
Psoriatic Arthritis Sciatica: Causes & Treatment
That sharp, shooting pain down your leg is often blamed on a herniated disc pinching your sciatic nerve. But what if the real culprit isn’t a mechanical issue at all? For those living with psoriatic arthritis, the source of that debilitating nerve pain might be the underlying inflammation from your autoimmune condition. When your immune system attacks the joints in your lower spine and pelvis, the resulting swelling can irritate the sciatic nerve, perfectly mimicking classic sciatica. This guide explores the often-overlooked link between psoriatic arthritis sciatica. We’ll help you understand the difference between inflammatory and mechanical pain and show you how targeting the inflammation can lead to real, sustainable relief from that radiating pain.
Key Takeaways
- Psoriatic arthritis can mimic sciatica: The radiating leg pain you feel might not be from a pinched nerve but from inflammation in your lower back or pelvic joints, a common issue with psoriatic arthritis that irritates the sciatic nerve.
- Identify the type of pain you're feeling: Inflammatory pain from psoriatic arthritis typically feels worse after rest, like in the morning, and gets better with activity. Recognizing this pattern is a key step toward getting an accurate diagnosis from a professional.
- Combine medical care with lifestyle changes: Effective management involves more than just medication. A holistic plan that includes natural therapies like light therapy, gentle exercises, and an anti-inflammatory diet can help reduce symptoms and improve your overall quality of life.
Psoriatic Arthritis and Sciatica: What's the Connection?
If you're dealing with the sharp, radiating pain of sciatica along with the joint stiffness of psoriatic arthritis, you might be wondering if they're related. It’s a valid question, and the answer is more complex than a simple yes or no. While psoriatic arthritis (PsA) doesn't directly cause sciatica in the classic sense (like a herniated disc), the widespread inflammation it creates can certainly lead to sciatica-like symptoms. The inflammation can irritate nerves and cause pain that feels identical to sciatica. Let's break down how these two conditions are connected.
First, What Is Psoriatic Arthritis?
Psoriatic arthritis, or PsA, is a type of inflammatory arthritis that affects some people who have psoriasis, a skin condition that causes itchy, scaly patches. For most people, the skin condition appears first, sometimes years before any joint issues begin. As an autoimmune disease, PsA occurs when your body's immune system mistakenly attacks healthy cells and tissues. This immune response causes inflammation in your joints, leading to pain, stiffness, and swelling. While it can affect any part of the body, PsA commonly appears in the fingers, toes, knees, and spine. Understanding that PsA is a systemic inflammatory condition is key to seeing how it can cause problems far beyond the joints themselves.
How PsA Can Affect Your Spine and Nerves
While many people associate PsA with pain in their hands and feet, it can also target the spine. When this happens, it's called axial arthritis or spondylitis. A common issue for people with PsA is sacroiliitis, which is inflammation of the sacroiliac (SI) joints that connect your pelvis and lower spine. A significant number of people with PsA experience this. The inflammation in the SI joints can cause pain that radiates from your lower back, through your buttocks, and down your leg. This pattern of pain feels almost identical to classic sciatica, which is a primary reason why the two conditions are so often linked.
Why Inflammation Leads to Nerve Pain
The pain from PsA-related inflammation behaves differently than pain from a mechanical injury, like a pulled muscle. Inflammatory pain often feels worse after periods of rest (like first thing in the morning) and can actually improve with gentle movement and activity. This inflammation can also occur where tendons and ligaments attach to the bone, a condition called enthesitis. When this happens in your lower back or pelvis, the swelling can irritate nearby nerve roots, including the large sciatic nerve. It’s not a pinched nerve from a disc, but rather a nerve that’s aggravated by the inflammation surrounding it. Recognizing that inflammation is the root cause is the first step toward finding effective pain management strategies.
Is Your Sciatica Caused by Psoriatic Arthritis? Key Symptoms to Watch For
Figuring out the source of your pain is the first step toward finding relief. While sciatica is often linked to issues like a herniated disc, the radiating leg pain you’re feeling could be a sign of psoriatic arthritis (PsA). Because PsA is an inflammatory condition, the symptoms it causes are different from the mechanical pain you’d get from an injury.
Understanding these differences can help you have a more productive conversation with your doctor and get on the right path to treatment. If you’re experiencing sciatica-like symptoms along with joint pain or skin issues, it’s worth paying close attention to the specific signals your body is sending. Watch for these key signs that suggest your sciatica might be connected to PsA.
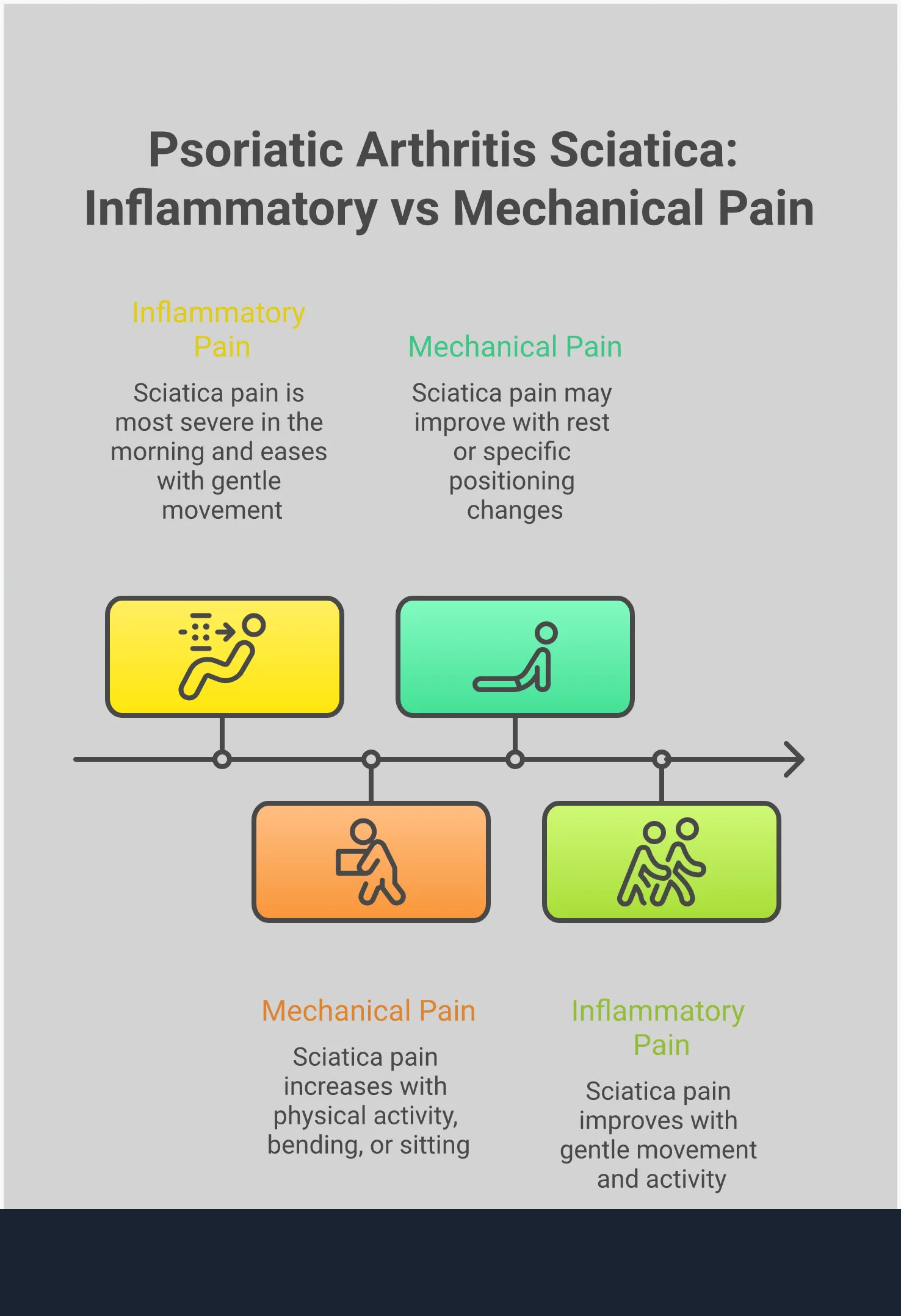
Inflammatory vs. Mechanical Pain: How to Tell the Difference
One of the biggest clues is how your pain behaves throughout the day. Mechanical back pain, the kind you get from lifting something heavy or sitting with poor posture, usually feels worse after activity and better with rest. Inflammatory back pain from PsA is often the exact opposite. You might find that the pain and stiffness are most intense when you first wake up or after you’ve been sitting for a long time. As you start to move around, the pain may actually improve. This type of pain can even be disruptive enough to wake you up in the middle of the night, which is less common with mechanical issues.
That Familiar Radiating Leg Pain
That sharp, shooting pain down your leg is the classic sign of sciatica, but when PsA is the cause, it starts with inflammation in your sacroiliac (SI) joints. These joints connect your lower spine to your pelvis. When they become inflamed, a condition called sacroiliitis, the pain can radiate down into your buttocks and legs, mimicking sciatica perfectly. For many people with axial PsA, which primarily affects the spine, the SI joints are one of the first areas to show signs of trouble. This is why effective pain management starts with identifying the true source of the inflammation.
Stiffness in the Morning That Eases with Movement
Do you feel like the Tin Man when you first get out of bed? Significant morning stiffness that lasts for more than 30 minutes is a hallmark of inflammatory arthritis, including PsA. With mechanical back pain, you might feel a little stiff for a few minutes, but it usually resolves quickly. With PsA, the stiffness can be intense and persistent, making it hard to bend over or get your day started. The good news is that this stiffness often gets better with gentle movement and activity. If a warm shower and some light stretching are essential for you to feel functional in the morning, inflammation could be the underlying issue.
Pain Centered in Your Hips or Buttocks
While sciatica can cause pain anywhere along the nerve path, PsA-related pain is often centered in the lower back, hips, or buttocks. The sensation can vary from person to person, feeling like a sharp, stabbing pain or a constant, dull ache. You might notice it gets worse after you’ve been sitting or standing for a while. That moment when you stand up after being seated for a long time can be particularly painful. This localized pain is a direct result of the inflammation in the sacroiliac joints, where the sciatic nerve is in close proximity.
How Psoriatic Arthritis Triggers Sciatica-Like Pain
So, how does an autoimmune condition like psoriatic arthritis (PsA) cause pain that feels so much like sciatica? It’s not that PsA directly causes sciatica, but the inflammation it creates can mimic the symptoms. The pain shooting down your leg might not be from a herniated disc, but from inflamed joints irritating the nerves in your lower back. The root cause isn't a mechanical issue but a systemic inflammatory one. When your immune system attacks your joints, the resulting inflammation can create nerve pain that travels the same path as sciatica. Understanding this is key to getting the right diagnosis.
When Inflamed Joints Pinch Your Nerves
A common culprit behind PsA-related sciatica is inflammation in the sacroiliac (SI) joints, which connect your lower spine to your pelvis. When these joints become inflamed, a condition known as sacroiliitis, it can cause pain in your lower back, buttocks, and hips. Because the sciatic nerve runs right past these joints, the swelling can put pressure on it. This pressure triggers that familiar radiating pain down your leg, making you think you have classic sciatica. The pain originates from joint inflammation, not a spinal disc problem.
How PsA Can Affect Your Spine Directly
Sometimes, psoriatic arthritis targets the spine itself in a condition called axial arthritis or spondylitis. This causes inflammation in the vertebrae, and when your lower spine is affected, the pain and stiffness can easily be confused with sciatica. However, there’s a key difference: inflammatory back pain from PsA usually feels worse in the morning or after inactivity. Gentle movement tends to ease the stiffness. This tells you that inflammation, not injury, is the source of the problem, which requires a different approach to pain management.
Clearing Up Common Myths About PsA and Sciatica
It’s easy to assume all sciatic nerve pain comes from a pinched nerve, but that’s a common myth when PsA is involved. The crucial difference is inflammation versus a mechanical problem. True sciatica is mechanical; something is physically pressing on the nerve. With PsA, the pain is driven by your body’s inflammatory response. This distinction is vital because the treatments are completely different. While physical therapy might help a herniated disc, it won’t stop the autoimmune process causing your joint inflammation. An accurate diagnosis ensures you’re targeting the inflammation at its source.
How Do Doctors Diagnose Psoriatic Arthritis-Related Sciatica?
Figuring out if your sciatica is linked to psoriatic arthritis isn't a one-step process. Because the symptoms can mimic other conditions, like a herniated disc, your doctor will act like a detective, gathering clues from different sources to get a clear picture of what’s happening inside your body. This usually involves a combination of a physical exam, imaging tests, and blood work to connect the dots between your nerve pain and PsA. Getting an accurate diagnosis is the most important step toward finding a pain management plan that truly works for you.
What to Expect During Your Physical Exam
Your appointment will start with a conversation. Your doctor will ask about your symptoms, your personal and family health history, and what your pain feels like. Be ready to describe when the pain occurs and what makes it better or worse. They’ll pay close attention if you mention morning stiffness that eases with movement, as that’s a classic sign of inflammatory arthritis. Next, they’ll perform a physical exam, gently pressing on your joints to check for tenderness and swelling, especially around your spine and hips. They will also assess your range of motion to see how well you can move.
A Closer Look: Imaging Tests like MRI and X-Rays
To see what’s going on with your bones and soft tissues, your doctor will likely order imaging tests. X-rays are great for revealing any long-term changes or damage to the bones in your spine and sacroiliac (SI) joints, which connect your spine to your pelvis. For a more detailed view, they may order an MRI. This scan can show inflammation in the soft tissues, cartilage, and joints before any permanent damage occurs. Imaging is crucial because it helps your doctor see direct evidence of sacroiliitis (inflammation of the SI joints) and rule out other common causes of sciatica, like disc issues.
Using Blood Tests to Spot Inflammation
While there isn't a specific blood test that can definitively diagnose psoriatic arthritis, lab work provides important clues. Your doctor may order tests to check for general markers of inflammation in your body, such as C-reactive protein (CRP) and erythrocyte sedimentation rate (ESR). Elevated levels of these markers suggest an inflammatory process is happening. Blood tests are also incredibly useful for ruling out other conditions. For example, testing for rheumatoid factor (RF) can help distinguish PsA from rheumatoid arthritis, as most people with PsA test negative for this antibody.
Making Sure It's Not Something Else
Connecting sciatica to PsA requires looking at your health as a whole. Your doctor will carefully consider any other symptoms you have, especially those related to psoriasis. They’ll look for skin lesions, particularly on the scalp or in less visible areas, and check your fingernails and toenails for signs of pitting or separation from the nail bed. These symptoms are strong indicators that psoriatic arthritis could be the root cause of your joint and nerve pain. This comprehensive approach ensures that other potential issues are ruled out, leading to a more accurate diagnosis and a more effective treatment plan. It reflects a commitment to holistic care that addresses the complete picture.
Effective Medical Treatments for PsA-Related Sciatica
When you're dealing with the double challenge of psoriatic arthritis and sciatica, your doctor will likely focus on a two-part goal: easing your immediate pain and addressing the underlying inflammation to prevent long-term damage. The right approach depends on how severe your symptoms are and how your body responds. Medical treatments are often the first step in getting the condition under control so you can start feeling better.
These treatments typically involve medications that reduce inflammation throughout your body, which in turn can relieve the pressure on your sciatic nerve. Your healthcare provider will work with you to find the best fit, often starting with simpler options and adjusting as needed. It’s all about creating a plan that manages your symptoms while slowing down the progression of the disease.
Managing Pain with NSAIDs
For milder sciatic pain caused by PsA, your doctor will probably suggest starting with nonsteroidal anti-inflammatory drugs, or NSAIDs. You’re likely already familiar with these over-the-counter options, which include ibuprofen (Advil, Motrin) and naproxen (Aleve). They work by reducing inflammation and offering temporary pain relief. While they don't stop the disease from progressing, they can be very effective for managing day-to-day discomfort and stiffness. Think of them as the first line of defense to help you get through a flare-up and stay active. If these don't provide enough relief, your doctor will likely explore stronger options.
Slowing the Disease with DMARDs and Biologics
If NSAIDs aren't cutting it, or if your PsA is more moderate to severe, your doctor may prescribe medications designed to slow the disease itself. These are called disease-modifying antirheumatic drugs (DMARDs). A specific type of DMARD, known as a biologic, is often used for PsA that affects the spine. These drugs, like TNF inhibitors, are highly targeted. They work by blocking specific proteins in your immune system that cause inflammation. By calming the underlying autoimmune response, biologic medicines can prevent further joint damage and provide significant relief from sciatica and other PsA symptoms.
Targeted Relief with Corticosteroid Injections
When inflammation is concentrated in a specific area, like the sacroiliac joints in your lower back, a corticosteroid injection can offer powerful, targeted relief. During this procedure, a doctor injects a strong anti-inflammatory medication directly into the inflamed joint. This can quickly reduce swelling and pain right at the source, calming the irritation around the sciatic nerve. These injections aren't a long-term solution, but they can be incredibly helpful for breaking a cycle of intense pain and inflammation, giving you the relief needed to participate in physical therapy or other treatments.
Why Timing and Monitoring Your Treatment Matters
With PsA, acting quickly is key. Research shows that waiting even six months to start effective treatment can lead to permanent joint damage. That's why it's so important to talk to your doctor as soon as you notice symptoms like back pain or morning stiffness. Your treatment plan for PsA affecting the spine is different from other types of PsA, so clear communication helps your doctor make an early diagnosis and get you on the right path. Regularly checking in with your healthcare team allows them to monitor your progress, adjust medications, and ensure your treatment plan is working as effectively as possible.
Find Natural Relief with Light Therapy
If you’re looking for a way to manage psoriatic arthritis and sciatica without relying solely on medication or invasive procedures, light therapy is a powerful option to consider. This approach uses specific wavelengths of light to work with your body’s natural healing processes. It’s a gentle, non-invasive way to address both the pain and the underlying inflammation that come with PsA-related sciatica.
Think of it as giving your cells the energy they need to repair themselves and function better. Instead of just masking symptoms, light therapy gets to the source of the problem, helping to calm inflammation, ease pain, and support your body’s recovery. It’s not about replacing your current medical treatments but rather adding another effective tool to your wellness toolkit. By integrating light therapy into your routine, you can create a more comprehensive plan for managing your symptoms and improving your quality of life. It’s a safe, drug-free way to find relief and feel more in control of your health.
Calm Inflammation at the Source
Psoriatic arthritis and the sciatica it can trigger are fundamentally driven by inflammation. When your immune system is overactive, it creates a cascade of inflammatory responses that lead to joint pain, stiffness, and nerve irritation. Light therapy offers a way to address this at a cellular level. It helps reduce pro-inflammatory markers in your body while increasing the anti-inflammatory ones. This process helps restore balance, calming the inflammation that’s causing your pain. By targeting the root cause, you can achieve more sustainable pain management instead of just temporarily covering up the symptoms.
Get Pain Relief Without Drugs or Surgery
For many people, the idea of long-term medication use or surgery is a major concern. Light therapy provides a safe and effective alternative for pain relief. As a completely non-invasive treatment, it uses targeted light to penetrate the skin and stimulate healing in the tissues below. This process can significantly reduce the pain signals sent to your brain, offering relief without the side effects that often come with prescription drugs. It’s a way to take an active role in your health journey, using a method that supports your body’s ability to heal itself naturally.
Help Your Body Heal and Recover Faster
Beyond just easing pain, light therapy actively promotes healing. For those with psoriatic arthritis, this is especially beneficial. Research shows that certain types of light therapy can help slow the rapid growth of skin cells associated with psoriasis, addressing one of the key features of the condition. This same healing energy helps repair damaged tissues around your spine and sciatic nerve, supporting faster performance recovery and reducing the frequency of flare-ups. It’s a holistic approach that helps your body mend from the inside out, leading to lasting improvements in both your skin and joint health.
How Light Therapy Complements Your Current Treatment
Adding light therapy to your routine doesn’t mean you have to abandon the treatments that are already working for you. In fact, it works beautifully alongside conventional medical care. You can think of it as a supportive therapy that enhances the effects of your current plan. Because it’s safe and has few side effects, it can easily be integrated to provide extra pain relief and reduce inflammation. Discussing light therapy with your healthcare provider can help you create a well-rounded strategy that gives you the best of both worlds: advanced medical treatment and natural, restorative care. You can learn more about our approach and how we can help you build a comprehensive plan.
Lifestyle Changes That Make a Real Difference
While medical treatments are essential for managing psoriatic arthritis and sciatica, your daily habits play a huge role in how you feel. Think of these lifestyle adjustments as powerful tools in your wellness toolkit. They work alongside professional care to reduce flare-ups, ease daily discomfort, and give you more control over your health. Making small, consistent changes to how you move, eat, and manage stress can create a strong foundation for long-term relief. These strategies aren't about a complete overhaul overnight; they're about building sustainable habits that support your body's ability to heal and help you feel your best.
Move Better with Gentle Stretches and Exercises
When you’re in pain, the last thing you might want to do is move, but gentle activity is one of the best things for your joints and nerves. Movement helps reduce stiffness, improve flexibility, and strengthen the muscles that support your spine and hips. This doesn't mean you need to run a marathon. Low-impact activities like walking, swimming, or gentle yoga can make a significant difference. The key is to listen to your body and find a routine that feels good. Regular, gentle physical activity can help ease the symptoms of both psoriatic arthritis and sciatica, making it easier to go about your day with less pain.
Try Nerve Glides to Soothe Your Sciatic Nerve
If you’re dealing with that distinct radiating pain from sciatica, nerve glides can be a game-changer. Think of them as a form of gentle flossing for your sciatic nerve. These specific exercises are designed to help the nerve move more freely through the surrounding tissues, which can reduce irritation and tension. By carefully mobilizing the nerve, you can help decrease pain and improve your range of motion. You can easily learn a few basic nerve glide exercises to do at home. Performing them slowly and gently can provide targeted relief and help calm down an aggravated sciatic nerve without putting extra strain on your body.
Eat to Fight Inflammation
The food you eat can either fuel inflammation or help fight it. For a condition like psoriatic arthritis, which is driven by inflammation, an anti-inflammatory diet can be a powerful tool. Focus on incorporating whole foods rich in antioxidants and healthy fats, like leafy greens, berries, salmon, and nuts. At the same time, try to limit processed foods, sugar, and red meat, which can make inflammation worse. You don’t have to change your entire diet overnight. Start by making small swaps, like adding a side of spinach to your dinner or choosing fruit for dessert. These simple dietary changes can help manage your symptoms from the inside out.
Manage Your Weight and Reduce Stress
Your weight and stress levels have a direct impact on joint pain and inflammation. Maintaining a healthy weight reduces the amount of pressure on your joints, especially in your back and hips, which can significantly lessen sciatic and arthritic pain. Even a small amount of weight loss can lead to a noticeable improvement in your symptoms. Similarly, managing stress is crucial, as stress hormones can trigger inflammatory flare-ups. Finding healthy ways to cope, whether through deep breathing, meditation, or a favorite hobby, can help keep your symptoms in check. These two factors work hand-in-hand to support your overall preventative wellness journey.
Create Your Comprehensive Treatment Plan
Managing psoriatic arthritis and sciatica isn't about finding a single magic bullet. Instead, the most effective approach is building a personalized, comprehensive plan that addresses your unique symptoms and goals. Think of it as assembling your own dedicated support system, with you as the team captain. This plan should combine the expertise of your medical providers with effective natural therapies and smart lifestyle adjustments. By taking an active role in your care, you can create a strategy that not only manages pain but also helps you feel more in control of your health. A well-rounded plan empowers you to tackle symptoms from all angles, leading to better, more sustainable results.
This means looking beyond just medication. It involves understanding how your diet, exercise habits, and stress levels affect your symptoms. It also means exploring therapies that work with your body’s natural healing processes to reduce inflammation and promote recovery. When you bring all these pieces together, you create a powerful synergy. Your medical treatments can work more effectively, and you’ll feel better equipped to handle flare-ups when they happen. This proactive approach ensures you're not just reacting to pain but are actively working toward long-term wellness and mobility, helping you get back to doing the things you love with confidence.
Partner with Your Healthcare Team
Your relationship with your healthcare provider is the foundation of your treatment plan. Open and honest communication is key, especially since the right approach depends on your specific symptoms. It's crucial to tell your doctor about everything you're experiencing, including back or neck pain, as the treatment for axial psoriatic arthritis (which affects the spine) is different from other forms of PsA. Don't hesitate to share how the pain impacts your daily life. To make the most of your appointments, try jotting down your questions and a list of your symptoms beforehand. This helps you have a productive conversation and work together to find the best path forward.
Integrate Medical and Natural Therapies
Many people with psoriatic arthritis are interested in adding complementary therapies to their medical treatments to support their overall well-being. Integrating natural, non-invasive options like light therapy can be a game-changer for effective pain management. Because it works by reducing inflammation at the cellular level, it can provide significant relief without drugs or surgery. This approach complements your doctor's recommendations, helping to ease pain and support your body’s healing processes. It’s a safe and proven way to enhance your care plan and improve your quality of life, giving you another tool in your toolkit for feeling your best.
Track Your Symptoms and Adjust as You Go
Living with a chronic condition means your symptoms can change from day to day. Keeping a simple journal or using an app to track your pain levels, stiffness, and potential triggers can provide invaluable insight. Note what makes you feel better and what makes you feel worse. This information is incredibly helpful for you and your healthcare team. Early and accurate diagnosis is vital, as even a six-month delay in treatment can lead to more joint damage over time. By monitoring your symptoms closely, you can help your doctor adjust your treatment plan quickly and effectively, ensuring you’re always on the right track to feeling better.
Set Realistic Goals for Your Recovery
When you're dealing with chronic pain, it's easy to feel discouraged. Setting small, achievable goals can help you stay motivated and recognize your progress. Since initiating treatment for psoriatic arthritis as early as possible helps prevent long-term joint damage, your goals can focus on consistent action. Maybe your first goal is to do five minutes of gentle stretching each morning or to try an anti-inflammatory recipe once a week. Celebrate these small wins. Recovery is a journey, not a race, and the objective is to improve your function and maintain your quality of life for the long haul. These consistent steps add up to big changes over time.
When Is It Time to See a Professional?
Trying to manage persistent pain on your own can feel overwhelming, especially when you’re not sure what’s causing it. While it’s tempting to search for answers online and try different home remedies, there comes a point when self-diagnosing isn’t enough. Getting a clear, professional diagnosis is the most important first step toward finding real, lasting relief. A doctor can help you understand the root cause of your symptoms and rule out other conditions, ensuring you get on the right track from the start.
Ignoring persistent symptoms or hoping they’ll just go away can lead to bigger problems down the road, including permanent joint damage. A healthcare professional can create a personalized treatment plan that addresses your specific needs. This plan often involves a combination of medical treatments and supportive, natural therapies. At Laser Lab, we partner with you and your healthcare team to provide non-invasive pain management solutions that complement your overall wellness strategy. If you’re experiencing any of the signs below, it’s time to schedule an appointment and get the clarity you deserve.
Red Flag Symptoms You Shouldn't Ignore
Sometimes your body sends clear signals that something more serious is happening. With psoriatic disease, certain symptoms act as red flags, indicating that you need to see a doctor sooner rather than later. Pay close attention if you have psoriasis and notice new issues with your nails, significant scalp psoriasis, or widespread skin lesions. These can suggest a more severe form of the disease that requires prompt medical attention. Don't dismiss these changes as minor annoyances. Being proactive and discussing them with a professional is the best way to protect your long-term joint health and overall well-being.
If Your Symptoms Are Getting Worse
If your pain and stiffness seem to be getting worse instead of better, it’s a clear sign to seek professional advice. It’s especially important to tell your doctor about any new or increasing back or neck pain, particularly if you experience significant morning stiffness that takes a while to ease up. An increase in pain or stiffness can signal a progression of the disease that needs to be addressed with a different treatment approach. Keeping a simple log of your symptoms can help you track these changes and communicate them effectively to your doctor, ensuring you get the right care when you need it.
How to Find the Right Specialists for Your Care
When you’re dealing with symptoms of psoriatic arthritis, seeing the right kind of doctor is key. While your primary care physician is a great starting point, psoriatic arthritis is best diagnosed and treated by a rheumatologist. A rheumatologist is a specialist who focuses on arthritis and other diseases of the joints, muscles, and bones. They have the expertise to identify the specific type of arthritis you have and can prescribe the most effective treatments to reduce inflammation, lessen pain, and help prevent permanent joint damage. Building a trusted healthcare team, including specialists and providers of complementary care, gives you the comprehensive support you need to feel your best.
Frequently Asked Questions
How can I tell if my sciatica is from psoriatic arthritis or a back injury? The biggest clue is often the timing and behavior of your pain. Pain from a mechanical injury, like a herniated disc, usually feels worse after activity and gets better with rest. Inflammatory pain from psoriatic arthritis is often the opposite; you might feel most stiff and sore first thing in the morning or after sitting for a while, with the pain actually improving as you start to move around.
Will light therapy get rid of my psoriatic arthritis? Psoriatic arthritis is a chronic autoimmune condition, which means there is no cure. However, light therapy is an excellent, non-invasive way to manage the symptoms. It works at a cellular level to reduce the inflammation that causes joint pain and nerve irritation. Think of it as a powerful tool to help you manage pain, reduce flare-ups, and support your body's healing process alongside your medical treatments.
I have psoriasis and back pain. What kind of doctor should I see first? Your primary care physician is always a great place to start the conversation. They can help rule out other issues and provide a referral. However, a rheumatologist is the specialist best equipped to diagnose and treat psoriatic arthritis. They focus on inflammatory and autoimmune conditions affecting the joints and can create a targeted treatment plan to prevent long-term damage.
Are the exercises for PsA-related sciatica different from regular sciatica exercises? Yes, the focus is a bit different. While both aim to relieve pain, exercises for PsA-related sciatica center on gentle movement to soothe inflammation and reduce stiffness. Low-impact activities like walking or swimming, along with specific nerve glides, are ideal because they improve mobility without stressing inflamed joints. The goal is to calm the area, not necessarily to strengthen muscles around a physical injury.
Can I manage this with just lifestyle changes, or do I need medication? Lifestyle changes like an anti-inflammatory diet and gentle exercise are incredibly important for managing day-to-day symptoms. However, because psoriatic arthritis is an autoimmune disease, medical treatment is often necessary to control the underlying inflammation and prevent permanent joint damage. The most effective approach combines medical care from your doctor with supportive lifestyle habits and natural therapies.
Frequently Asked Questions
Is light therapy safe for athletes?

Yes, light therapy is completely safe and highly beneficial for athletes. It promotes faster muscle recovery, reduces inflammation, and supports performance without the risks of medication or downtime. That’s why professional and amateur athletes worldwide rely on it to train smarter and recover quicker.
How many sessions will I need?

The number of sessions varies depending on the type and severity of your condition. Many patients notice improvement after 3–5 sessions, while chronic conditions may require ongoing care for best results. During your initial consultation, we’ll design a personalized treatment schedule tailored to your body’s response and recovery goals.




