

How Physiotherapy Works for Arthritis Pain Relief
Living with arthritis pain can feel like a frustrating catch-22. Your joints hurt, so you move less. But less movement leads to more stiffness and weaker muscles, which only makes the pain worse. So how do you break the cycle? This is where expert guidance is a game-changer. Many people ask how physiotherapy work for arthritis, especially when movement itself is the problem. The answer is in its strategic approach. A physiotherapist doesn’t just tell you to move more; they teach you how to move smarter with a tailored plan of gentle exercises designed to build strength and improve flexibility, reducing strain on your joints.
Key Takeaways
- Address the root cause, not just the symptoms: Physiotherapy focuses on strengthening the muscles around your joints and improving mobility, which provides long-term support and relief instead of just masking pain.
- Explore a powerful, non-invasive alternative: As a drug-free strategy for managing arthritis, physiotherapy can be as effective as medication and may help you delay or even avoid the need for surgery.
- Your participation is key to success: A physiotherapy plan is a partnership. Your therapist provides a personalized roadmap, but your consistency with at-home exercises is what builds lasting strength and control over your condition.
Does Physiotherapy Work for Arthritis?
If you’re living with arthritis, you know that finding effective, long-term relief is the top priority. While there’s no single cure, physiotherapy stands out as a cornerstone of successful arthritis management. It’s a non-invasive, personalized approach that focuses on improving your movement, reducing pain, and giving you back control over your daily life. By working with a physiotherapist, you can learn how to protect your joints, build strength, and stay active without causing further discomfort. This approach isn’t about a quick fix; it’s about building a sustainable plan for better joint health and overall well-being.
First, What Is Arthritis and How Does It Affect You?
At its core, arthritis is inflammation in one or more of your joints. If you're dealing with it, you're likely all too familiar with the main symptoms: persistent pain, stiffness (especially in the morning), swelling, and a frustrating decrease in your range of motion. This isn't just a minor ache; it can make everyday activities like walking, gripping a coffee mug, or even getting dressed feel like a major challenge. The condition can affect people of all ages, and it's a leading cause of discomfort and mobility issues. Understanding what's happening in your joints is the first step toward finding effective ways to manage the symptoms and live more comfortably.
How Common is Osteoarthritis?
If you’re dealing with osteoarthritis, you are far from alone. It’s one of the most common forms of arthritis and a leading cause of disability around the globe. According to the World Health Organization, about 60% of people living with osteoarthritis are women, and while it can affect anyone, the risk increases with age. Many people begin to notice the first signs of joint pain and stiffness in their late 40s or mid-50s. This isn't just a minor inconvenience; the chronic pain and loss of mobility can significantly impact your quality of life, making it difficult to participate in activities you love and leading to a great deal of frustration.
How Physiotherapy Steps In to Help Manage Arthritis
This is where physiotherapy comes in as a powerful tool for managing arthritis. Think of physiotherapists as experts in body movement. Their primary goal isn't just to offer a temporary fix but to help you achieve long-term improvements in how you move and feel. They work with you to reduce pain, improve joint function, and strengthen the muscles surrounding your joints for better support. By creating a personalized plan, physiotherapy helps you stay active and maintain your independence at home and work. It’s a proactive approach focused on empowering you with the tools and techniques for effective pain management and a better quality of life.
Why Try Physiotherapy for Your Arthritis?
Physiotherapy is much more than just a set of exercises; it's a comprehensive approach to managing arthritis that can transform your daily life. By working with a physiotherapist, you're not just treating symptoms—you're building a foundation for long-term joint health. The benefits extend from easing your immediate discomfort to empowering you with the strength and knowledge to stay active and in control. Let's look at the key ways physiotherapy can make a real difference.
Find Relief from Pain and Inflammation
Living with arthritis often means dealing with persistent pain and stiffness, which can make even simple movements feel like a challenge. Physiotherapy offers a powerful, drug-free way to find relief. Through a tailored program of regular, gentle exercise, you can significantly reduce joint pain and manage inflammation. Unlike medication that can come with side effects, physiotherapy addresses the root mechanical issues causing discomfort. It helps with the stiffness and soreness that come with arthritis, making it a safe and effective cornerstone of your pain management plan. This approach helps you feel better without relying on surgery or heavy medications.
Regain Your Joint Mobility and Flexibility
When your joints are stiff and sore, your natural instinct might be to move less. Unfortunately, this can make the problem worse, leading to even less mobility. Physiotherapy helps break this cycle. A physiotherapist is an expert in how the body moves and can create a plan specifically for you. They use targeted exercises and techniques to gently increase your range of motion and improve flexibility in the affected joints. The goal is to help you move more freely and with less pain. This personalized guidance ensures you’re moving safely and effectively, helping you regain confidence in your body’s abilities.
Strengthen Muscles to Support Your Joints
Strong muscles are your joints' best friends. They act as natural shock absorbers, taking pressure off your arthritic joints and providing much-needed stability. A key focus of physiotherapy is building the muscles around your affected joints. This isn't about intense weightlifting; it's about targeted, low-impact exercises that improve strength and overall function. A physiotherapist will also help you set achievable goals and build confidence in managing your condition. By strengthening your body, you can keep yourself as active as possible and better support your joints through everyday activities, which is a core part of performance recovery and daily wellness.
Get Back to the Activities You Love
Ultimately, the goal of managing arthritis is to live your life to the fullest. Physiotherapy translates directly into real-world benefits that improve your daily routine. The personalized plans are designed around your specific goals, whether that’s walking your dog without pain, playing with your grandkids, or simply getting in and out of the car more easily. Beyond the exercises, physiotherapy empowers you with education and self-management strategies. You’ll learn how to listen to your body, make informed decisions about your care, and take control of your health for the long term, supporting your journey toward preventative wellness.
What Physiotherapy Treatments Help Arthritis?
When you think of physiotherapy, you might picture someone recovering from a sports injury. But it’s also one of the most effective ways to manage arthritis. A physiotherapist doesn't just give you a list of exercises; they create a comprehensive plan using a variety of techniques to address your specific symptoms. The goal is to reduce your pain, improve how you move, and give you the tools to manage your condition long-term, so you can get back to the activities you love.
Think of your physiotherapist as a partner in your health journey. They use their expertise to find the right combination of treatments that work for your body and your lifestyle. This could include hands-on therapy to ease stiff joints, gentle exercises to build strength, or even specialized therapies that use heat or cold to soothe inflammation. It’s a personalized approach designed to help you regain control and live more comfortably. This kind of proactive care is a cornerstone of preventative wellness and can make a significant difference in your daily life. By focusing on function and education, physiotherapy empowers you to understand your body better and take an active role in your own care, which is crucial for living well with a chronic condition like arthritis.
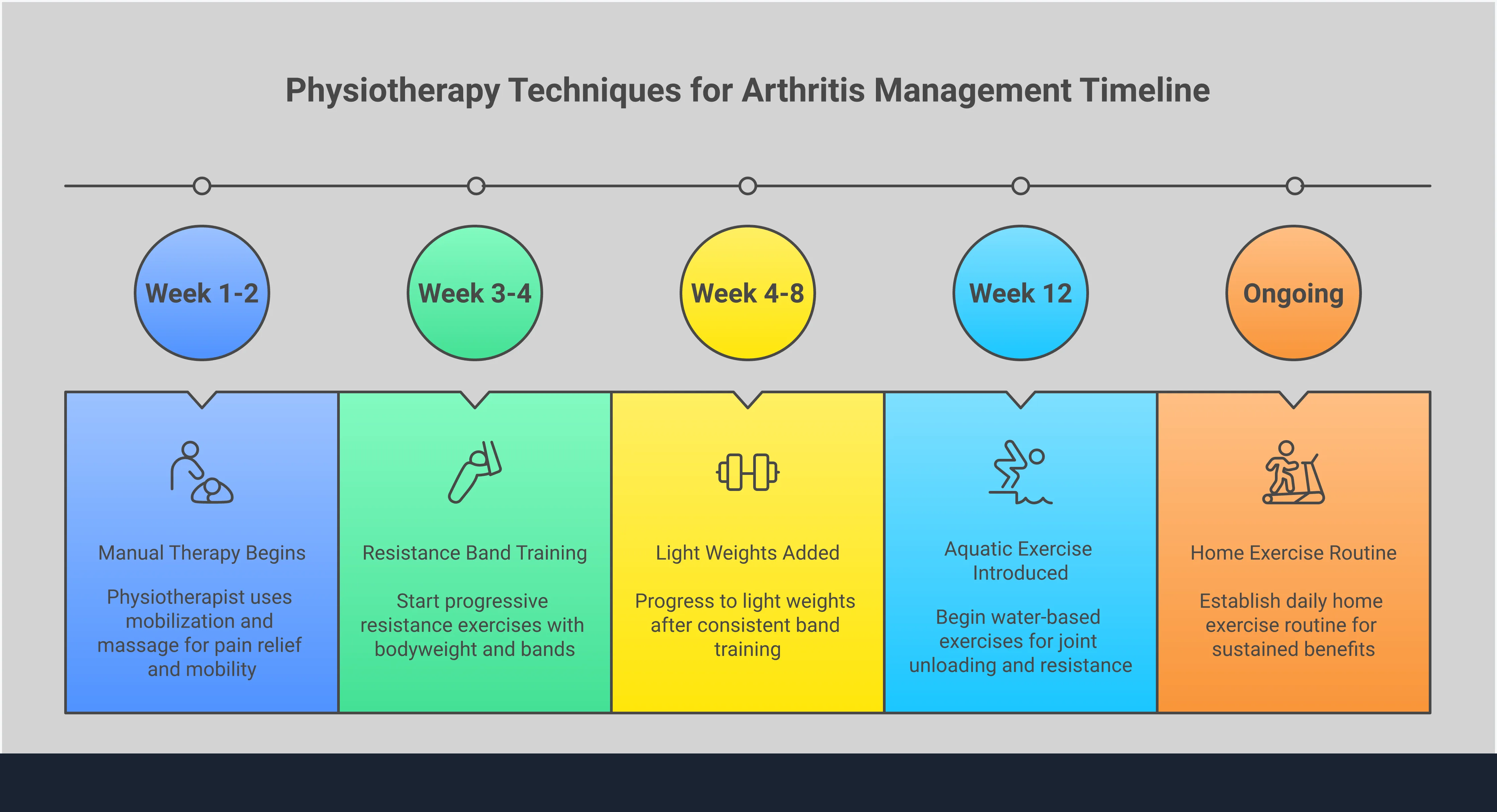
Hands-On Manual Therapy Techniques
One of the core components of physiotherapy for arthritis is manual therapy. This is a hands-on approach where your therapist uses skilled movements to work directly on your joints and soft tissues. They might use gentle mobilization techniques to improve your joint’s range of motion or soft tissue massage to release tight muscles that are contributing to your pain. It’s a targeted treatment that can provide immediate relief from stiffness and discomfort. By directly addressing the physical restrictions caused by arthritis, manual therapy helps restore function and makes it easier to move with less pain.
Custom Low-Impact Exercise Programs
The idea of exercising with sore joints can feel counterintuitive, but movement truly is medicine for arthritis. Your physiotherapist will guide you through low-impact exercises that get your heart rate up without putting stress on your joints. Activities like walking, cycling, or swimming are fantastic options. They’ll also create a strengthening program focused on building up the muscles around your affected joints. Stronger muscles act like a support system, taking pressure off the joints, which helps reduce pain and improve stability. This is a key strategy for effective pain management.
Types of Recommended Exercises
A physiotherapist will design a program with exercises tailored specifically to you. The focus is on gentle movements that build strength and improve your ability to move without causing more pain. This often includes range-of-motion exercises to reduce stiffness, strengthening exercises to build muscle support around your joints, and low-impact aerobic activities like swimming or walking to improve overall fitness. As the Arthritis Foundation explains, these targeted exercises are used to gently increase your range of motion and improve flexibility in the affected joints, helping to break the cycle of pain and inactivity.
Exercise Frequency and Duration
When it comes to exercising with arthritis, consistency is far more important than intensity. Your physiotherapist will help you create a routine that fits into your life, starting slowly and gradually increasing the duration and frequency as you get stronger. The goal is to make movement a regular, manageable part of your day. According to the Mayo Clinic, a program of regular, gentle exercise can significantly reduce joint pain and manage inflammation. This steady approach helps you build momentum and see lasting results without overwhelming your body, making it a sustainable part of your long-term wellness plan.
Tips for Protecting Your Joints
Beyond specific exercises, a huge part of physiotherapy is learning how to protect your joints during everyday activities. Your therapist will teach you practical strategies to reduce strain and manage discomfort. This might include simple adjustments like maintaining good posture, using assistive devices to open jars, or learning how to lift objects without stressing your joints. They can also show you how to use heat packs to soothe tense muscles or ice packs to reduce swelling in your joints. These small changes can make a big difference in your daily comfort and help prevent flare-ups.
Listening to Your Body
Learning to distinguish between the normal discomfort of a new exercise and pain that signals a problem is a critical skill. Your physiotherapist will teach you how to pay attention to your body's signals. It’s important to remember that some muscle soreness is normal when you start a new routine, but sharp, stabbing, or constant pain is not. If you feel pain that's worse than your usual joint pain, or if you notice new swelling or redness, it's a sign to slow down or stop. This self-awareness empowers you to stay active safely and ensures your exercise plan is helping, not hurting.
Aquatic Therapy: Gentle on Your Joints
Aquatic therapy, sometimes called hydrotherapy, is an excellent option for people with significant joint pain. This treatment involves performing gentle exercises in a warm pool. The natural buoyancy of the water supports your body weight, which dramatically reduces the strain on your joints. This allows you to move more freely and with less pain than you could on land. The warmth of the water also helps to relax tense muscles and soothe aching joints, making it a comfortable and effective way to improve your mobility, strength, and flexibility.
Using Heat and Cold to Soothe Your Joints
Beyond exercises and hands-on techniques, physiotherapists often use specialized modalities to help manage arthritis symptoms. Heat and cold therapy are two of the most common. Applying a heat pack can help relax tense, sore muscles and improve circulation before you start your exercises. On the other hand, using an ice pack is great for reducing swelling and inflammation in your joints after activity. Your therapist will show you how and when to use each one as part of your self-management plan, giving you simple yet powerful tools to control your symptoms at home.
Additional Pain Management Techniques
Beyond hands-on therapy and exercise, a comprehensive physiotherapy plan often includes other strategies to help you manage your arthritis symptoms day-to-day. Your therapist can introduce you to various tools and techniques that provide support, relieve pain, and make daily activities easier. These methods are designed to complement your active treatments, giving you more control over your comfort levels. By incorporating these additional approaches, you can build a well-rounded pain management strategy that addresses your unique needs and helps you stay engaged in the activities you enjoy with greater confidence and less discomfort.
Therapeutic Tools like TENS and Splints
Your physiotherapist might recommend specific tools to help manage pain and support your joints. For instance, they may suggest using splints to stabilize and rest a particularly painful joint, which can be especially helpful during a flare-up. Another common tool is a TENS (Transcutaneous Electrical Nerve Stimulation) unit. This small, portable device uses a mild electrical current to reduce pain signals going to the brain and may help your body produce more of its natural painkillers. Your therapist can teach you how to use these tools safely and effectively, integrating them into your routine to provide targeted, drug-free relief right where you need it.
Help with Assistive Devices
Sometimes, the best way to protect your joints is to use a little extra support. Assistive devices can make a huge difference in your mobility and independence. A physiotherapist can assess your needs and show you how to properly use tools like a cane or walker to reduce the load on your hips, knees, or ankles. They might also recommend other helpful items, such as braces for joint support or specialized shoe inserts (orthotics) to improve your alignment and absorb shock when you walk. Learning to use these devices correctly is key to getting the most benefit and moving with greater ease and safety.
Physiotherapy vs. Other Arthritis Treatments
When you’re living with arthritis, it’s natural to look at all the options on the table. Most people are familiar with the two most common paths: medication to manage pain and surgery to replace a joint. But where does physiotherapy fit in? It’s not just a set of exercises; it’s a comprehensive approach to improving how your body moves and feels, getting to the root of the problem instead of just masking the symptoms.
Thinking about your treatment plan isn’t about picking one option and sticking with it forever. It’s about understanding the pros and cons of each and finding the right combination for your unique needs. While medication can offer quick relief and surgery can be a necessary step for severe joint damage, physiotherapy provides a non-invasive, empowering way to take control of your joint health. It focuses on building your body’s natural strength and resilience, which can lead to lasting relief and a better quality of life. Let’s break down how it stacks up against other common treatments.
Physiotherapy vs. Medication
Medication is often the first thing people reach for to handle arthritis pain, and it can certainly be effective for short-term relief. However, it primarily works by masking pain signals rather than addressing the underlying cause. Physiotherapy takes a different approach. It focuses on improving your joint’s function by strengthening the muscles that support it, increasing flexibility, and restoring proper movement patterns.
While medication provides symptomatic relief, physiotherapy aims to create long-term change. Think of it this way: medication can turn down the volume on your body’s alarm bells, but physiotherapy helps fix what’s setting off the alarm in the first place. Studies have shown that a consistent physiotherapy program can be just as effective as medication for pain relief, with the added benefits of improved mobility and strength, all without the potential side effects of long-term drug use.
Can Physiotherapy Help You Avoid Surgery?
The idea of joint surgery can be daunting, and for good reason. It’s an invasive procedure with a long recovery period that’s typically considered a last resort. Before you go down that road, it’s worth exploring what physiotherapy can do for you. For many people, especially those in the earlier stages of arthritis, physiotherapy can be a powerful tool to postpone or even eliminate the need for surgery.
By focusing on building strength, improving range of motion, and correcting movement habits that put stress on your joints, physiotherapy helps your body support itself more effectively. This reduces the strain on the damaged joint, which in turn alleviates pain and improves function. It’s a proactive approach that empowers you to manage your condition and maintain your independence without going under the knife.
How Physiotherapy Complements Other Treatments
Your treatment plan doesn’t have to be an either-or decision. In fact, the most effective strategies often involve combining different therapies to create a synergistic effect. Physiotherapy pairs exceptionally well with other non-invasive treatments, especially advanced options like light therapy. While physiotherapy works on the mechanical function of your joints, light therapy works at the cellular level to reduce inflammation and accelerate tissue repair.
This combination can be a game-changer. The pain management benefits of light therapy can make it easier and more comfortable to perform your physiotherapy exercises, allowing you to get more out of each session. Together, they create a holistic plan that addresses both the symptoms and the root causes of your arthritis, supporting your body’s natural healing processes and promoting long-term preventative wellness.
Combining Physiotherapy with Light Therapy
At Laser Lab Therapy, we often see the best results when treatments are combined to create a more powerful effect. Think of physiotherapy as the "macro" approach—it focuses on strengthening muscles, improving your range of motion, and correcting the mechanics of how your joints move. Light therapy, on the other hand, is the "micro" approach. It works at a cellular level to reduce the deep-seated inflammation and pain that are hallmarks of arthritis. When you put them together, you get a comprehensive strategy that tackles the problem from both the outside in and the inside out, addressing both the symptoms and their source.
This combination creates a powerful cycle of improvement. The significant pain management benefits from light therapy can make it much more comfortable to perform your physiotherapy exercises, allowing you to build strength and mobility more effectively and get more out of every session. This holistic approach doesn't just mask symptoms; it actively supports your body’s natural healing processes. By addressing both the mechanical issues and the underlying inflammation, you can build a sustainable foundation for long-term preventative wellness and get back to living your life with less pain and more freedom.
What to Expect from Your Physio Appointments
Starting physiotherapy for arthritis can feel like a big step, but knowing what the process looks like can make it feel much more manageable. Your sessions are a partnership between you and your therapist, designed to help you regain control and feel better in your body. It’s not about pushing through intense, painful workouts that leave you feeling defeated. Instead, it’s a thoughtful and supportive process focused on building strength, improving mobility, and giving you the tools you need to manage your symptoms effectively day-to-day.
From your very first appointment, the goal is to understand your unique situation. Your therapist will listen to your concerns, assess your physical condition, and work with you to set realistic goals that matter to you—whether that’s walking the dog without pain or getting back to gardening. Each session builds on the last, gradually helping you move with more confidence and less discomfort. Think of your physiotherapist as a coach who is there to guide you, teach you, and cheer you on as you work toward a more active and comfortable life. The entire experience is tailored to you, ensuring that the plan adapts as you get stronger and your needs change.
Your First Step: The Initial Assessment
Your first physiotherapy appointment is all about creating a roadmap for your treatment. It starts with a conversation where you can share your story—what hurts, what activities are difficult, and what you hope to achieve. Your physiotherapist will then conduct a gentle physical evaluation, looking at your muscle strength, joint movement, and overall activity level. This isn't a test; it's simply a way to get a clear picture of your starting point. Based on this assessment, your therapist will develop a custom plan just for you. This plan outlines the specific exercises and techniques that will help you reach your goals. It’s a collaborative process, so you’ll have the chance to ask questions and make sure you feel comfortable with the approach.
What a Typical Physio Session Looks Like
Once your plan is in place, you’ll begin your regular sessions. These appointments usually last about an hour and are very hands-on. Your physiotherapist will guide you through your prescribed exercises, making sure you’re using the correct form to get the most benefit without causing strain. They may also use manual therapy techniques to help ease stiffness and improve your range of motion. A huge part of each session is education. Your therapist’s main goal is to teach you how to perform your exercises and treatments correctly on your own. This empowers you to take an active role in your pain management between appointments. You’ll leave each session feeling more knowledgeable and confident in your ability to manage your arthritis symptoms at home.
Your At-Home Plan for Lasting Relief
The work you do between your physiotherapy appointments is where the real magic happens. The most important factor in your success is consistently doing the exercises your therapist teaches you. Your at-home plan is designed to be manageable and effective, helping you build on the progress you make in the clinic. Your therapist will also give you practical advice on how to stay active, balance rest with activity, and set achievable goals for yourself. They’ll likely create a "graded exercise program," which means you’ll start slowly and gradually increase the intensity. This approach helps you build strength and stamina without triggering pain or inflammation, setting you up for long-term joint health and a better quality of life.
Understanding and Managing Arthritis Flares
Even with a solid management plan, there will be days when your arthritis symptoms feel much worse. These periods, known as flares, are a normal part of living with the condition, but they can be discouraging. A flare is when your usual symptoms of pain, stiffness, and fatigue suddenly intensify, making it difficult to get through your day. Understanding what’s happening in your body and having a plan to respond can make these episodes feel less overwhelming. The key is to listen to your body, adjust your routine, and use the right strategies to get back on track without losing the progress you’ve made.
What is an Arthritis Flare?
Think of an arthritis flare as a temporary, but intense, spike in your symptoms. It’s when the inflammation in your joints kicks into high gear, causing a sudden increase in pain, swelling, and stiffness that goes beyond your typical day-to-day discomfort. Flares can last for a few days or even a few weeks, and they often come with a heavy dose of fatigue and even mental fogginess that can make concentration difficult. Learning to cope with these flares is a crucial part of your overall management strategy, helping you feel more in control when your symptoms feel anything but.
How to Handle a Flare-Up
When you feel a flare coming on, your first instinct should be to give your body a break. Rest the affected joint as much as you can to let the inflammation calm down. Applying ice packs can help reduce swelling, while a heat pack or a warm shower can soothe stiffness, especially in the morning. Over-the-counter pain relievers like acetaminophen or NSAIDs can also provide temporary relief. It’s important to have a go-to plan for these moments, as it gives you a sense of control. These simple at-home strategies are a great first line of defense for immediate pain management.
Flare Symptoms Across Different Arthritis Types
While all arthritis flares involve a worsening of symptoms, the specifics can vary depending on the type of arthritis you have. If you have Rheumatoid Arthritis (RA), a flare might bring on intense joint pain and swelling, significant morning stiffness, and profound fatigue. For those with Psoriatic Arthritis, a flare can include those same joint issues, but you might also notice a worsening of skin plaques. Understanding the specific signs of a flare for your condition helps you recognize it early and take action quickly, which can shorten its duration and reduce its intensity.
Lifestyle Adjustments to Support Your Joints
Managing arthritis effectively goes beyond your physiotherapy appointments. The small choices you make every day can have a huge impact on your joint health and overall comfort. Simple lifestyle adjustments, from the shoes you wear to the way you arrange your workspace, can help reduce strain on your joints and prevent your symptoms from getting worse. These changes aren’t about overhauling your entire life; they’re about making smart, intentional modifications that support your body. By taking a proactive approach, you can protect your joints, conserve your energy, and continue to do the things you love with less pain.
Choosing the Right Footwear for Arthritis
Your feet are your foundation, and what you put on them can affect your entire body, from your ankles and knees all the way up to your hips and back. Wearing unsupportive shoes can throw your alignment off balance, putting extra stress on already sensitive joints. The right pair of shoes, on the other hand, can act as shock absorbers, cushioning your joints with every step. Investing in proper footwear is one of the simplest and most effective ways to reduce pain and improve your stability, making it an essential part of your daily arthritis care.
What to Look For in a Shoe
When shopping for shoes, prioritize function over fashion. Look for a pair that offers a good combination of cushioning, arch support, and stability. Shoes with thick, resilient midsoles are excellent for absorbing impact. It’s also a great idea to find shoes with removable insoles, as this allows you to insert custom orthotics if you need them. The right shoe should fit your specific foot shape and provide support exactly where you need it most, helping to distribute your weight evenly and reduce pressure on painful joints.
Shoes to Avoid with Arthritis
Just as important as knowing what to look for is knowing what to avoid. Stay away from shoes that offer little to no support, like flip-flops and most flat sandals. These can force the muscles in your toes and feet to over-grip, which can increase pain. High heels are another major culprit, as they shift your body weight forward and can increase the pressure on the front of your foot by up to 80%. While they might look good for a special occasion, these types of shoes can seriously aggravate your arthritis symptoms and should be avoided for daily wear.
Home and Work Modifications for Easier Living
Making small changes in your environment can make a big difference in protecting your joints. A physiotherapist can be an incredible resource here, offering practical advice on how to adapt your daily routines. They can show you how to protect your joints during everyday tasks, whether it’s using ergonomic tools in the kitchen or adjusting your desk setup at work. By setting achievable goals together, you can build confidence in managing your condition and stay as active as possible. These modifications are a key part of a long-term preventative wellness strategy, helping you conserve energy and reduce unnecessary strain on your body.
Can Physiotherapy Treat Different Types of Arthritis?
Arthritis isn't a single condition; it's a term for over 100 types of joint pain and disease. Because each type affects your body differently, the right physiotherapy plan will be tailored specifically to you. A skilled practitioner will create a program that addresses the root cause of your discomfort, whether it’s the wear-and-tear of osteoarthritis or the inflammation of rheumatoid arthritis. The goal is always the same: to help you move more freely and with less pain. Let’s look at how physiotherapy can help with some of the most common forms of arthritis.
Physiotherapy for Osteoarthritis
Osteoarthritis (OA) is the most common type of arthritis, often called the "wear-and-tear" kind. It happens when the protective cartilage that cushions your joints breaks down over time. Physiotherapy for OA focuses on gentle, consistent movement to keep your joints flexible and strengthen the muscles around them. Studies have shown that a consistent physical therapy program can be just as effective as medication or even surgery for managing OA symptoms. By improving your strength and mobility, you take pressure off the affected joints, which can significantly reduce pain and improve your ability to do daily activities.
Physiotherapy for Rheumatoid Arthritis
Rheumatoid arthritis (RA) is an autoimmune disease where your body’s immune system attacks the lining of your joints, causing painful swelling and inflammation. A physiotherapist acts as your partner in managing RA. They do more than just prescribe exercises; they help you feel confident in managing your condition, address your concerns, and set realistic goals to stay active. The right physiotherapy plan can help you manage pain, improve how you move, and make your joints stronger without causing flare-ups. It’s all about finding the right balance of rest and activity to keep you feeling your best.
Physiotherapy for Spinal Arthritis
Spinal arthritis, or spondyloarthrosis, causes stiffness and pain in the neck and back. Physiotherapy is a cornerstone of managing this condition, using a combination of techniques to maintain your spine's flexibility and strength. Your treatment might include hands-on manual therapy to improve joint movement, targeted exercises to strengthen your core and back muscles, and guidance on proper posture. Learning how to maintain a healthy weight and use good body mechanics, like bending your knees when lifting, can also make a huge difference. These strategies work together to provide lasting pain management and help you keep your spine healthy.
How Soon Can You Expect to See Results?
It’s completely normal to wonder how long it will take to feel better. When you’re dealing with joint pain, you want relief as soon as possible. While physiotherapy isn’t an overnight fix, it is an effective way to create lasting change. Think of it less like a quick repair and more like building a stronger foundation for your body. The goal is to establish healthy habits that improve your life for the long term, not just for a few weeks. This approach helps you regain control and build resilience against future flare-ups.
Every person’s journey with arthritis is unique, so your timeline for results will be, too. It depends on several factors, including the type and severity of your arthritis, your overall health, and how consistently you follow your plan. Some people notice small improvements in mobility or a slight decrease in pain within a few weeks. For others, it might take a bit longer. The key is to stay patient and trust the process. Combining your physiotherapy with other supportive treatments focused on pain management can also help create a well-rounded approach to your care, ensuring you feel supported every step of the way. Your therapist will work with you to set realistic milestones so you can celebrate your progress and stay motivated.
Setting a Realistic Timeline for Relief
Getting stronger and moving more freely takes time and consistent effort. You can expect to see gradual improvements as you stick with your program. A typical physiotherapy plan for arthritis often starts with appointments twice a week for about four to six weeks. During this initial phase, you’ll learn proper form for your exercises and begin building a solid base of strength and flexibility.
While you may feel better during these first few weeks, the most significant changes often come with continued dedication. Many people report the best results in pain reduction and quality of life after sticking with their exercise programs for at least 12 weeks. Remember, progress isn’t always linear—you’ll have good days and some that are more challenging. The goal is steady, forward movement.
What Affects Your Progress?
Your active participation is the single most important factor in your success. While your therapist guides you, the real work happens when you apply what you’ve learned to your daily life. The most crucial part of a successful plan is learning the exercises from your therapist and doing them regularly at home. This consistency is what reinforces new movement patterns and builds strength over time.
Your treatment plan will also be made just for you, based on your specific goals. Whether you want to get in and out of the car without pain or walk a 5K, your physiotherapist will design a program to help you get there. Other factors, like the type of arthritis you have and your overall health, also play a role. Ultimately, your commitment to the plan is what will make the biggest difference.
Can Physiotherapy Slow the Progression of Arthritis?
It’s a question we hear often: Can you actually slow down arthritis? While there’s no cure, taking a proactive approach can make a significant difference in managing your symptoms and protecting your joints for the long haul. Think of physiotherapy not just as a way to find relief now, but as an investment in your future mobility and comfort. By consistently working with a professional, you can learn how to move better, build strength, and reduce the strain on your joints, which can help manage the progression of the condition over time. It’s about giving your body the support it needs to stay as healthy and active as possible.
How Regular Physio Protects Your Joints
One of the most powerful aspects of physiotherapy is its preventive potential. Consistent, guided exercise offers many advantages over surgery and medication. In fact, some studies show that physical therapy can be just as effective as more invasive procedures. By strengthening the muscles that support your joints and improving your range of motion, you can reduce daily wear and tear. A therapist also equips you with education and self-management strategies, empowering you to take control of your health. This knowledge helps you make informed decisions about your care and, in some cases, may even postpone or eliminate the need for joint replacement surgery by improving your function and easing pain.
Building a Plan for Long-Term Joint Health
The goal of physiotherapy is to build a foundation for lasting joint health. Physical therapists are trained experts who create personalized plans to help you move with greater ease. For arthritis, this means focusing on specific strategies that address the root of the problem. Your plan will likely include exercises to strengthen the muscles around your affected joints, which act as natural shock absorbers. It will also focus on improving flexibility to keep your joints from becoming stiff. By helping you manage your arthritis in this way, physiotherapy doesn’t just reduce pain—it helps you maintain your independence and continue doing the activities you love for years to come.
Your Top Physiotherapy Questions, Answered
Starting any new treatment path can bring up a lot of questions. If you’re considering physiotherapy for arthritis, it’s completely normal to have some concerns about what the process involves and whether it’s the right choice for you. Many people have preconceived notions about physical therapy—that it’s only for athletes or people recovering from surgery, or that it’s going to be a painful, grueling process.
Let’s clear the air and address some of the most common worries head-on. Understanding what physiotherapy for arthritis is really like can help you feel more confident and prepared to take the next step. We’ll look at what you can expect in terms of comfort, who can benefit from this type of care, and the truth about exercise and joint health.
Will the Treatment Be Painful?
This is probably the biggest question on your mind, and the answer is simple: the goal of physiotherapy is to relieve your pain, not make it worse. While you might feel some mild soreness or fatigue after a session—similar to how you’d feel after a good workout—you should never experience sharp or unbearable pain. Your physiotherapist is your partner in this process. They will work within your comfort zone, constantly checking in with you and adjusting exercises or techniques as needed. Open communication is key. If something doesn’t feel right, you should always speak up. The entire treatment plan is designed to reduce inflammation and build strength gently, helping you achieve long-term pain management.
How Do I Know If It's Right for Me?
Many people think physiotherapy is only for recovering from a major injury, but its benefits are much broader. If you're living with any type of arthritis that causes joint pain, stiffness, or difficulty with daily activities, physiotherapy can likely help. It’s a proactive approach that not only addresses current symptoms but also provides you with strategies to prevent future flare-ups and injuries. Whether you’re struggling to open a jar, walk up the stairs, or simply want to maintain your independence, a physiotherapist can create a plan tailored to your specific goals. A consultation is the best way to find out how a personalized program can support your unique needs and improve your overall well-being.
Is Exercise Really Safe for Arthritic Joints?
One of the most persistent myths about arthritis is that exercise will wear down your joints and make the condition worse. In reality, the opposite is true—movement is crucial. Inactivity can cause your muscles to weaken and your joints to become even stiffer. A physiotherapist won’t ask you to do anything that causes harm. Instead, they will guide you through safe, controlled, and low-impact exercises designed to strengthen the muscles that support your joints. This added support actually reduces the stress on the joint itself, improving stability and function. This focus on smart, targeted movement is a core part of preventative wellness and long-term joint health.
How to Get Started with Physiotherapy
Taking the first step toward managing your arthritis pain can feel like the hardest part, but finding the right support makes all the difference. A great physiotherapy plan starts with a practitioner who truly understands your condition and a strategy that’s built just for you. This isn't about pushing through pain; it's about working with an expert to find gentle, effective ways to improve your movement and daily life. Let's walk through how to find the right professional and what goes into creating a plan that fits your unique needs.
How to Find a Physiotherapist for Arthritis
Not all physiotherapists have the same areas of expertise, so it’s important to find someone experienced in treating arthritis. Think of physiotherapists as experts in how your body moves—they are trained to help you stay active and independent. When you start your search, you can use online tools from organizations like the American Physical Therapy Association to find a therapist. Once you have a few options, don't hesitate to call and ask if they have experience with your specific type of arthritis. This simple step ensures you connect with a professional who understands the nuances of your condition from day one.
What to Ask a Potential Therapist
Finding the right therapist is like finding a great coach—you want someone who understands your goals and knows how to get you there safely. A physiotherapist should feel like a partner in managing your condition, so it’s important to feel comfortable and confident in their approach. Before committing to a plan, have a few key questions ready for your first conversation:
- What is your experience with treating my specific type of arthritis (e.g., osteoarthritis, rheumatoid arthritis)?
- What does your typical treatment approach look like? Do you combine hands-on therapy with exercise?
- How will we work together to set goals and measure my progress?
- What is your philosophy on managing pain or discomfort during our sessions?
Their answers will give you a clear sense of their style and whether they’re the right fit for you. A good therapist will welcome your questions and make you feel like an active participant in your own care from the very beginning.
Working Together on Your Personal Treatment Plan
Your arthritis is unique to you, and your treatment plan should be, too. During your first visit, a physiotherapist will conduct a thorough assessment, looking at your current activity level, muscle strength, and joint range of motion. Based on this evaluation, they will create a special plan designed to improve your flexibility, strength, and balance. This isn't a generic handout of exercises; it's a tailored roadmap for your body. Remember that progress takes time and consistency. By sticking with your plan and communicating with your therapist, you’ll slowly and steadily work toward better movement and less pain.
Frequently Asked Questions
I'm worried exercise will make my joint pain worse. How does physiotherapy avoid this? This is a completely valid concern, and it’s the number one reason people with arthritis avoid movement. A physiotherapist’s entire approach is built around this challenge. They are experts in body mechanics who create plans that work within your comfort level. The goal is to find the sweet spot where you are strengthening the muscles around your joints without causing a flare-up. It’s all about gentle, controlled, and low-impact movements that reduce strain, not add to it.
What's the difference between doing physiotherapy and just exercising on my own? While any safe movement is beneficial, physiotherapy is far more targeted than a general workout. A physiotherapist conducts a detailed assessment to understand your specific movement patterns, muscle imbalances, and joint limitations. Based on that, they design a program just for you. They teach you the correct form for every exercise to ensure you’re supporting your joints properly, which is something you can’t get from a fitness app or a class at the gym.
How long will I need to be in physiotherapy? Physiotherapy isn't meant to be a lifelong series of appointments. The initial phase typically involves more frequent sessions to assess your condition, create your plan, and teach you the exercises correctly. The ultimate goal is to empower you with a self-management program that you can confidently do on your own at home. You might have periodic check-ins to adjust your plan as you get stronger, but the aim is to give you the tools for long-term independence.
Can physiotherapy help even if I have severe arthritis and might need surgery? Yes, absolutely. Physiotherapy is valuable at every stage of arthritis. For those with advanced joint damage, a consistent program can sometimes improve function and reduce pain enough to delay or even avoid surgery. If surgery does become necessary, physiotherapy is a critical part of the process. Going into an operation with stronger muscles can lead to a smoother recovery, and post-surgical rehab is essential for regaining your strength and mobility.
Do I need a referral from my doctor to start physiotherapy? In many states, including Michigan, you can see a physiotherapist directly without a referral from a physician. This is called Direct Access, and it allows you to get an evaluation and start treatment sooner. While a referral isn't always required to be seen, it's a good idea to check with your insurance provider to understand their specific requirements for coverage.
Understanding Visit Frequency
Physiotherapy isn't about endless appointments. The main goal is to empower you with the knowledge to manage your arthritis at home. Sessions typically last about an hour, and a significant portion of that time is dedicated to teaching you how to do your exercises and treatments on your own. It helps to think about your personal goals before you start, like being able to get in and out of your car without pain. You don’t need to go every week indefinitely. For many people, a few visits over a couple of months are enough to establish a solid plan, with occasional check-ins to make adjustments as you get stronger.
Checking Your Insurance Coverage
Before you begin, it’s a good idea to understand what your insurance plan covers. The best way to get clear answers is to call your insurance company directly and ask a few key questions. Find out if physiotherapy is covered for your condition, what your copay or deductible will be, and if there's a limit on the number of sessions per year. You can ask your doctor for a recommendation for a therapist, or you can search for one yourself using the American Physical Therapy Association's online tool. Taking a few minutes to sort out the financial details upfront can help you focus on what really matters: feeling better.
Frequently Asked Questions
Is light therapy safe for athletes?

Yes, light therapy is completely safe and highly beneficial for athletes. It promotes faster muscle recovery, reduces inflammation, and supports performance without the risks of medication or downtime. That’s why professional and amateur athletes worldwide rely on it to train smarter and recover quicker.
How many sessions will I need?

The number of sessions varies depending on the type and severity of your condition. Many patients notice improvement after 3–5 sessions, while chronic conditions may require ongoing care for best results. During your initial consultation, we’ll design a personalized treatment schedule tailored to your body’s response and recovery goals.




