve your daily function, making it easier to do the things you love. A physical therapist can also help you improve your performance recovery if arthritis is holding you back from your fitness goals.
Could Chiropractic Care Help Your Joints?
Chiropractic care focuses on the relationship between your spine and nervous system and how it affects your overall health. For arthritis, a chiropractor uses manual manipulation to restore proper movement to joints that have become restricted. By improving joint function, this therapy can help reduce pain and slow the progression of joint degeneration. It’s often recommended for people with osteoarthritis, especially in the hips, knees, ankles, or feet. A chiropractor can help ensure your body is properly aligned, which can take unnecessary strain off your arthritic joints and provide lasting relief.
How Can Mindfulness Help You Manage Pain?
When you live with chronic pain, it can feel like it takes over every part of your life. But what if you could change your relationship with that pain? That’s the core idea behind mindfulness. It’s not about pretending the pain isn’t there; it’s about learning to observe it without letting it control your thoughts and emotions. The mind-body connection is incredibly powerful. By calming your mind, you can often soothe your body’s response to pain signals.
Mindfulness gives you a set of tools to manage the stress, anxiety, and frustration that so often accompany arthritis. It helps you create a mental space between you and the sensation of pain, giving you a greater sense of control. Think of it as a skill you can build over time. With consistent practice, you can learn to respond to pain with calm awareness instead of automatic tension, which can make a significant difference in your day-to-day comfort and quality of life.
Reduce Stress to Change Your Perception of Pain
Stress and pain are closely linked. When you’re stressed, your body releases hormones that can increase inflammation and make you more sensitive to pain. Mindfulness practices are a direct way to interrupt this cycle. By focusing on the present moment, you can calm your nervous system and lower your stress levels. This doesn’t make the pain vanish, but it can change how you experience it. Instead of being overwhelmed, you can learn to acknowledge the sensation without the added layer of stress and anxiety. This is a key part of a drug-free pain management approach that helps you cope in a healthier, more resilient way.
Try These Meditation and Breathing Exercises
You don’t need to sit for hours to feel the benefits of meditation. Starting with just five minutes a day can make a real impact. Simple breathing exercises are especially effective for managing moments of intense pain or anxiety. Try this: inhale slowly through your nose for four counts, hold your breath gently for four counts, and then exhale slowly through your mouth for six counts. This technique helps calm your nervous system almost instantly. You can also explore guided meditation apps or videos that walk you through body scans or other mindfulness practices designed to reduce anxiety and pain.
Improve Your Sleep to Promote Healing
Pain can make getting a good night’s sleep feel impossible, but a lack of sleep can make your pain feel even worse the next day. Mindfulness can help break this frustrating cycle. By practicing a short meditation or breathing exercise before bed, you can quiet a racing mind and prepare your body for rest. Quality sleep is when your body does its most important repair work, reducing inflammation and promoting healing. When you combine mindfulness with other therapies that support your body’s natural recovery processes, you create a powerful strategy for long-term preventative wellness and better joint health.
### Exploring Cognitive Behavioral Therapy (CBT)Managing arthritis isn't just a physical challenge; it's a mental and emotional one, too. This is where Cognitive Behavioral Therapy (CBT) can be a game-changer. CBT is a type of therapy that helps you identify and change negative thought patterns and behaviors. When it comes to chronic pain, the way you think about your discomfort can directly influence how you feel. CBT teaches you practical skills to reframe thoughts like, "This pain is unbearable and will never end," into more manageable ones, such as, "I am feeling pain right now, and I have tools to cope with it." It’s a proactive way to manage the psychological weight of arthritis, giving you a greater sense of control over your well-being. You can learn more about how CBT helps with chronic pain from the Mayo Clinic.
Understanding and Managing Arthritis Flare-Ups
Living with arthritis often means navigating periods of relative calm followed by sudden flare-ups, where your symptoms of pain, stiffness, and swelling intensify. These flares can be frustrating and disruptive, making even simple daily activities feel like monumental tasks. One day you might feel great, and the next, walking to the mailbox or opening a jar can be a painful struggle. This unpredictability is one of the most challenging aspects of the condition, but understanding what a flare-up is and what might be causing it is the first step toward managing it effectively.
The goal isn't to eliminate flare-ups entirely—that may not always be possible—but to shorten their duration, lessen their intensity, and feel more prepared when they happen. By paying attention to your body and your daily habits, you can often identify patterns or specific triggers that lead to a spike in your symptoms. This knowledge empowers you to make proactive choices, whether that means adjusting your activity level, managing stress, or having a go-to relief plan ready. The Arthritis Foundation offers excellent resources to help you live better by learning to manage these painful episodes.
What Triggers a Pain Flare-Up?
Arthritis flare-ups can feel like they come out of nowhere, but they often have specific triggers. These periods of increased pain can appear suddenly or build gradually, lasting for a few days or even weeks. One of the most common triggers is overdoing it—pushing yourself too hard during a workout or spending a long day on your feet can strain your joints and lead to a flare. Other factors can include stress, poor sleep, or even an illness like the flu. While the exact cause isn't always clear, learning to recognize your personal triggers is a key part of managing your symptoms and preventing future flare-ups.
Does Weather Affect Arthritis Pain?
If you’ve ever felt like you can predict a storm in your joints, you’re not alone. Many people with arthritis report that their pain and stiffness worsen with changes in the weather. While the scientific connection is still being studied, many believe that shifts in barometric pressure can affect the fluid in your joints, leading to increased discomfort. For some, it’s the cold, damp days of winter that cause the most trouble, while others find that hot and humid summer weather makes their swelling worse. The key is to pay attention to how your body responds and have a plan for those difficult weather days, like gentle indoor stretches or a warm bath. You can find more information on this from Arthritis UK.
Tips for Managing Arthritis in Common Areas
Arthritis doesn't affect every joint in the same way. The pain you feel in your hands might require a different management approach than the ache in your knees or hips. Because these joints have different jobs and handle different kinds of stress, your relief strategies should be tailored to their specific needs. For example, strengthening the muscles around your knees can provide crucial support, while learning new ways to grip objects can make a world of difference for your hands. It’s all about making small, targeted adjustments to your daily routine.
By focusing on the specific areas that give you the most trouble, you can create a more effective and personalized pain management plan. This approach allows you to address the unique challenges of each joint, whether it’s finding the right kind of exercise, using supportive devices, or adapting everyday tasks. The following tips offer practical, actionable advice for some of the most common spots affected by arthritis. By implementing these strategies, you can reduce strain, improve function, and find more comfort throughout your day. Yale Medicine offers a great guide to managing pain by body part.
Hip Arthritis
When your hips are aching, high-impact activities like running or jumping can make the pain much worse. Instead, switch to low-impact exercises that are gentler on your joints. Walking, swimming, or cycling are excellent choices because they strengthen the muscles that support your hips without the jarring impact. It’s also wise to be mindful of movements like deep lunges and squats, which can put excessive strain on the hip joint. On days when the pain is particularly bad, applying ice or a heating pad can provide simple, effective relief and help you stay mobile.
Hand Arthritis
Managing arthritis in your hands is all about finding a balance between movement and protection. Gentle exercises that take your fingers and wrists through their full range of motion can help maintain flexibility, but it’s important to avoid activities that put too much stress on these small joints. Look for ways to adapt daily tasks to reduce strain. For example, use tools with larger, padded grips, or choose clothing with zippers instead of small buttons. These simple modifications can make a huge difference in your daily comfort and help preserve your joint function over the long term.
Knee Arthritis
Your knees bear a significant amount of your body weight, so one of the most effective ways to reduce knee pain is to maintain a healthy weight. Every pound you lose takes several pounds of pressure off your knees. Strengthening the muscles around your knees, particularly your quadriceps and hamstrings, also provides better support and stability for the joint. When your knees are swollen and painful, applying ice can help reduce inflammation. For chronic stiffness and aches, a heating pad can help relax the surrounding muscles and improve blood flow to the area, offering soothing relief.
Foot and Ankle Arthritis
The joints in your feet and ankles support your entire body, so keeping them healthy is crucial. Maintaining a healthy weight is a great first step to reduce the daily load they have to carry. If you notice that certain activities cause your pain to flare up, try modifying them or finding alternatives. For acute pain and swelling, an ice pack can be very effective. To improve stability and flexibility, incorporate gentle ankle-strengthening exercises and Achilles tendon stretches into your routine. These simple movements can help support the joints and reduce your risk of further discomfort.
How to Safely Add These Strategies to Your Routine
Finding new drug-free strategies to manage arthritis is empowering, but it’s normal to feel a little hesitant about where to begin. The key is to introduce these changes thoughtfully so they become lasting habits, not sources of stress or injury. By focusing on a few core principles, you can build a routine that supports your joints and fits your life. The most successful approaches are built on starting slow, staying consistent, and working with professionals who can guide you.
Start Slow and Listen to Your Body
When you’re motivated to feel better, it’s tempting to jump in with both feet. But a slow and steady approach will always win. Your body needs time to adapt to new movements and therapies, so begin with shorter sessions and lower intensity. Regular, gentle exercise is proven to strengthen the muscles that support your joints, which can significantly reduce pain over time.
Pay close attention to what your body is telling you. If a joint feels painful, swollen, or hot, that’s your cue to rest. Pushing through sharp pain can set you back, so learn to distinguish between the discomfort of building strength and a signal to stop. Your body is your best guide—trust its wisdom.
Find a Consistent, Sustainable Pace
Consistency is more important than intensity. A 15-minute walk every day will do more for your joints than a strenuous hour-long workout once a week. Small, regular efforts help maintain flexibility, reduce stiffness, and build momentum. Remember that any amount of activity is better than none, and even small amounts of movement can lead to significant improvements.
Think of it this way: each time you stretch, eat an anti-inflammatory meal, or practice a mindfulness exercise, you’re making a deposit in your health bank. These actions add up, creating a strong foundation for long-term joint health. Don’t get discouraged if you miss a day; just get back to your routine when you can. Progress, not perfection, is the goal.
Work with a Pro to Create Your Personal Plan
You don’t have to figure this all out on your own. Arthritis affects everyone differently, which is why a personalized plan is so important. Working with a professional, like a physical therapist or a light therapy specialist, can help you find the right combination of strategies for your unique needs. They can create a custom exercise plan to improve your strength and flexibility while ensuring you’re performing every movement safely and correctly.
At Laser Lab Therapy, we specialize in creating personalized pain management plans that address the root cause of your discomfort. Our team can help you integrate treatments like Class IV laser therapy into your routine for targeted, drug-free relief. Getting expert guidance removes the guesswork and gives you the confidence to move forward.
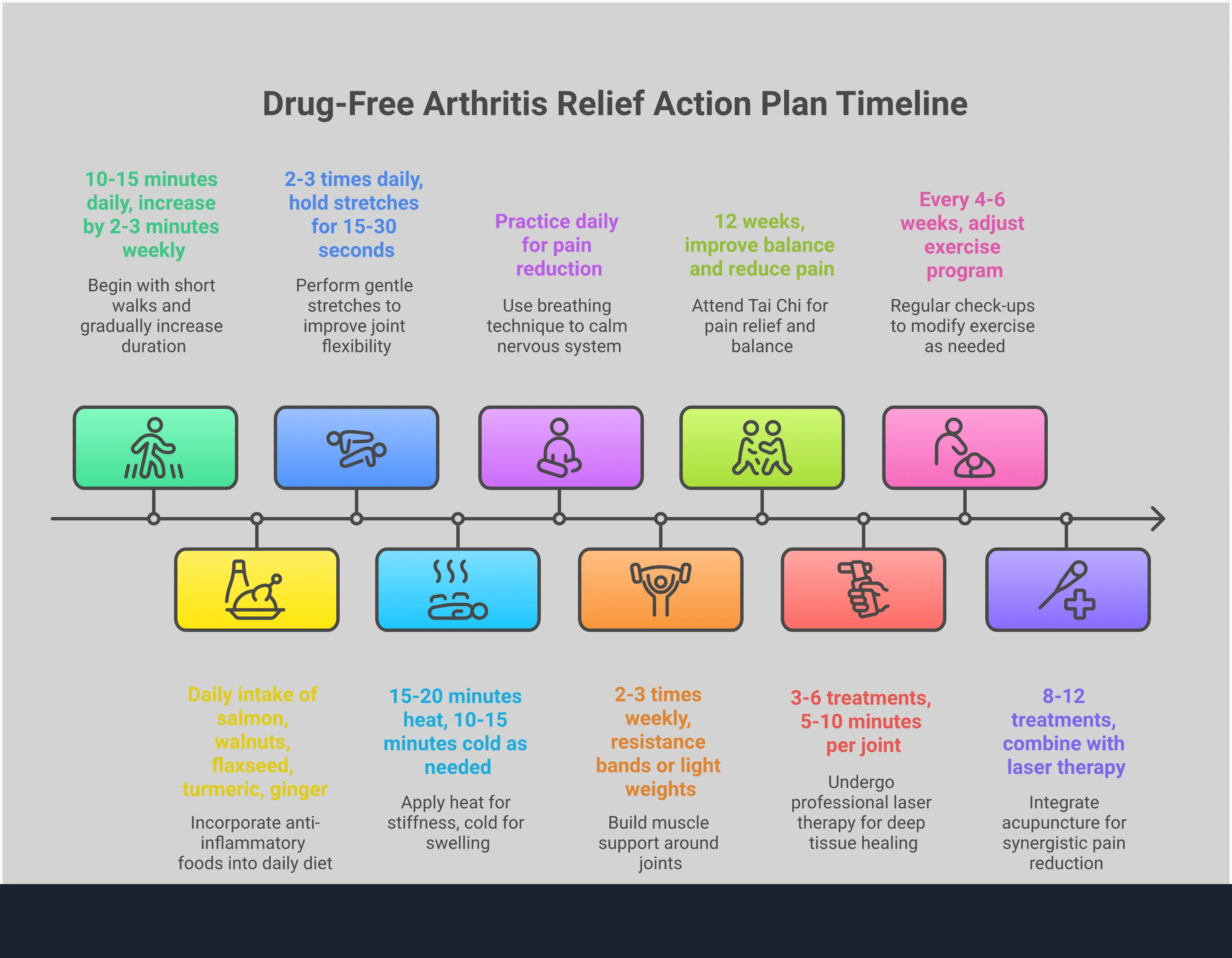
Putting It All Together: Your Arthritis Action Plan
Finding what works for your arthritis is a personal process. Since pain is complex, a single solution rarely does the trick. The most effective approach is often a combination of strategies tailored to your body and lifestyle. Building a personal plan empowers you to take control of your symptoms and live more comfortably. It’s about creating a toolkit of different therapies and habits that you can rely on day-to-day.
This plan isn’t set in stone. It should be a living document that you can adapt as your symptoms change or as you discover new strategies that work for you. Think of it as your roadmap to feeling better, with clear, actionable steps you can take to manage pain and improve your joint health.
Combine Therapies for Better Results
Because everyone experiences arthritis differently, a multi-faceted approach is usually best for long-term relief. For example, combining regular, gentle movement with targeted treatments can be more effective than either strategy alone. Physical therapy can strengthen the muscles around your joints, while treatments like laser therapy can directly address inflammation and pain. At Laser Lab, we create personalized pain management plans that often blend different light therapies to calm inflamed joints and make movement easier. The key is to find a synergy between different methods that supports your body from multiple angles.
Track Your Progress and Adjust Your Plan
How do you know which strategies are actually working? Keeping a simple journal can make a huge difference. Note your pain levels, what you ate, how you slept, and what activities you did each day. This practice helps you identify patterns, recognize triggers, and see the positive impact of new habits. A pain management tool like a journal also helps you communicate more clearly with your healthcare providers. By tracking your experience, you can make informed adjustments to your plan, focusing more on what brings you relief and modifying what doesn’t.
Use a Pain Journal to Identify Patterns
It’s one thing to feel better or worse on a given day, but it’s another to understand why. This is where a pain journal becomes your personal detective. By taking a few minutes each day to jot down your pain levels, what you ate, how well you slept, and your physical activities, you start to connect the dots. You might notice that your knee always flares up after a rainy day or that your pain is lower on days you do your morning stretches. This simple practice helps you recognize your personal triggers and see which habits are truly making a difference. Plus, having this detailed record makes conversations with your healthcare team more productive, allowing you to work together to fine-tune your plan for the best possible results.
Manage Your Weight to Support Your Joints
Maintaining a healthy weight is one of the most impactful things you can do for your joints, especially your knees and hips. Extra pounds put additional stress on these weight-bearing joints, which can increase pain and inflammation. The good news is that even a small amount of weight loss can provide significant relief. In fact, research shows that losing just one pound can reduce the stress on your knee joint by four pounds. By pairing an anti-inflammatory diet with gentle exercise, you can work toward a healthy weight that better supports your joints for years to come.
How Losing Weight Reduces Joint Pressure
It’s easy to forget how much work our joints do every day, especially the ones that bear our weight, like our hips and knees. The pressure on these joints isn’t just equal to your body weight; it’s magnified with every step you take. In fact, every pound you carry puts about five pounds of pressure on your hip and knee joints. When you look at it that way, you can see how even a small amount of weight loss can make a huge difference. Losing just five pounds can take 25 pounds of pressure off your joints. This simple change can significantly ease pain and inflammation, making it a cornerstone of any effective, drug-free pain management plan.
When Is It Time to See a Professional?
While managing arthritis at home is empowering, there are times when you need a professional in your corner. Think of it less as a last resort and more as the next logical step in your wellness journey. Seeking expert guidance means you’re getting a plan tailored specifically to your body, your pain, and your goals. A professional can help you understand what’s really going on with your joints and introduce you to powerful, effective treatments you can’t do on your own.
Pain is complex, and what works for one person might not work for another. That’s where a specialist comes in. They can help you cut through the noise and identify the most effective drug-free strategies for your unique situation. They can also help you combine different approaches safely to get the best results, ensuring that your efforts at home are supported by targeted, clinical care. The goal is to build a sustainable, long-term approach to pain management that helps you feel and move better without relying on medication. It’s about finding a partner who can support you in living a full, active life and provide the tools you need to thrive. This partnership ensures you're not just guessing what might work but are following a clear path toward relief. A professional can also track your progress, make adjustments as needed, and offer encouragement along the way, which can be invaluable when dealing with chronic pain.
Signs You Might Need More Support
It’s important to listen to your body. While some stiffness and discomfort can be managed, certain signals suggest it’s time for more support. If a joint is consistently painful, swollen, or feels hot to the touch, your body is telling you it needs help. Pay attention if the pain isn't getting better with rest or if it’s starting to interfere with your daily life, like walking the dog or enjoying your hobbies. Since pain is so personal, what works for a friend might not be the right solution for you. When your current routine isn’t providing the relief you need, that’s a clear sign to seek a professional diagnosis and a more structured treatment plan.
Intense or Persistent Pain
A dull ache that comes and goes is one thing, but pain that’s intense or never seems to let up is your body’s way of sending a clear message. If your joint pain is constant, wakes you up at night, or is so severe that it stops you from doing everyday tasks, it’s time to bring in a professional. Pain is complex, and what works for one person might not be the right fit for you. A specialist can help you get a clear diagnosis and create a personalized pain management plan that targets the source of your discomfort, rather than leaving you to guess what might work.
Severe Swelling, Warmth, or Discoloration
Look at your affected joint. Is it noticeably swollen compared to the other side? Does it feel warm or hot when you touch it? Have you noticed any redness or unusual discoloration? These are all classic signs of significant inflammation that isn’t being controlled by your current routine. While some mild swelling can be typical with arthritis, severe or persistent symptoms indicate that your body is struggling and needs more support. A professional can help you understand the cause of this inflammation and introduce targeted therapies to calm it down effectively.
Signs of Infection
It’s crucial to distinguish between a typical arthritis flare-up and a joint infection, which requires immediate medical attention. If your joint pain comes on suddenly and is extremely severe, and is accompanied by a fever or chills, it could be a sign of a septic joint. An infected joint will often be very swollen, red, and intensely painful to move. This is not something to wait out. If you experience these symptoms, it’s important to seek medical care right away to prevent serious complications.
How to Find the Right Practitioner for You
Finding the right practitioner is about finding a partner for your health. You want someone who listens to your concerns and is dedicated to finding drug-free solutions. A physical therapist, for example, can design a personal exercise program to improve your strength and mobility. For more targeted relief, you might explore advanced treatments like Class IV laser therapy. This non-invasive approach is a powerful way to reduce inflammation and pain directly at the source. When you’re looking for a provider, ask about their experience with drug-free pain management. The right fit will be someone who can create a personalized plan that helps you reach your wellness goals without surgery or medication.
Frequently Asked Questions
With so many options, where is the best place to start? It can feel overwhelming, but you don't have to do everything at once. The best approach is to pick one or two simple strategies that feel manageable for you right now. For example, you could start by incorporating a gentle 15-minute walk into your daily routine and trying a topical cream on a particularly sore joint. Small, consistent actions build momentum and are far more effective than trying to overhaul your entire life overnight.
How quickly can I expect to feel a difference with these natural approaches? Results really vary from person to person and depend on the strategy you're using. Something like heat or cold therapy can provide immediate, temporary relief from an ache or flare-up. On the other hand, changes from diet and exercise are more gradual and build over several weeks or months as your body gets stronger and inflammation subsides. With treatments like laser therapy, many people report feeling a noticeable improvement after just a few sessions.
Is light therapy actually safe for arthritis? Yes, light therapy is a very safe and non-invasive treatment for arthritis pain when administered by a trained professional. Unlike medications, it doesn't come with a list of potential side effects because it works by supporting your body's own natural healing mechanisms. The light energy simply stimulates your cells to reduce inflammation and repair tissue more efficiently, all without breaking the skin or introducing any foreign substances.
Can I use these drug-free strategies if I'm already taking arthritis medication? Absolutely. These natural strategies are designed to work alongside your current care plan, not replace it. Think of them as additional tools you can use to manage your symptoms and improve your overall well-being. However, it's always important to talk with your doctor before making any significant changes to your routine, especially when it comes to exercise or diet, to ensure everything works together safely.
How is professional laser therapy different from the red light devices I can buy online? The main differences are power and precision. The Class IV lasers we use in a professional setting are significantly more powerful than at-home devices, allowing the therapeutic light to penetrate much deeper into your joint tissues for more effective relief. A professional can also create a personalized treatment plan that targets your specific areas of pain, ensuring you get the right dose of light exactly where you need it most.
Frequently Asked Questions
Is light therapy safe for athletes?

Yes, light therapy is completely safe and highly beneficial for athletes. It promotes faster muscle recovery, reduces inflammation, and supports performance without the risks of medication or downtime. That’s why professional and amateur athletes worldwide rely on it to train smarter and recover quicker.
How many sessions will I need?

The number of sessions varies depending on the type and severity of your condition. Many patients notice improvement after 3–5 sessions, while chronic conditions may require ongoing care for best results. During your initial consultation, we’ll design a personalized treatment schedule tailored to your body’s response and recovery goals.




