

9 Rheumatoid Arthritis Thoracic Spine Symptoms to Know
Have you ever noticed a link between stiffness in your mid-back and a feeling of tightness in your chest? It might seem like two separate issues, but they can be connected. Your thoracic spine is anchored to your rib cage, meaning inflammation in your spinal joints can directly impact your breathing and comfort. This is particularly important for those with RA, as the condition can cause problems in this area. Knowing the specific rheumatoid arthritis thoracic spine symptoms helps you connect the dots between what you’re feeling, leading to a clearer diagnosis and a more comprehensive approach to finding relief.
Key Takeaways
- Listen for specific signs beyond back pain: RA in the thoracic spine can cause prolonged morning stiffness, a grinding sensation when you move, and even chest or lung symptoms like a persistent cough due to the spine's connection to your ribs.
- A clear diagnosis is a team effort: Since symptoms can be subtle, getting answers involves working with your doctor through a physical exam, blood tests, and imaging scans to build a complete picture of your spinal health.
- Combine treatments for better results: An effective management plan pairs medical treatments from your doctor with supportive natural therapies, such as light therapy for inflammation and gentle exercise to maintain mobility.
What is Rheumatoid Arthritis in the Thoracic Spine?
When you hear "rheumatoid arthritis," you probably picture swollen knuckles or sore knees. While RA most often affects smaller joints, it can also impact the spine. The neck is a more common spinal target, but RA can sometimes develop in the thoracic spine, which is the middle section of your back. Understanding how this autoimmune condition affects this area is the first step toward finding effective relief. Because it's less common, RA in the mid-back can be overlooked or mistaken for other issues, so getting familiar with the basics is key to having informed conversations with your doctor.
What is Rheumatoid Arthritis?
Rheumatoid arthritis (RA) is an autoimmune disease where your immune system mistakenly attacks your body's own healthy tissues. It primarily targets the synovium, the lining of your joints, causing inflammation that leads to pain, swelling, and stiffness. Over time, this can result in joint damage. This chronic condition affects about one in every 100 adults. Effectively managing the inflammation is key to controlling symptoms and protecting your joints, which is where therapies focused on pain management can play a supportive role.
The Role of Your Thoracic Spine
Your thoracic spine is the longest part of your spinal column, running from the base of your neck to your abdomen. It consists of 12 vertebrae and is the only section of the spine attached to the rib cage, which gives it incredible stability. While RA typically affects the more mobile cervical spine (your neck), it can, in rare cases, cause inflammation in the joints of the thoracic spine. When this occurs, the inflammation can lead to pain and stiffness in your mid-back and may even affect your chest and breathing due to its connection to the ribs.
Why This Area is Less Commonly Affected
The main reason RA is less common in the thoracic spine is its structure. This part of your back is much more rigid and stable compared to your flexible neck and lower back; it’s built for support, not a wide range of motion. Since RA tends to affect more mobile joints, the sturdy nature of the thoracic spine makes it a less likely target. However, "less likely" doesn't mean impossible. Because it is so rare, symptoms here can be mistaken for simple back pain, making a proper diagnosis crucial for getting the right care.
What Are the Symptoms of RA in the Thoracic Spine?
Recognizing the signs of rheumatoid arthritis in your mid-back is the first step toward getting the right support. While RA is famous for affecting the hands and feet, it can also target the thoracic spine, leading to a unique set of symptoms. These signs often develop gradually and can be mistaken for general back problems, so paying close attention to what your body is telling you is key. Understanding these specific symptoms can help you have a more productive conversation with your healthcare provider and start exploring effective, non-invasive treatment options.
Back Pain and Stiffness
One of the most common indicators of RA in the thoracic spine is a persistent, aching pain in your middle or upper back. This isn't like the sharp pain from a pulled muscle; it's often a deep, chronic discomfort that can feel worse after periods of rest. You might also experience significant stiffness that makes it difficult to bend, twist, or even stand up straight. While it's more common for RA to affect the neck, it can cause issues in the thoracolumbar spine, sometimes leading to serious complications like pathological fractures if the inflammation is severe.
Morning Stiffness and Limited Movement
If you wake up feeling like the Tin Man, you know how frustrating morning stiffness can be. For people with RA, this isn't just a minor inconvenience. A key sign of the condition is stiffness that lasts for more than an hour after you wake up or after you’ve been sitting for a while. When RA affects your thoracic spine, this stiffness can severely limit your range of motion, making it a challenge to get your day started. You might find it hard to rotate your torso or take a deep breath because the joints in your mid-back feel locked up.
Swelling and Tenderness
While the visible, "spongy" swelling common in hands and wrists is rare in the thoracic spine, the underlying inflammation is still at play. Instead of obvious swelling, you're more likely to feel tenderness in your mid-back. The area might feel sore or sensitive to the touch, especially if you press on the vertebrae. This tenderness is a direct result of the immune system attacking the synovial lining of the facet joints in your spine. Even without visible signs, this internal inflammation is what causes the pain and stiffness you feel.
A Grinding Sensation When You Move
Have you ever noticed a "creaky" or grinding feeling in your back when you twist or bend? This sensation, known as crepitus, can be a symptom of spinal arthritis. It happens when the protective cartilage in your spinal joints wears down from chronic inflammation, causing the bones to rub against each other. While it might just be an odd noise at first, it’s a sign that the joints in your thoracic spine are experiencing damage. This symptom often accompanies pain and can contribute to the feeling of stiffness and limited mobility in your back.
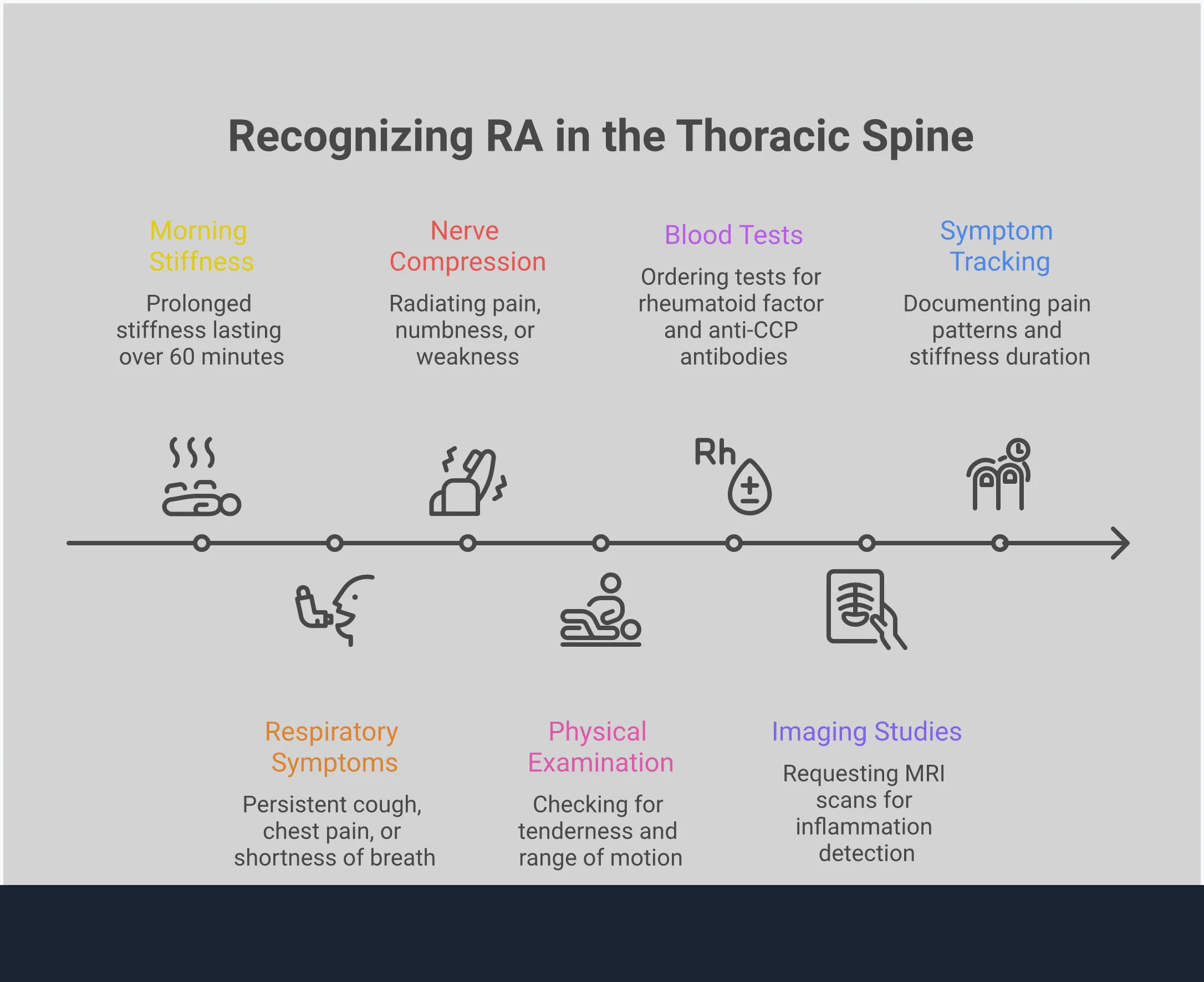
What Chest and Lung Symptoms Should You Watch For?
When you think about rheumatoid arthritis, joint pain is probably the first thing that comes to mind. But since RA is a systemic disease, its inflammatory effects can show up in surprising places, including your chest and lungs. This happens because the thoracic spine is directly connected to your rib cage, which protects these vital organs. Inflammation can spread from the spinal joints to the surrounding tissues, leading to a range of respiratory symptoms that are important to recognize.
These symptoms can be subtle and are often mistaken for other issues like asthma or a common cold. Knowing what to look for can help you and your doctor connect the dots sooner. Managing the underlying inflammation is key to protecting not just your joints, but your entire body. Our approach to pain management focuses on reducing inflammation at its source to help you feel and move better. Paying attention to these signs is a critical part of a proactive approach to your health.
A Persistent Cough or Wheezing
It’s easy to dismiss a cough or a bit of wheezing as allergies or the lingering effects of a cold. But if you have RA and these symptoms just won’t go away, it could be a sign of inflammation in your lungs. RA can cause inflammation in the small airways, a condition known as bronchiolitis, which narrows the passages and makes it harder for air to move through. This can trigger a chronic, nagging cough that might be dry or produce phlegm. You might also notice a whistling sound when you breathe. If a cough sticks around for weeks without a clear cause, it’s worth discussing with your doctor.
Chest Pain
Chest pain is always a symptom to take seriously. With RA, it can be caused by inflammation of the pleura, the thin tissue that lines the outside of your lungs and the inside of your chest cavity. This condition, called pleurisy, often causes a sharp, stabbing pain that gets worse when you take a deep breath, cough, or sneeze. Sometimes, fluid can build up in the space between these layers (a pleural effusion), creating a feeling of pressure or heaviness in your chest. While there are many causes of chest pain, linking it to your RA is an important possibility to consider with your healthcare provider.
Shortness of Breath
Feeling winded after climbing a flight of stairs might not seem like a big deal, but shortness of breath is one of the most common lung-related symptoms of RA. It can start gradually, happening only when you exert yourself, but it may progress over time. This can be a result of several RA-related issues, including inflammation, fluid around the lungs, or even scarring of the lung tissue itself. This scarring, called interstitial lung disease, makes the lungs stiff and less efficient at transferring oxygen to your bloodstream. Taking steps toward preventative wellness can help manage the systemic inflammation that contributes to these issues.
Fever and Respiratory Issues
A low-grade fever is your body’s classic response to inflammation and infection. When you have RA, your immune system is already working overtime, and a fever can signal that the inflammation is particularly active. If you develop a fever alongside chest pain, a cough, or shortness of breath, it’s a clear sign that something is going on with your respiratory system. It could indicate pleurisy or another inflammatory process in your lungs. While a fever isn’t always present with RA-related lung issues, its appearance with other respiratory symptoms should prompt an immediate call to your doctor to figure out the cause.
Lung Nodules
The idea of having nodules in your lungs can sound alarming, but in the context of RA, they are often not as scary as they seem. These rheumatoid lung nodules are small, firm lumps of tissue that can form in the lungs. In most cases, they don't cause any symptoms and are discovered by chance on a chest X-ray or CT scan done for another reason. However, it's important for your doctor to monitor them. In rare cases, larger nodules can rupture, which can lead to serious complications like a collapsed lung. Regular check-ups help ensure that any changes are caught early.
How is RA in the Thoracic Spine Diagnosed?
Getting a clear diagnosis for rheumatoid arthritis in the thoracic spine can feel like putting together a puzzle. Because the symptoms often overlap with other conditions, your doctor will use a combination of methods to get a full picture of what’s going on. It’s a process of gathering clues, from your personal health story to detailed images of your spine. This comprehensive approach ensures they can pinpoint the cause of your discomfort and create the right treatment plan for you.
Physical Exam and Medical History
Your diagnostic journey will start with a conversation. Your doctor will ask about your symptoms, when they started, and how they affect your daily life. They’ll also review your complete medical history to understand your overall health. A physical exam is the next step. Your doctor will gently press on your mid and upper back to check for tenderness, swelling, or warmth. They will also assess your range of motion, asking you to bend and twist to see if your movement is limited or causes pain. This initial evaluation helps rule out other potential causes and guides which tests to order next.
Blood Tests
To get a better look at what’s happening inside your body, your doctor will likely order blood tests. These tests search for specific markers of inflammation and antibodies associated with RA, such as the rheumatoid factor (RF). It’s important to know that these tests aren’t always definitive. Some people with RA have normal blood work, while others without the condition can test positive for these antibodies. Think of blood tests as an important piece of evidence, but not the whole story. They provide valuable information that, when combined with other findings, helps confirm a rheumatoid arthritis diagnosis.
Imaging Tests (X-Rays, MRI, CT Scans)
Imaging tests allow your doctor to see the joints, bones, and soft tissues in your thoracic spine. An X-ray is often the first step and can reveal any joint damage or bone erosion that has already occurred. However, for a closer look at earlier stages of the disease, your doctor might order an MRI or an ultrasound. These scans are much better at detecting soft tissue inflammation and swelling before significant joint damage is visible. Identifying inflammation early is key to managing symptoms and slowing the progression of RA, which is a core focus of our pain management therapies.
Lung Scans and Function Tests
Because RA can sometimes affect the lungs, especially when the thoracic spine is involved, your doctor may recommend tests to check your respiratory health. If you’ve been experiencing a persistent cough, shortness of breath, or chest pain, these tests are particularly important. A chest X-ray or CT scan can look for any inflammation or nodules in the lungs. Pulmonary function tests, which involve breathing into a special machine, measure how well your lungs are working. This helps your doctor understand if your breathing issues are connected to RA and ensures your treatment plan addresses your whole body.
What Are the Risks of Thoracic Spine RA?
Understanding the potential complications of rheumatoid arthritis in your thoracic spine is a key step in protecting your long-term health. While it’s a less common area for RA to affect, the risks are significant and can impact your bones, nerves, and even your breathing. Being aware of these possibilities allows you to work with your healthcare team on a proactive plan to manage your symptoms and maintain your quality of life.
Vertebral Fractures
The persistent inflammation from RA can gradually weaken the bones in your spine. Over time, this can make the vertebrae in your thoracic region more susceptible to what are known as pathological fractures. This means the bone can break or even collapse under normal stress, not just from a major injury. In one documented case, a woman with RA experienced severe back pain that was ultimately caused by several of these fractures in her mid-back. This risk highlights the importance of monitoring your bone health and managing inflammation effectively to keep your spine strong and stable.
Spinal Instability and Nerve Issues
RA doesn't just affect the bones; it targets the joints and connective tissues that keep your spine aligned. Inflammation can damage the small facet joints that allow your spine to bend and twist, or the areas where your discs connect to the vertebrae. This damage can lead to spinal instability, where the vertebrae shift out of their proper position. When this happens, it can put pressure on your spinal cord or the nerves branching out from it. This nerve compression can cause radiating pain, numbness, tingling, or weakness in your back, chest, or abdomen. Addressing this instability is crucial for preventing long-term nerve damage and managing your pain.
Chronic Pain and Reduced Mobility
The combination of joint inflammation, bone damage, and potential nerve compression can result in persistent, chronic pain. This isn't just a minor ache; it can be a debilitating symptom that makes it difficult to perform daily activities like bending, lifting, or even just sitting comfortably for long periods. This ongoing pain often leads to a significant reduction in mobility as your body tries to protect itself by limiting movement. Finding effective ways to manage your pain and inflammation is essential for breaking this cycle, improving your mobility, and reclaiming your ability to enjoy an active life.
Worsening Breathing Problems
Your thoracic spine is directly connected to your rib cage, which expands and contracts every time you breathe. When RA causes pain and stiffness in this area, it can restrict your rib cage’s movement, making it difficult to take deep breaths. Beyond this mechanical issue, RA is a systemic disease that can cause inflammation throughout the body. Lung problems are a serious and surprisingly common complication of RA, sometimes occurring without obvious symptoms. This makes it incredibly important to pay attention to any changes in your breathing, like shortness of breath or a persistent cough, and discuss them with your doctor right away.
What Are the Common Medical Treatments?
When you're dealing with rheumatoid arthritis in your thoracic spine, your doctor’s main goal is to create a plan that slows the disease down, manages your symptoms, and keeps you moving comfortably. This isn't about a single quick fix; it's about finding the right combination of treatments that work for your body. Think of it as building a personalized toolkit to help you feel your best. The approach is often layered, starting with medications to control the underlying inflammation and adding supportive therapies to manage pain and maintain your mobility.
Your healthcare team will work with you to figure out the best path forward. This plan will likely evolve as your needs change. The primary objectives are to reduce inflammation, prevent or slow down joint damage, relieve pain, and improve your overall quality of life. It’s a proactive partnership focused on keeping you active and in control. Let's walk through some of the most common medical treatments your doctor might discuss with you, from foundational medications to therapies that support your movement and strength.
Medications like DMARDs and Biologics
The first line of defense against RA is typically a group of drugs called disease-modifying antirheumatic drugs (DMARDs). Unlike standard pain relievers, these medications get to the root of the problem by calming your overactive immune system. Their main job is to slow the progression of RA and help prevent permanent damage to your joints. A newer, more targeted class of DMARDs, known as biologics, works by pinpointing specific immune system signals that trigger inflammation. Your rheumatologist will help you understand if these medications are a good fit, as they can be incredibly effective at getting the disease under control.
Pain Relievers and Steroids
To help you manage the day-to-day pain and swelling that can come with an RA flare-up, your doctor will likely recommend over-the-counter pain relievers like ibuprofen. These can be very helpful for taking the edge off and reducing mild inflammation so you can go about your day more comfortably. For more intense flare-ups, your doctor might prescribe a short course of corticosteroids. These are powerful anti-inflammatory drugs that act quickly to suppress your immune response and provide fast relief from severe symptoms. Because of potential side effects, they are generally used as a short-term solution to get a serious flare under control.
Physical Therapy
Physical therapy is a vital and empowering part of managing RA in your spine. A skilled physical therapist will design a personalized program just for you, focusing on safe and effective ways to move. The goal is to strengthen the muscles that support your back, improve your flexibility, and help you maintain your range of motion without causing more pain. It’s about learning how to work with your body, not against it. Consistent physical therapy can make a huge difference in your daily comfort and long-term mobility, helping you stay active and confident. These thoracic spine stretches are a great example of gentle movements that can help.
Surgery as a Last Resort
Surgery is rarely the first step for treating RA in the thoracic spine. It’s typically considered a last resort, reserved for situations where other treatments haven't provided enough relief and there's a risk of serious complications. If chronic inflammation has led to severe joint damage, causing spinal instability or putting pressure on your nerves, an operation may be necessary to fix the structural problem. Your doctor would only recommend this path if your symptoms are severely impacting your quality of life or posing a risk to your neurological health. The main goals of surgery are to stabilize the spine, relieve nerve compression, and reduce pain.
How Can Natural Therapies Support Your Treatment?
While medical treatments are essential for managing rheumatoid arthritis, incorporating natural therapies into your routine can make a significant difference in your daily comfort and overall well-being. Think of these strategies as powerful allies that work alongside your prescribed care plan. They can help you feel more in control of your health by addressing symptoms like pain, stiffness, and inflammation from a holistic perspective.
From targeted light therapy to simple lifestyle adjustments, these approaches focus on supporting your body’s natural ability to heal and function. By combining these methods with your doctor's recommendations, you can build a comprehensive care plan that addresses your unique needs. This integrated approach is key to managing symptoms effectively and improving your quality of life. Exploring options for preventative wellness can also help you maintain long-term health and reduce the impact of chronic conditions.
Light Therapy to Reduce Pain and Inflammation
If you’re dealing with the persistent pain and morning stiffness of RA, light therapy can be a game-changer. This non-invasive treatment uses specific wavelengths of light to penetrate the skin and stimulate your cells. Research shows that red light therapy can be an effective short-term treatment for reducing the pain and inflammation associated with arthritis. It works by helping to decrease swelling in the joints and providing relief without medication or invasive procedures. Adding light therapy to your pain management strategy can help you find comfort and get back to your daily activities with greater ease.
Gentle Movement to Improve Mobility
When your joints are stiff and sore, moving more might be the last thing on your mind. However, gentle, consistent movement is crucial for managing RA. Activities like stretching and low-impact exercises help maintain joint function and improve your range of motion. Regular physical activity fights the stiffness that can make mornings so difficult. You don’t have to run a marathon; simple, mindful movements can keep your joints lubricated and your muscles strong. This focus on mobility is a core part of any effective performance recovery plan, helping your body stay resilient and functional.
Holistic Wellness for Overall Health
Managing a chronic condition like RA goes beyond just treating physical symptoms. A holistic approach that includes stress management and good nutrition can have a profound impact on your overall health. Chronic stress can worsen inflammation, so finding healthy ways to cope, like meditation or deep breathing, is incredibly beneficial. Similarly, an anti-inflammatory diet rich in fruits, vegetables, and healthy fats can support your body from the inside out. Taking care of your whole self, not just your joints, helps you build a stronger foundation for managing your RA symptoms and feeling your best.
Lifestyle Changes for Better Breathing
Because RA in the thoracic spine can affect your chest and lungs, making positive lifestyle changes is especially important. Maintaining a healthy weight reduces the strain on your entire skeletal system, including your spine, which can ease pain and improve breathing mechanics. If you smoke, quitting is one of the most impactful things you can do for your respiratory and overall health. These adjustments help reduce the burden on your thoracic spine and support better lung function, allowing you to breathe more freely and comfortably.
When Should You See a Doctor Immediately?
While managing rheumatoid arthritis often involves a long-term strategy of care, some symptoms are red flags that require immediate medical attention. Think of it this way: your day-to-day management plan is for the marathon, but these symptoms are sprints straight to your doctor's office. Ignoring them can lead to more serious complications, so it’s important to know what to look for. If you experience any of the following, don't wait for your next scheduled appointment. Call your doctor or seek urgent care to get a clear diagnosis and prevent further issues.
Sudden, Severe Back Pain
If you suddenly experience intense, sharp pain in your back that feels different from your usual RA discomfort, it’s time to call a doctor right away. This isn't the kind of ache you can stretch out or ignore until morning. Severe pain could signal a significant issue, like a vertebral fracture or acute inflammation that needs immediate assessment. Research suggests that RA in the mid and lower back may be more common than once thought, and doctors often recommend X-rays or other scans to investigate sudden back pain in RA patients. Getting a prompt evaluation is key to protecting your spine from further damage.
Worsening Nerve Symptoms
Pay close attention to any new or worsening nerve-related symptoms. This includes pain that radiates from your back into other parts of your body, such as your hips, legs, or even your ribs. You might also feel numbness, tingling, or weakness in your limbs. These sensations often indicate that inflammation or changes in your spine are beginning to compress or irritate your nerves. According to the Cleveland Clinic, this type of spreading pain is a common symptom of spinal arthritis. Don't brush it off as a minor annoyance; nerve issues can become serious if left unaddressed.
Trouble Breathing
Any difficulty breathing should always be taken seriously. If you notice new or worsening shortness of breath, chest pain, or a persistent cough, seek medical help immediately. Lung issues can be a significant complication of rheumatoid arthritis, and your thoracic spine’s proximity to your rib cage and lungs means problems in one area can affect the other. Studies show that thoracic manifestations of RA can be quite serious, so it's crucial to have any respiratory symptoms checked out by a professional to rule out or treat underlying problems.
Signs of an Unstable Spine
An unstable spine occurs when your vertebrae are no longer properly supported, which can happen if RA weakens the surrounding joints and bones. You might feel like your back is "giving way," or you could experience severe pain when you change positions. Sometimes, RA can cause inflammatory cells to form in the bone marrow, which can weaken the bone and even lead to collapse. If you feel a sense of instability in your back or notice any sudden changes in your posture accompanied by pain, it’s a clear sign you need an urgent medical evaluation. After you've seen a doctor, we can help you create a supportive care plan for your pain management.
Build Your Comprehensive Care Plan
Managing rheumatoid arthritis in your thoracic spine requires a thoughtful and proactive approach. It’s not about finding a single solution, but about creating a sustainable strategy that combines the best of medical science with supportive natural care. Think of it as building a personal wellness toolkit with your healthcare providers. A comprehensive plan empowers you to address symptoms from multiple angles, giving you more control over your health and helping you maintain your quality of life. This involves integrating different therapies, working closely with your medical team, and staying committed to long-term monitoring to keep your plan effective and responsive to your body’s needs. By taking charge of your care, you can build a routine that not only manages pain but also supports your overall health, helping you stay active and engaged in the things you love. The goal is to create a balanced, multi-faceted approach that feels right for you. It’s about feeling empowered and informed every step of the way, knowing you have a solid plan in place to handle whatever comes your way.
Integrate Medical and Natural Therapies
While there isn't a cure for RA, a combination of treatments can make a significant difference in managing your symptoms. Your doctor will likely recommend a foundation of medical care, which may include medications and physical therapy. Alongside these conventional treatments, you can incorporate natural therapies to support your body. For instance, non-invasive light therapy is an excellent way to complement your existing plan. It can help reduce inflammation and ease discomfort, offering a drug-free option for pain management. By integrating these approaches, you create a more holistic strategy that addresses both the disease and your overall well-being.
Partner with Your Healthcare Team
Your relationship with your healthcare providers is one of the most important tools you have. A successful treatment plan begins with a thorough evaluation, where your doctor reviews your symptoms and health history to understand your specific situation. Be an active participant in this partnership. Ask questions, share your concerns, and always report new or changing symptoms, especially any related to your breathing. Open communication ensures your care plan is tailored to you and can be adjusted as your needs change. This collaborative approach helps you and your team make informed decisions together.
Focus on Long-Term Monitoring and Prevention
Managing a chronic condition like RA is a marathon, not a sprint. Consistent, long-term monitoring is key to staying ahead of symptoms and potential complications. Regular check-ups allow your doctor to track your progress, monitor for issues like lung involvement, and make timely adjustments to your treatment. This proactive approach is a core part of preventative wellness. By staying vigilant and committed to your care plan, you can better protect your spinal health and mobility, ensuring you feel and move your best for years to come.
Frequently Asked Questions
How can I tell if my mid-back pain is from RA or just a regular backache? Distinguishing between the two can be tricky, but there are key differences. A typical backache might feel sharp and is often linked to a specific activity or injury. RA pain, on the other hand, tends to be a deep, persistent ache. A major clue is significant morning stiffness that lasts for an hour or more. If your mid-back feels incredibly stiff and locked up when you wake up, and this is paired with tenderness or a grinding sensation when you move, it’s a strong signal to talk with your doctor about the possibility of an inflammatory condition.
If RA in the thoracic spine is so rare, why is it important to know about? Because it's uncommon, the symptoms are often mistaken for more ordinary back problems, which can delay a correct diagnosis. Understanding the possibility allows you to have a more informed conversation with your doctor. The thoracic spine’s connection to the rib cage means that inflammation here can lead to serious complications, including breathing difficulties and nerve issues. Being aware of the risks helps you and your healthcare team take a proactive approach to protect not just your spine, but your overall health.
Can lifestyle changes like diet and exercise really help with an autoimmune disease? Absolutely. While they aren't a substitute for medical treatment, lifestyle choices are a powerful part of your management plan. Gentle movement, like stretching, helps maintain flexibility and reduces the stiffness that makes daily activities difficult. Similarly, focusing on an anti-inflammatory diet and managing stress can help calm your body's overall inflammatory response. These habits support your medical care, giving you more control over your well-being and helping you feel better day-to-day.
Is light therapy a standalone treatment for this condition? Light therapy is best viewed as a supportive and complementary part of your comprehensive care plan, not a standalone cure. It works wonderfully alongside the treatments prescribed by your doctor, like medication and physical therapy. Its main role is to provide non-invasive, drug-free relief by reducing localized pain and inflammation. Think of it as a powerful tool in your toolkit for managing daily symptoms and improving your comfort.
My doctor diagnosed me. What's the most important first step I should take? The most important first step is to build your healthcare team and create a partnership. Your rheumatologist will guide your medical treatment, but you are the central player. Start by asking questions to fully understand your treatment plan and then work on integrating supportive therapies that feel right for you. Open communication is key; always report new or changing symptoms. This collaborative approach ensures your care plan is tailored to your needs and empowers you to manage your health proactively.
Frequently Asked Questions
Is light therapy safe for athletes?

Yes, light therapy is completely safe and highly beneficial for athletes. It promotes faster muscle recovery, reduces inflammation, and supports performance without the risks of medication or downtime. That’s why professional and amateur athletes worldwide rely on it to train smarter and recover quicker.
How many sessions will I need?

The number of sessions varies depending on the type and severity of your condition. Many patients notice improvement after 3–5 sessions, while chronic conditions may require ongoing care for best results. During your initial consultation, we’ll design a personalized treatment schedule tailored to your body’s response and recovery goals.




