

What Rheumatoid Arthritis Joint Pain Feels Like
Think about where your pain shows up. Is it just in your right knee? Or does it affect both of your wrists? This pattern is a huge clue. Osteoarthritis often picks one side, a result of wear and tear on a specific joint. But the pain in a rheumatoid arthritis joint is different. It's an autoimmune condition that usually creates a mirror image of discomfort on both sides of your body. This symmetry is one of the biggest distinctions when comparing osteoarthritis vs rheumatoid arthritis symptoms, and it offers powerful insight into what’s really happening.
Key Takeaways
- It's Wear and Tear vs. Autoimmune: Osteoarthritis is a mechanical issue caused by cartilage breaking down over time, while rheumatoid arthritis is a systemic autoimmune disease that creates widespread inflammation. This core difference is why their symptoms and treatment plans are so distinct.
- Listen to Your Symptoms: Pay attention to your pain patterns to spot the differences. Osteoarthritis pain typically worsens with activity and affects joints on one side of the body, while rheumatoid arthritis pain is often symmetrical, feels worse after rest, and includes prolonged morning stiffness.
- Seek a Diagnosis and Explore Natural Support: An accurate diagnosis from a doctor is the essential first step for creating an effective treatment plan. Regardless of the type of arthritis, you can manage pain and inflammation by integrating non-invasive therapies like light therapy and gentle exercise into your routine.
How to Spot the Signs of Osteoarthritis
If you’ve heard the term “wear-and-tear” arthritis, it was likely referring to osteoarthritis (OA). As the most common form of arthritis, OA happens when the protective cartilage that cushions the ends of your bones wears down over time. Unlike some other conditions, its symptoms tend to develop slowly and can worsen over many years. Understanding these early signs is the first step toward managing them effectively and maintaining your active lifestyle. The symptoms can range from a minor annoyance to a major obstacle, but knowing what to look for can help you find the right path to relief.
What Does Osteoarthritis Pain Feel Like?
The most common complaint with osteoarthritis is a deep, aching joint pain. You might notice it most during or after movement, like when you’re walking, climbing stairs, or gripping an object. The joint might also feel tender when you apply light pressure. Along with pain, stiffness is a classic sign, especially when you first wake up or after you’ve been sitting for a while. This stiffness usually gets better with a little movement. Many people also experience some swelling around the affected joint, which can make it feel even more uncomfortable and difficult to move. Finding effective pain management is key to handling these symptoms.
How OA Affects Your Range of Motion
Osteoarthritis can change how your joints feel and function day-to-day. You might notice a loss of flexibility or find that you can’t move a joint through its full range of motion anymore. Some people hear or feel a grating sensation when they use the joint, which can be accompanied by popping or cracking sounds. This is caused by the rough, worn-down cartilage surfaces rubbing against each other. In the beginning, the pain might come and go, but as the condition progresses, you may feel a more constant, dull ache even when you’re resting. This can make simple activities feel like a chore.
Which Joints Does Osteoarthritis Target?
While osteoarthritis can damage any joint, it most often affects the hands, knees, hips, and spine. One of the key ways OA distinguishes itself is that it often starts asymmetrically. This means it might affect the joints on one side of your body but not the other. For example, you could develop symptoms in your right knee long before your left one shows any signs of trouble. Over time, the condition can spread to other joints, but it typically follows this one-sided pattern initially. This is an important clue when trying to figure out what’s causing your joint pain.
Recognizing Rheumatoid Arthritis Symptoms
Rheumatoid arthritis (RA) is a bit different from osteoarthritis because it’s an autoimmune condition. This means your immune system mistakenly attacks your body's own tissues, primarily the lining of your joints. As a result, the symptoms of RA often go beyond simple joint pain and can affect your entire body. Understanding these signs is the first step toward finding the right kind of relief and getting back to feeling like yourself.
Why Morning Stiffness Is a Key RA Sign
One of the most common signs of RA is persistent joint inflammation. This isn't just a little ache; it's often accompanied by visible swelling, tenderness, and a feeling of warmth around the affected joint. Another classic symptom is morning stiffness. If you wake up feeling like the Tin Man and it takes more than 30 minutes to loosen up your joints, that’s a strong indicator of RA. This prolonged stiffness happens because fluids build up in the joints overnight due to inflammation, making movement difficult when you first get out of bed.
RA Symptoms That Aren't in Your Joints
Because RA is a systemic disease, its effects aren't confined to your joints. Many people with RA experience a deep, persistent fatigue that sleep doesn't seem to fix. It’s a kind of exhaustion that can make it hard to get through the day. You might also run a low-grade fever or just feel generally unwell, similar to having the flu. Some people even experience unexplained weight loss. These body-wide symptoms happen because your immune system is in overdrive, causing inflammation throughout your body, not just in one or two spots.
Identifying Swelling and Warmth in Your Joints
With rheumatoid arthritis, joint swelling often appears symmetrically. This means if your right wrist is affected, your left wrist probably is too. The same goes for your knees, hands, or feet. This symmetrical pattern is a key clue that helps doctors distinguish RA from other types of arthritis. The affected joints will typically feel warm to the touch and look puffy or swollen. This is a direct result of the inflammatory process happening inside the joint. Finding ways to manage this inflammation is crucial for pain management and protecting your joints from long-term damage.
Understanding Rheumatoid Arthritis
Rheumatoid arthritis is more than just achy joints; it's a systemic autoimmune disease. This means your immune system, which is designed to protect you from invaders like bacteria and viruses, gets confused and starts attacking your own healthy tissues. In the case of RA, the primary target is the synovium, the delicate lining of your joints. This attack triggers a cascade of inflammation that causes the pain, swelling, and stiffness characteristic of the condition. Unlike the wear-and-tear damage of osteoarthritis, RA can affect your whole body, leading to symptoms that go far beyond your joints.
The Nature of an Autoimmune Disease
When your immune system goes on the offensive against your joints, it causes the synovium to thicken, leading to the swelling and pain you feel in the joint capsule. According to the Cleveland Clinic, this inflammation can eventually damage the cartilage and bone within the joint. A key feature of RA is its symmetrical pattern. It usually affects the same joints on both sides of your body. So, if the knuckles on your right hand are inflamed, it’s very likely the knuckles on your left hand will be, too. This mirrored discomfort is a significant clue that you might be dealing with an autoimmune response rather than mechanical joint wear.
Flares, Remission, and Living with RA
Living with rheumatoid arthritis often means learning to manage its unpredictable nature. The condition is characterized by periods of "flares" and "remission." A flare is when your symptoms suddenly worsen, bringing on intense joint pain, swelling, and fatigue that can make daily activities feel impossible. These episodes can last for days or even months. In contrast, remission is a period when the inflammation subsides, and your symptoms improve or disappear completely. Understanding these cycles is a crucial part of managing the condition and developing a sustainable plan for your long-term preventative wellness.
Key Risk Factors for Developing RA
While the exact cause of rheumatoid arthritis isn't fully understood, researchers have identified several factors that can increase your risk. Genetics play a significant role; if a close family member has RA, your chances of developing it are higher. Your sex is also a factor, as women are more likely to be diagnosed with RA than men. Lifestyle choices matter, too. Smoking is a major risk factor and can also make the disease more severe if you do develop it. Additionally, studies have shown a link between obesity and an increased risk of developing RA.
Genetic and Lifestyle Influences
Experts believe that RA is triggered by a combination of factors rather than a single cause. You might have a genetic predisposition that makes you more susceptible, but it often takes an environmental trigger to set the disease in motion. According to the Mayo Clinic, things like an infection, smoking, or even significant physical or emotional stress can activate your immune system's faulty response. It’s this complex interplay between your genes, hormones, and environment that ultimately leads the immune system to begin its attack on your joints, creating the chronic inflammation that defines RA.
The Four Stages of Rheumatoid Arthritis Progression
Rheumatoid arthritis is a progressive disease, meaning it can worsen over time if not managed effectively. Doctors often categorize its progression into four distinct stages to better understand the extent of the joint damage and create an appropriate treatment plan. In the early stages, the focus is on controlling inflammation to prevent further damage. As the disease advances, the goal shifts to preserving joint function and managing pain. Knowing which stage you're in can help you and your healthcare provider make informed decisions about your care and explore supportive therapies to maintain your quality of life.
Stage 1: Early Joint Inflammation
In the first stage of RA, the inflammation is just beginning. Your immune system has started attacking the joint lining, or synovium, causing it to swell. You might feel some initial pain, stiffness, and tenderness in your joints, but there is no damage to the bone yet. An X-ray taken at this stage wouldn't show any signs of erosion. This is the critical window for early diagnosis and intervention. By focusing on reducing inflammation early on, you can help slow the progression of the disease and protect your joints from future damage, making it a key time for effective pain management strategies.
Stage 2: Cartilage Damage Begins
During the second stage, the persistent inflammation starts to take a toll on the cartilage in your joints. The synovium continues to thicken, and this inflammation begins to wear away the protective cartilage that cushions your bones. As the cartilage thins, you may experience more noticeable pain, stiffness, and a decreased range of motion. While there still might not be significant bone damage, the joint is becoming compromised. This is when symptoms can start to interfere more with your daily activities, making consistent management even more important.
Stage 3: Severe Damage to Cartilage and Bone
By the time RA reaches the third stage, it's considered severe. The inflammation has become so persistent that it has eroded not only the cartilage but also the bone itself. As the cushion between the bones disappears, the bones may start to rub against each other, causing significant pain and swelling. You might also begin to notice physical changes in your joints as they shift and deform due to the bone damage. This stage is often marked by increased pain, more pronounced stiffness, and a greater loss of mobility.
Stage 4: Joint Deformity and Loss of Function
In the final stage of rheumatoid arthritis, the inflammatory process often subsides, but the damage left behind is significant. The joints may become fused together, a condition known as ankylosis, which leads to a complete loss of joint function. The extensive damage to bone and cartilage can result in severe pain, swelling, and muscle weakness. While the joints no longer work as they should, it doesn't mean you're out of options. The focus at this stage is on managing pain and finding adaptive ways to perform daily tasks to maintain your independence.
Is It OA or RA? Spotting the Key Differences
Trying to figure out what’s causing your joint pain can feel like solving a puzzle. While both osteoarthritis (OA) and rheumatoid arthritis (RA) affect your joints, they are very different conditions with unique signs. OA is often called a "wear and tear" condition, where the cartilage that cushions your joints breaks down over time. RA, on the other hand, is an autoimmune disease, which means your immune system mistakenly attacks the lining of your joints, causing widespread inflammation. Understanding these distinctions is the first step toward finding the right path for relief. Let’s look at four key areas where OA and RA part ways, so you can get a clearer picture of what you might be experiencing.
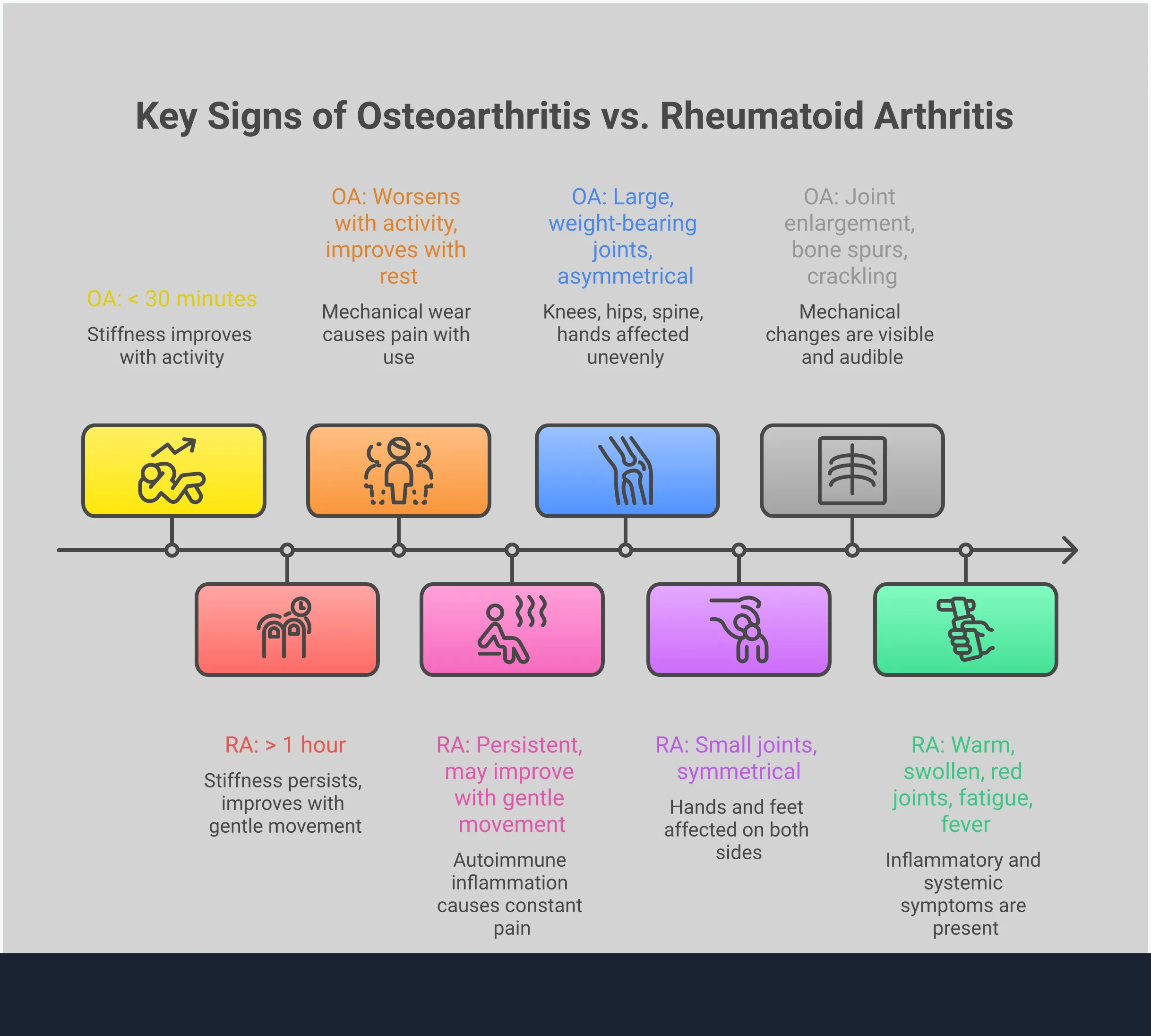
How the Pain Differs Between OA and RA
One of the biggest clues is the timing of your pain. If you have osteoarthritis, you’ll likely notice that your joints ache more during or after activity. Think of it as a wear-and-tear issue; the more you use a worn-down joint, the more it complains. Rest usually makes it feel better.
Rheumatoid arthritis, on the other hand, often works in reverse. The pain and stiffness are typically at their worst after you’ve been still for a while, especially first thing in the morning. Gentle movement and activity can actually help ease the discomfort. This is because RA is an inflammatory condition, and inactivity allows that inflammation to settle in and cause stiffness. Finding effective pain management starts with understanding these patterns.
How Long Does Morning Stiffness Last?
That stiff, slow-to-get-going feeling in the morning is common with both types of arthritis, but how long it lasts is a major differentiator. For people with osteoarthritis, morning stiffness is usually brief. It might take you a few minutes to work out the kinks, but it generally fades in under an hour, often much sooner.
With rheumatoid arthritis, the morning stiffness is more persistent and can significantly disrupt your day. It’s a defining symptom when the stiffness lasts for more than an hour. This prolonged feeling of being "stuck" or "frozen" is a classic sign that the inflammation from RA is at play. According to Alberta Health Services, this difference in duration is a key factor doctors use to compare the two conditions.
Does Your Joint Pain Affect Both Sides?
Think about which joints are hurting. Does the pain appear in the same joint on both sides of your body? Rheumatoid arthritis often presents symmetrically, meaning if your right wrist is affected, your left wrist probably is, too. This pattern of affecting joints on both sides of the body happens because RA is a systemic disease where the immune system attacks your body’s own tissues.
Osteoarthritis is typically asymmetrical. It’s more likely to show up in a single, specific joint that has seen a lot of use or a past injury, like your right knee or left hip. It doesn't follow a symmetrical pattern because it’s caused by the mechanical breakdown of cartilage in a particular area, not a body-wide autoimmune response.
Comparing Swelling and Inflammation in OA vs. RA
While both conditions can cause swelling, the nature of it is quite different. In rheumatoid arthritis, the swelling is a direct result of active inflammation. This means the affected joints may not only look puffy but also feel warm to the touch and appear red. This inflammation is also what can lead to other body-wide symptoms like fatigue and fever.
In osteoarthritis, any swelling you experience is generally milder and "harder." It’s often caused by the formation of bony spurs (osteophytes) around the joint, rather than the soft, tender swelling seen in RA. While there is some low-grade inflammation with OA, it’s not the primary driver of the condition the way it is with RA. Learning how to manage inflammation is a core part of preventative wellness for any type of joint pain.
Where Do OA and RA Show Up in the Body?
One of the biggest clues to figuring out whether you’re dealing with osteoarthritis or rheumatoid arthritis is where the pain shows up. While both conditions affect your joints, they tend to follow different patterns throughout the body. OA often picks and chooses specific, hard-working joints, while RA is less selective and usually appears in a more symmetrical fashion.
Think of it like this: if your joint pain is telling a story, its location is a key part of the plot. Paying attention to which joints are affected, and whether the pain is on one or both sides of your body, can give you and your doctor valuable insight. Understanding these patterns is a great first step toward identifying the root cause of your discomfort and finding a path to effective pain management. Let’s look at the typical joint patterns for both OA and RA.
Common Hotspots for Osteoarthritis
Osteoarthritis often begins in a single joint on one side of your body, though it can spread over time. Because it’s caused by mechanical wear and tear, it typically targets the body’s most frequently used, weight-bearing joints. This includes your knees, hips, and spine. You might also notice OA in smaller joints that see a lot of action, like the base of your thumb or the joints closest to your fingernails. For example, you might develop pain in your right knee from an old sports injury or find that only the joints in your right hand feel stiff and sore after years of work. This asymmetrical pattern is a hallmark of OA.
Typical Rheumatoid Arthritis Joint Patterns
Rheumatoid arthritis tends to present a much more symmetrical picture. Since it’s an autoimmune condition where the body attacks its own tissues, it often affects the same joints on both sides of the body at the same time. If your left wrist is swollen and painful, it’s very likely your right wrist is, too. This symmetry is a classic sign of RA. It commonly appears in the smaller joints of the hands and feet, as well as the wrists, elbows, and ankles. Unlike OA, which might affect just one or two joints, RA often involves multiple joints at once. This widespread, mirrored pattern is one of the most distinct differences between the two conditions.
Why Do OA and RA Target Different Joints?
The reason OA and RA affect different joints comes down to their underlying causes. Osteoarthritis is a degenerative condition, meaning it develops from the gradual breakdown of cartilage in a specific joint due to overuse, injury, or age. That’s why it’s often localized to a single, hard-working joint like a knee or hip. Rheumatoid arthritis, on the other hand, is a systemic autoimmune disease. Your immune system mistakenly attacks the lining of your joints (the synovium), causing widespread inflammation. This systemic attack explains why RA appears in multiple joints and in a symmetrical pattern. It’s not about wear and tear on a specific spot; it’s about a body-wide response. Understanding this helps create a plan for preventative wellness and symptom management.
RA Is More Than Just Joint Pain
Unlike osteoarthritis, which is primarily a "wear and tear" condition limited to your joints, rheumatoid arthritis is an autoimmune and inflammatory disease. This means your immune system mistakenly attacks healthy cells, causing painful swelling, mainly in the joints. But the effects of RA don't stop there. Because the inflammation is systemic, it can impact your entire body, leading to symptoms that go far beyond joint pain.
Understanding these whole-body effects is a key part of managing your health. It helps explain why you might feel unwell in ways that don't seem connected to your joints at first. Recognizing these signs allows you to have more informed conversations with your doctor and build a comprehensive care plan that addresses all your symptoms, not just the obvious ones. From persistent fatigue to issues with major organs, RA's reach is wide, making a holistic approach to wellness essential.
Understanding RA-Related Fatigue and Malaise
If you're dealing with a deep, persistent exhaustion that sleep doesn't seem to fix, you're not alone. This kind of fatigue is a hallmark symptom of RA. It’s not just about feeling a little tired; it's a draining lack of energy that can interfere with your daily life. This happens because your body is constantly using energy to fuel its immune response and fight widespread inflammation. When multiple joints are persistently inflamed, your body is in a constant state of high alert, which can leave you feeling completely wiped out and generally unwell.
Can RA Cause Fever and Weight Loss?
Have you noticed a persistent low-grade fever or that you're losing weight without trying? These can be surprising but common signs of rheumatoid arthritis. When your body is dealing with significant inflammation, it can trigger a slight fever, much like when you're fighting off an infection. Unexplained weight loss can also occur as your body burns more calories managing the inflammatory process. These systemic symptoms are your body's way of signaling that something is going on internally, and they are important clues that distinguish RA from other types of arthritis.
How RA Can Affect Your Organs and Skin
Because RA involves body-wide inflammation, it can affect organs and systems far from your joints. For some people, chronic inflammation can lead to anemia (a low red blood cell count), which contributes to fatigue and weakness. The inflammation can also affect your heart and blood vessels, increasing the risk of heart disease over time. Even your lungs can be impacted. It’s a clear example of how inflammation affects various body systems, which is why managing RA effectively is so important for your overall, long-term health.
Other Health Complications Linked to RA
Because rheumatoid arthritis is a systemic condition, the inflammation it causes can create issues in other parts of your body, not just your joints. This is a major reason why getting an accurate diagnosis and creating a comprehensive management plan is so important. When inflammation is allowed to persist, it can contribute to a range of other health concerns that might seem unrelated to your initial joint pain. Understanding these potential complications can help you stay proactive about your overall health and have more informed conversations with your healthcare provider about your long-term wellness.
Osteoporosis and Increased Infection Risk
The chronic inflammation associated with RA can speed up bone loss, leading to osteoporosis, a condition where bones become weak and more likely to break. On top of that, both RA itself and many of the powerful medications used to treat it can weaken your immune system. This can leave you more vulnerable to infections, from the common cold to more serious illnesses. It’s a double-edged sword where the disease and its treatment can both lower your body's natural defenses, making a focus on overall health and wellness even more critical for staying strong and resilient.
Rheumatoid Nodules and Carpal Tunnel Syndrome
Have you ever noticed firm bumps under your skin, especially near your elbows, hands, or feet? These are called rheumatoid nodules, and they are a common complication of RA. While they are usually painless, they can sometimes form in more sensitive areas or even on internal organs. Another common issue is carpal tunnel syndrome. When RA causes inflammation and swelling in your wrist, it can compress the major nerve that runs through to your hand. This pressure can lead to that familiar tingling, numbness, and weakness in your fingers, making everyday tasks feel much more difficult.
Heart and Lung Health
The systemic inflammation from RA can also take a toll on your major organs, particularly your heart and lungs. People with RA have a higher risk of developing hardened arteries and inflammation of the sac surrounding the heart. This is because the same inflammatory process that attacks your joints can also damage blood vessels and heart tissue. Similarly, your lungs can be affected, with inflammation sometimes leading to scarring that causes shortness of breath and other respiratory issues. This highlights why managing RA is not just about pain management, but about protecting your entire body for long-term health.
When to See a Doctor for Your Symptoms
It’s easy to brush off aches and pains as a normal part of life, but sometimes your body is trying to tell you something more. While occasional discomfort is one thing, persistent symptoms are a clear signal that it’s time to get a professional opinion. Listening to your body is the first step toward feeling better, and knowing when to reach out for help is crucial. If your joint pain is affecting your daily routine, making it harder to do the things you love, a conversation with your doctor can provide clarity and a path forward.
Getting a proper diagnosis is the key to creating an effective care plan. Whether it’s osteoarthritis, rheumatoid arthritis, or something else entirely, understanding the root cause of your symptoms allows you to explore the right treatment options. This could include conventional medical care alongside supportive, non-invasive therapies designed to help you manage pain and improve your quality of life.
Warning Signs That Mean It's Time to Call a Doctor
Pay close attention to joint pain, swelling, or stiffness that sticks around for more than a few days. While a little soreness after a workout is normal, persistent discomfort is not. You should schedule a visit with your doctor if you experience severe joint pain, noticeable swelling, or fatigue so significant it gets in the way of your daily activities. Other important signs include morning stiffness that lasts for more than an hour or any visible changes or deformities in your joints. These are key indicators that something more serious may be happening, and it’s always best to get it checked out.
The Importance of an Early Arthritis Diagnosis
Getting an early and accurate diagnosis, especially for rheumatoid arthritis, can make a world of difference in your long-term health. Treatments are most effective when started early, helping to manage symptoms, slow the progression of the disease, and prevent permanent joint damage. An early diagnosis empowers you to take control of your health sooner. Once you know what you’re dealing with, you can work with your healthcare provider to build a comprehensive plan that may include natural approaches to pain management and inflammation reduction. The sooner you have a clear picture, the faster you can get back to living your life with less pain and more freedom.
The Role of a Rheumatologist in Diagnosis
If your primary care doctor suspects your symptoms point toward rheumatoid arthritis, they will likely refer you to a specialist called a rheumatologist. Think of them as the detectives of the joint and immune system world. A rheumatologist is a doctor with specialized training in diagnosing and treating musculoskeletal diseases and autoimmune conditions like RA. Their expertise is crucial because the symptoms of RA can sometimes mimic other health issues. They know exactly what to look for and can piece together the clues from your symptoms, a physical exam, and specific tests to give you a clear and accurate diagnosis, which is the essential first step toward creating a treatment plan that works for you.
How Doctors Diagnose RA: Blood Tests and Imaging
Diagnosing rheumatoid arthritis isn't based on a single test. Instead, your rheumatologist will use a combination of tools to get a full picture of what's happening in your body. This process usually starts with blood tests, which can identify specific antibodies and inflammatory markers that are often present in people with RA. In addition to lab work, your doctor may order imaging tests like X-rays or MRIs. These allow them to look inside your joints for signs of inflammation and damage, such as bone erosion, that are characteristic of the condition. By combining these test results with your personal health history and a physical exam, your doctor can confirm a diagnosis and understand how the disease is affecting you.
How to Naturally Manage Arthritis Symptoms
Living with arthritis doesn't mean you have to rely solely on medication or accept daily pain as your new normal. Many people find significant relief by incorporating natural, holistic approaches into their routine. These strategies can help manage pain, reduce inflammation, and improve your overall quality of life without invasive procedures. From targeted light therapy to simple lifestyle adjustments, you have the power to take control of your symptoms and feel more like yourself again. Let’s explore some of the most effective ways to find natural comfort and support for your joints.
Can Light Therapy Help Soothe Joint Pain?
If you're looking for a drug-free way to manage arthritis symptoms, light therapy is a powerful option. This non-invasive treatment uses specific wavelengths of light to penetrate deep into your tissues, helping to reduce inflammation and stimulate cellular repair right at the source. It’s one of several holistic solutions that can provide relief without surgical intervention. By promoting better circulation and easing stiffness, light therapy offers effective pain management that supports your body’s natural healing processes. It’s a gentle yet effective way to get back to the activities you love with less discomfort.
Safe Exercises to Keep Your Joints Moving
When your joints hurt, exercise might be the last thing on your mind, but gentle movement is one of the best things you can do for arthritis. Regular, low-impact activity helps strengthen the muscles around your joints, maintain flexibility, and reduce stiffness. Studies have shown significant reductions in pain and disability from activities like walking and simple home-based exercises. The key is to start slow and listen to your body. Try incorporating activities like swimming, gentle yoga, or daily walks into your routine to keep your joints moving smoothly and comfortably.
Heat vs. Cold: Which Is Better for Your Pain?
Heat and cold therapy are simple, accessible tools for managing arthritis flare-ups. Applying heat, like with a warm towel or a heating pad, is great for soothing chronic stiffness and sore muscles. Heat increases blood flow to painful joints, which helps relax tightness and flush out pain-inducing waste products. On the other hand, cold therapy, using an ice pack wrapped in a towel, is best for acute pain and swelling. The cold helps constrict blood vessels, which can reduce inflammation and numb the area for temporary relief.
Easy Diet and Lifestyle Changes for Arthritis Relief
Small changes in your daily habits can lead to big improvements in your arthritis symptoms. Focusing on an anti-inflammatory diet rich in fruits, vegetables, whole grains, and healthy fats can help reduce overall inflammation in your body. Beyond diet, simple strategies like activity modification and mindfulness can help you avoid aggravating your joints during daily tasks. You might also find that using braces provides extra stability and reduces pressure on affected joints. These mindful adjustments empower you to manage your condition proactively every single day.
Tips for Managing RA Flare-Ups
Rheumatoid arthritis often comes in waves, with periods of calm followed by flare-ups where your symptoms suddenly get worse. These flares can be unpredictable and are often set off by triggers like stress, an infection, or simply being overtired. During a flare, it’s important to listen to your body. While rest is essential for reducing fatigue, gentle movement can be just as crucial. It might seem counterintuitive, but light activity helps prevent inflammation from settling into your joints and causing intense stiffness. Communicating openly with your doctor about what you're feeling is also key, as your experience provides the most valuable information for your care plan. The Arthritis Foundation emphasizes that understanding these flare-ups is a critical part of your long-term preventative wellness and protecting your joints from damage.
Comparing Treatment Approaches for OA and RA
Since osteoarthritis is about managing wear and tear and rheumatoid arthritis is about calming an overactive immune system, the treatment plans look quite different. The main goal is always to reduce pain and protect your joints, but the path to get there varies. Understanding these differences can help you have more informed conversations with your doctor and find the right combination of medical and holistic care that works for you.
What to Expect from an Osteoarthritis Treatment Plan
Because OA is caused by the natural wear and tear on your body, treatment focuses on managing the symptoms. It’s a degenerative condition where the cartilage cushioning your bones wears down over time, causing bones to rub together. This leads to pain that can come and go, as well as stiffness, especially in the morning or after you’ve been sitting for a while. The primary goals are to reduce pain, improve your joint function, and slow the disease's progression. Your plan might include lifestyle changes, physical therapy, and non-invasive options to manage discomfort without relying on heavy medications.
What to Expect from a Rheumatoid Arthritis Treatment Plan
Treating RA requires a different approach because it’s an autoimmune disease. This means your immune system is mistakenly attacking your own healthy joints, causing fluid buildup, swelling, and pain. The main goal of an RA treatment plan is to control this immune response to stop it from causing further damage. This often involves specific medications called disease-modifying antirheumatic drugs (DMARDs) that help calm the immune system. Alongside medical treatment, lifestyle changes that focus on reducing inflammation throughout the body are a key part of managing RA long-term.
Medications to Control Inflammation
When treating rheumatoid arthritis, the primary goal is to calm your body's overactive immune response. Unlike OA, where the focus is on managing wear and tear, RA treatment aims to stop your immune system from mistakenly attacking your joints. To do this, doctors often prescribe a class of drugs called disease-modifying antirheumatic drugs, or DMARDs. These medications work to suppress your immune system, which helps reduce the inflammation causing your pain and swelling. The idea is to get the condition under control and prevent it from causing long-term damage to your joints.
Advanced Drugs to Slow Disease Progression
For many people, managing RA involves more advanced medications designed to slow the disease's progression. A newer class of DMARDs, known as biologics, offers a more targeted approach. Instead of broadly suppressing the immune system, these drugs target specific inflammatory pathways that contribute to joint damage. The goal with these advanced treatments is to achieve remission, where you have few or no symptoms. This medical approach works best when combined with lifestyle changes that focus on reducing inflammation throughout the body, creating a comprehensive strategy for long-term wellness.
Surgical Options for Severe Joint Damage
When medications and other therapies are no longer enough to manage pain or when joints have become severely damaged, surgery may become an option. Procedures like joint fusion or total joint replacement can help restore function and provide significant pain relief for those with advanced RA. However, surgery is typically considered a last resort. Many people focus on creating a comprehensive care plan that includes non-invasive options to manage discomfort and inflammation from the start. By integrating supportive therapies early on, the goal is to protect joint health and maintain mobility, helping you avoid or delay the need for more invasive procedures down the road.
Adding Complementary Therapies to Your Treatment
No matter which type of arthritis you have, you can support your medical treatment with holistic care. Simple self-care strategies can make a big difference in your daily comfort. For example, using heat can help relax tight muscles and increase blood flow, while cold packs can reduce swelling and numb acute pain. Gentle movement and physical therapy are also excellent ways to keep your joints mobile. Many people find significant relief with complementary therapies like light therapy, which helps reduce pain and inflammation directly at the source, offering a safe, drug-free way to manage your pain.
Frequently Asked Questions
How can I tell for sure which type of arthritis I have? While this guide offers clues, the only way to get a definite answer is by seeing a doctor. They will likely discuss your symptoms, review your medical history, and perform a physical exam. To distinguish between osteoarthritis and rheumatoid arthritis, they may also use blood tests to look for inflammatory markers or imaging tests like X-rays to see what’s happening inside your joints. A clear diagnosis is the most important step toward creating a treatment plan that actually works for you.
Is one type of arthritis considered more serious than the other? Both conditions can significantly impact your quality of life, but they pose different challenges. Because rheumatoid arthritis is an autoimmune disease, its inflammation can affect your entire body, including organs like your heart and lungs, which can lead to more widespread health issues if left unmanaged. Osteoarthritis is typically confined to the joints, but it can still cause severe pain and disability. The seriousness really depends on the individual and how the condition is managed.
Can my age or lifestyle cause one type of arthritis over the other? Your daily life and age can play a role, especially with osteoarthritis. Since OA is a "wear and tear" condition, it's more common as we get older and is often linked to past joint injuries or jobs that put repetitive stress on certain joints. Rheumatoid arthritis, however, is an autoimmune condition, so its causes are more complex and not directly tied to lifestyle. Factors like genetics are thought to play a much larger role in who develops RA.
What's the first step I should take if my joints are constantly hurting? The best first step is to start paying closer attention to your symptoms. Keep a simple log of when your joints hurt, how long any stiffness lasts, and which specific joints are bothering you. Note whether the pain is on one or both sides of your body. Once you have a few days or weeks of information, schedule an appointment with your doctor. This log will give them valuable insight and help you have a more productive conversation.
Can natural therapies like light therapy help both OA and RA? Yes, many people with either type of arthritis find relief with natural, non-invasive therapies. Treatments like light therapy can be very effective because they work by reducing inflammation and promoting cellular repair directly at the source of the pain. Since inflammation is a key factor in both OA and RA, therapies that address it can help manage symptoms, reduce stiffness, and improve joint function without adding more medication to your routine.
Frequently Asked Questions
Is light therapy safe for athletes?

Yes, light therapy is completely safe and highly beneficial for athletes. It promotes faster muscle recovery, reduces inflammation, and supports performance without the risks of medication or downtime. That’s why professional and amateur athletes worldwide rely on it to train smarter and recover quicker.
How many sessions will I need?

The number of sessions varies depending on the type and severity of your condition. Many patients notice improvement after 3–5 sessions, while chronic conditions may require ongoing care for best results. During your initial consultation, we’ll design a personalized treatment schedule tailored to your body’s response and recovery goals.




