

Spinal Injections for Arthritis: A Simple Guide
Think of a spinal injection as a way to press pause on your arthritis pain. It can calm the inflammation and quiet the pain signals, giving your body a chance to reset. But what you do during that pause is what truly creates lasting change. The most effective approach uses the relief from an injection as a bridge to other healing therapies. By pairing medical treatments with natural, non-invasive options like light therapy and targeted physical therapy, you can extend your results and build a stronger foundation for long-term wellness. This article explores how spinal injections for arthritis can be a powerful part of a comprehensive, holistic strategy for feeling and moving better.
Key Takeaways
- Injections provide targeted relief to calm inflammation: They are designed to reduce pain directly at the source, giving you a much-needed break from chronic discomfort and interrupting the pain cycle.
- Pair injections with other therapies for lasting results: The period of pain relief after an injection is the ideal time to engage in physical therapy and natural treatments like light therapy to build strength and address root causes.
- Build a comprehensive pain management strategy: Work with your healthcare team to create a personalized plan that uses injections as a stepping stone toward sustainable wellness, not as a standalone solution.
What Are Spinal Injections for Arthritis?
If you’re dealing with arthritis-related back pain, you’ve likely heard about spinal injections. They are a common treatment option doctors use to manage pain and inflammation directly at the source. Instead of taking an oral medication that affects your whole body, these injections deliver medicine right to the specific joints or nerves in your spine that are causing trouble. This targeted approach is often used for conditions like spinal osteoarthritis, sciatica, and spinal stenosis, where inflammation is a key driver of discomfort.
The goal is to reduce pain enough to improve your mobility and quality of life, potentially making it easier to participate in other therapies like physical therapy. Think of it as a way to calm down an irritated area so you can get back to moving more comfortably. While they can be an effective part of a pain management plan for many people, they are an invasive procedure and aren't a permanent fix. It’s important to understand how they work and who they’re best suited for before deciding if they’re the right path for you.
How They Work for Pain Relief
Spinal injections typically use a powerful combination of two types of medication: an anesthetic and a corticosteroid. The anesthetic, similar to what a dentist uses, provides immediate but temporary relief by numbing the painful area. This can help confirm that the injection was delivered to the right spot. The real workhorse is the corticosteroid, a strong anti-inflammatory medicine.
This steroid gets to work over the next few days, helping to reduce inflammation and swelling around the spinal nerves and joints. By calming this irritation, the injection can interrupt the pain signals being sent to your brain. This process can lead to significant pain relief that might last anywhere from a few weeks to several months, giving your body a much-needed break from constant discomfort.
Who Can Benefit from Them?
Spinal injections can be a helpful option for a wide range of people, but they are particularly effective for those with specific types of pain. If you experience sharp, shooting pain that travels from your lower back down into your leg—a classic sign of sciatica—you might be a good candidate. This type of nerve pain, also known as lumbar radicular pain, often responds well to the targeted anti-inflammatory effects of an injection.
People with pain localized to the small facet joints in the spine due to osteoarthritis may also find relief. Ultimately, these injections are considered when more conservative treatments like physical therapy or oral medications haven't provided enough relief. Your doctor will help determine if your specific symptoms and condition make you a good candidate.
What Are the Different Types of Spinal Injections?
When you hear "spinal injection," you might picture a single procedure, but there are actually several different types. Each one is designed to target a specific area of your spine where pain originates. Understanding the options can help you have a more informed conversation with your doctor about what might work for you. Think of it as a toolkit—the right tool is chosen based on the exact source of your discomfort. Let's break down the most common types so you can feel more prepared.
Epidural Steroid Injections
This is one of the most common injections for back pain. Epidural steroid injections (ESIs) deliver a powerful anti-inflammatory medication directly into the epidural space, which is the area surrounding your spinal nerves. They are often used to address chronic low back pain that stems from conditions like herniated discs or spinal stenosis. The main goal is to reduce inflammation and calm irritated nerves, which in turn provides pain relief. This can create a valuable window of opportunity for you to engage in physical therapy and other exercises to build long-term strength.
Facet Joint Injections
Your spine is made up of a stack of bones called vertebrae, and they are connected by small joints on each side known as facet joints. Just like your knees or hips, these joints can develop arthritis and become a source of pain. Facet joint injections deliver a mix of steroid and numbing medication directly into these small joints. This approach is very effective for people experiencing pain from osteoarthritis in the spine. The relief from these injections can last for several weeks to months, making it easier to manage daily activities.
Sacroiliac Joint Injections
If your low back pain is concentrated where your spine connects to your pelvis, the sacroiliac (SI) joint could be the source. This joint is a common but often overlooked cause of low back pain. Sacroiliac joint injections are used to treat pain that comes from inflammation or dysfunction in this specific joint. By delivering medication directly to the site of the problem, these injections can provide significant relief and improve your mobility, making movements like walking, standing, or climbing stairs much less painful.
Transforaminal Epidural Steroid Injections
This injection has a long name, but it’s a very precise procedure. Also known as a selective nerve-root block, it involves injecting medication exactly where a nerve exits the spine through an opening called the foramen. This approach is particularly effective for treating the sharp, radiating back and leg pain (like sciatica) caused by a pinched or inflamed nerve root. By targeting the specific nerve that’s causing trouble, these injections can provide very focused back pain relief right where you need it most.
Which Arthritis Conditions Do Spinal Injections Treat?
Spinal injections aren't a one-size-fits-all solution, but they are used to target pain from several specific arthritis-related conditions. By delivering medication directly to the source of inflammation, these injections can offer relief for issues stemming from joint degeneration, nerve pressure, and chronic irritation in the spine. If you're dealing with persistent back or neck pain, understanding which conditions respond well to this treatment can help you have a more informed conversation with your doctor about your options.
Osteoarthritis in the Spine
Osteoarthritis is often called "wear and tear" arthritis, and for good reason. Over time, the protective cartilage that cushions the joints in your spine can break down, leading to pain, stiffness, and inflammation. This is a common cause of chronic back and neck pain, particularly as we get older. When this happens, spinal injections can help by delivering anti-inflammatory medication directly to the affected joints. The goal is to alleviate the pain associated with this degeneration, giving you a window of relief from the discomfort and making it easier to stay active.
Spinal Stenosis
Spinal stenosis is a condition where the spaces within your spine begin to narrow. This narrowing can put pressure on the nerves that travel through the spine, causing pain, numbness, or weakness, often in the legs. You might hear this type of radiating pain referred to as sciatica. Epidural steroid injections are a common treatment for spinal stenosis because they can help reduce the inflammation around the compressed nerves. By calming the swelling, the injection can create more space and relieve the pressure that’s causing your symptoms, offering a break from that persistent, traveling pain.
Nerve Pain and Radiculopathy
At its core, much of the pain from spinal arthritis comes down to irritated nerves. Radiculopathy is the medical term for pain that occurs when a nerve in the spine is pinched or inflamed. This can cause sharp, shooting pain that travels from your back down into your limbs. The primary purpose of a lumbar epidural steroid injection is to manage this type of chronic low back and nerve pain. The steroid medication works to decrease swelling and pressure on these irritated nerves, which helps to block pain signals and provide significant relief from the sharp, disruptive symptoms that can make daily life so challenging.
Are Spinal Injections Right for You?
Deciding on spinal injections is a big step, and it’s a choice you’ll want to make with your healthcare team. They aren’t a first-line defense against arthritis pain; they’re typically considered when other methods haven’t provided the relief you need. Understanding what they do, when they’re used, and who they’re for will help you have a productive conversation with your doctor. This will help you figure out if this is the right path for your personal pain management plan and your specific health goals.
Key Factors to Consider
When doctors suggest spinal injections, they usually have one of two goals. The first is diagnostic—to help pinpoint the exact source of your pain. By injecting a numbing agent into a specific spot, your doctor can see if it temporarily relieves your pain. If it does, they’ve likely found the culprit. The second goal is therapeutic, meaning the injection is intended to provide longer-lasting relief, usually with a corticosteroid to reduce inflammation. Knowing which goal applies to you helps clarify the procedure's purpose and sets realistic expectations for the outcome.
When Other Treatments Haven't Worked
Spinal injections are rarely the first suggestion for arthritis pain. They are often recommended when more conservative treatments haven’t been effective enough, especially for severe pain that interferes with daily life. Your doctor will likely want you to try physical therapy, lifestyle adjustments, or oral medications first. If you’ve given these methods a fair shot and are still struggling, that’s when spinal injections might enter the conversation. It’s a way to deliver targeted treatment directly to the problem area when broader approaches fall short.
Health Conditions to Discuss with Your Doctor
An open conversation about your full health history is crucial before scheduling an injection. Certain conditions can increase the risk of side effects. For example, if you have diabetes, a steroid injection can cause a temporary spike in blood sugar. People with glaucoma might see a brief increase in eye pressure. It’s also important to tell your doctor if you have any active infections, take blood thinners, or have uncontrolled high blood pressure, as these may mean an injection isn't a safe option for you. Being transparent allows your doctor to make the safest recommendation.
Weighing the Pros and Cons of Spinal Injections
Deciding on any medical procedure, even a common one like spinal injections, means looking at the full picture. For many people dealing with arthritis pain, these injections can be a game-changer, but it’s just as important to understand the potential downsides and what to realistically expect. Thinking through the benefits and risks helps you and your doctor make the best choice for your health and your life.
The Upside: Pain Relief and Better Movement
The biggest advantage of spinal injections is targeted pain relief. When you’re dealing with conditions like osteoarthritis or spinal stenosis, inflammation around your spinal joints and nerves is often the primary source of pain. Injections deliver anti-inflammatory and anesthetic medication directly to that spot. This can quickly reduce swelling and block pain signals, offering a welcome break from discomfort. For many, this relief isn't just about feeling better—it's about moving better. It can create a crucial window of opportunity to engage more effectively in physical therapy and other treatments that build long-term strength and stability.
The Risks: Side Effects and Complications
While generally considered safe, spinal injections do come with potential side effects. Most are mild and temporary, like tenderness or bruising at the injection site or a brief spike in pain before the medication kicks in. However, there are also rare but more serious risks to be aware of, including infection, bleeding, nerve irritation, or a severe headache if spinal fluid leaks. It’s essential to have an open conversation with your doctor about your health history to understand your specific risk factors. Knowing the possibilities, both common and rare, empowers you to make a truly informed decision about your care.
Clearing Up Common Myths
One of the biggest misconceptions about spinal injections is that they are a permanent fix. While some people experience relief for several months, injections are typically a tool for temporary pain management, not a long-term cure. They are designed to calm a painful flare-up and help you get back to other therapies that address the root cause of your pain. Another myth is that you’ll need an endless series of shots. Most insurance plans cover a few injections per year, but the goal is often to achieve lasting relief with as few as possible, using them as a bridge to more sustainable wellness strategies.
What to Expect During the Procedure
If you’re considering a spinal injection, knowing what the process involves can help you feel more prepared and confident. The entire procedure is typically very quick, often completed in under 30 minutes. It’s a routine treatment performed by a specialist who has done it countless times. From preparing for your appointment to knowing what to do afterward, here’s a simple breakdown of what the experience is like.
How to Prepare for Your Appointment
Your main job before the procedure is to communicate clearly with your doctor. Be ready to discuss your full health history. Make sure to mention if you might be pregnant, and provide a complete list of all medications you take, including over-the-counter drugs, herbs, and supplements. It’s especially important to tell your doctor if you take any blood thinners, as you may need to pause them temporarily. Your doctor might also ask you to avoid eating or drinking for a few hours before your appointment. Following these instructions carefully helps ensure everything goes smoothly and safely on the day of your injection.
A Step-by-Step Look at the Process
When you arrive, a specially trained doctor will guide you through the process. You’ll likely lie on your stomach on an exam table so they can easily access your back. The doctor will clean the injection site and numb the skin to minimize discomfort. To ensure perfect placement, they use a type of X-ray called fluoroscopy to see exactly where the needle is going in real-time. You might feel a bit of pressure or a tingling sensation as the medication is injected, but the procedure itself is usually over in 15 to 30 minutes.
Your Recovery and Aftercare Plan
After the injection, you’ll rest for a short while before heading home. It’s a good idea to have someone drive you. Don’t be surprised if your pain feels a little worse for the first day or two—this is a common reaction before the steroid begins to work. The real relief typically starts within two to seven days. Plan on taking it easy for the rest of the day. You can usually manage any soreness with an ice pack or approved over-the-counter pain relievers. Your doctor will provide specific aftercare instructions to help you get the best results.
How Long Does the Pain Relief Last?
One of the biggest questions people have about spinal injections is how long the relief will actually stick around. It’s a fair question—you want to know if the procedure is worth it for you. The answer isn't one-size-fits-all; it really depends on your specific condition, the type of injection you receive, and how your body responds. For some, an injection can provide months of significant relief, allowing them to get back to activities they love and engage more fully in physical therapy. For others, the effects might be shorter-lived.
The goal of these injections is to reduce inflammation and interrupt the pain signals that are making you miserable. This creates a window of opportunity where you can move more freely and work on strengthening the muscles that support your spine. Think of it less as a permanent cure and more as a tool to help you break the cycle of pain and inactivity. Understanding the typical timeline, what influences the duration of relief, and how often you can safely receive injections will help you set realistic expectations and make an informed decision with your doctor.
A Timeline for Relief
After your injection, you won't walk out of the office instantly pain-free forever. There’s a typical progression of what you can expect. The procedure itself is quick, but you might notice your pain gets a bit worse for two or three days before it starts to improve. This is a normal reaction as your body adjusts. The medication usually begins to work within two to seven days. From there, the duration of pain relief can vary widely, lasting anywhere from a few days to several months. For some lucky individuals, the effects can last even longer, providing a substantial period of comfort and improved mobility.
What Makes the Effects Last Longer?
The lasting power of a spinal injection comes from its two-part approach. First, an anesthetic provides immediate, though temporary, pain relief. The real workhorse is the corticosteroid, which starts to kick in within a few days to calm inflammation around the nerve roots. By blocking pain signals and reducing that inflammation, the injection creates an environment where your body can start to heal. The duration of these effects often depends on the severity of your condition and what you do during your period of relief. Pairing the injection with physical therapy or other supportive treatments can help you build strength and stability, potentially extending the benefits.
How Often Can You Get Injections?
Spinal injections are not a treatment you can receive indefinitely. Because the corticosteroids can have side effects with overuse, doctors are careful about how frequently they administer them. Generally, you’ll be limited to just two or three injections per year. This is to protect your health and avoid potential long-term issues, such as the weakening of your spinal bones or nearby muscles. While some insurance plans may cover more, most healthcare providers agree that spacing them out is the safest approach. The aim is to use them strategically to manage flare-ups and provide enough relief to make progress with other long-term pain management strategies.
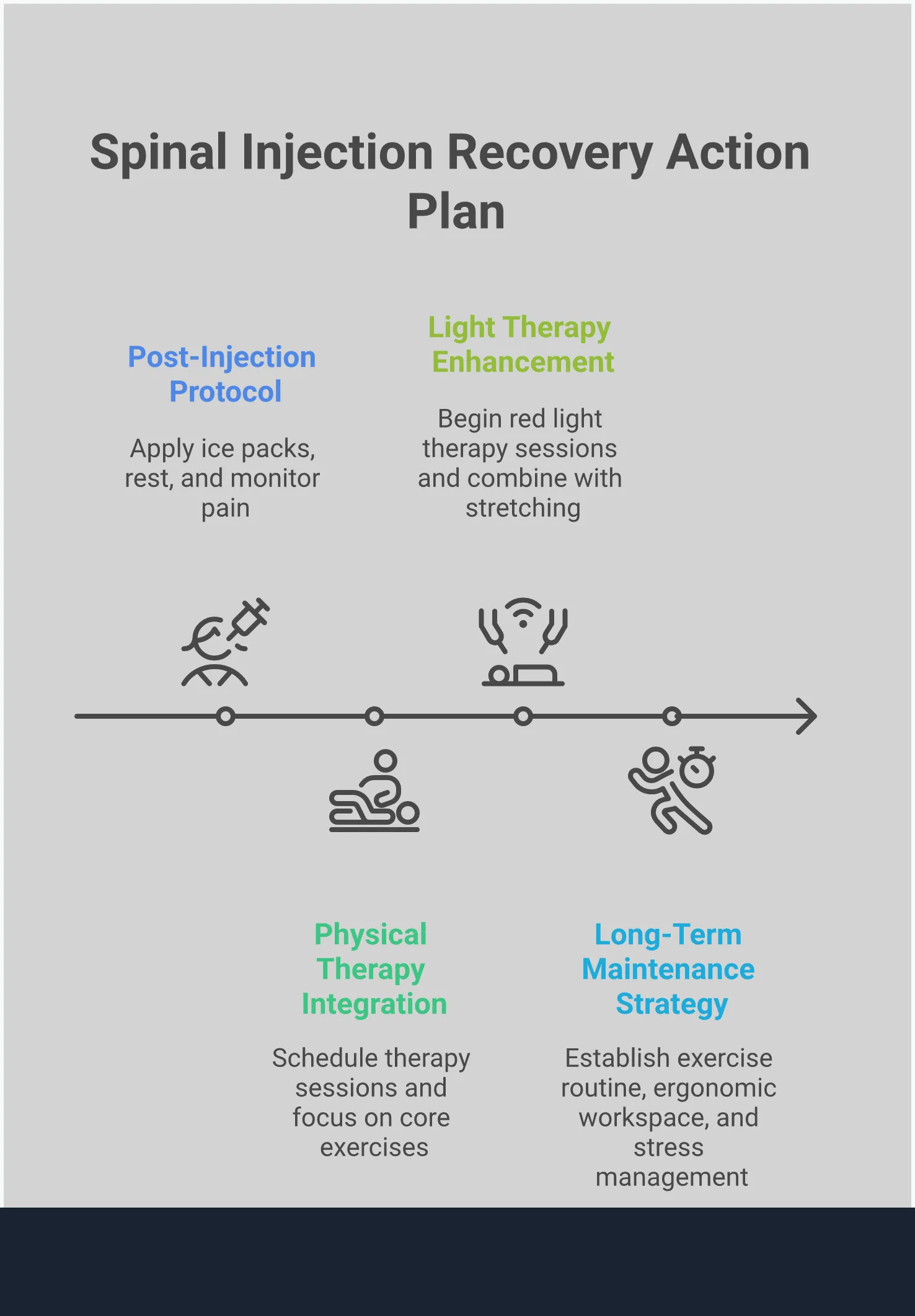
Pairing Injections with Natural Therapies for Better Results
Think of a spinal injection as a tool that opens a window of opportunity. It can significantly reduce your pain, but what you do during that period of relief is what truly sets the stage for long-term success. Instead of just waiting for the pain to return, you can use this time to build a stronger, more resilient body. Pairing injections with natural, non-invasive therapies creates a powerful synergy, addressing the symptoms while also tackling the underlying issues contributing to your arthritis pain.
This comprehensive approach to pain management helps you get more out of your medical treatment. By integrating therapies that support your body’s natural healing processes, you can extend the benefits of the injection and create a more sustainable plan for feeling and moving better. It’s about moving beyond temporary fixes and building a foundation for lasting wellness. This strategy puts you in the driver’s seat, empowering you to take an active role in your health journey.
Using Light Therapy to Reduce Inflammation
One of the most effective partners for spinal injections is light therapy. This non-invasive treatment uses specific wavelengths of light to penetrate the skin and stimulate healing at a cellular level. Since inflammation is a primary target of both spinal injections and light therapy, using them together can deliver a powerful one-two punch. The injection provides immediate, targeted relief, while light therapy works to reduce inflammation throughout the area and promote tissue repair.
This combination can help enhance the effects of the injection and support your body’s healing capacity. By calming inflammation naturally, light therapy helps create a healthier environment for your joints and tissues, making it a key component of any plan for preventative wellness.
The Role of Physical Therapy and Movement
Once the injection has eased your pain, it’s the perfect time to focus on movement. A structured physical therapy program can make a world of difference in your recovery. A physical therapist will guide you through exercises designed to strengthen the muscles that support your spine, improve your flexibility, and restore proper function. This isn’t about pushing through pain; it’s about using your newfound comfort to build a stronger foundation.
Think of it as retraining your body to move in a healthier way. By strengthening your core and back muscles, you reduce the strain on your joints, which can help prevent future flare-ups. This proactive step is crucial for anyone looking to optimize their performance recovery and maintain an active lifestyle.
Building a Holistic Pain Strategy
A truly effective treatment plan looks at the bigger picture. A holistic strategy combines medical treatments like injections with supportive therapies and positive lifestyle changes. This could include incorporating gentle movement, mindfulness practices to manage stress, or other complementary therapies like massage. The goal is to create a well-rounded approach that supports your entire well-being, not just a single symptom.
By building a comprehensive plan, you’re investing in your long-term health. This approach allows you to address pain from multiple angles, giving you more tools to manage your condition effectively. It’s about creating a sustainable routine that helps you feel your best, and our memberships are designed to support you every step of the way.
Creating Your Arthritis Treatment Plan
Spinal injections can be a game-changer for arthritis pain, but they aren't a magic wand. The most effective approach treats the injection as one piece of a bigger puzzle—a powerful tool that opens the door to other healing therapies. A successful strategy for long-term relief involves building a comprehensive treatment plan that’s tailored specifically to you, your body, and your lifestyle. This plan goes beyond the procedure itself, incorporating therapies and habits that support your spine's health for the long haul.
Think of it as a roadmap to feeling and moving better, with the injection being a key stop along the way. The goal is to use the window of pain relief from the injection to build strength, improve mobility, and address the root causes of your discomfort. This is where a holistic approach truly shines. By combining the immediate relief of an injection with ongoing care like physical therapy and natural treatments, you create a powerful synergy that promotes lasting wellness. Creating this plan starts with a conversation and a partnership between you and your healthcare providers. You can find great educational resources and support to help you get started on the right path.
How to Work with Your Healthcare Team
Your journey to pain relief is a team sport, and you’re the captain. Your team might include your primary doctor, a spine specialist, a physical therapist, and wellness experts. Your role is to communicate openly about your pain levels, your goals, and any concerns you have. Be honest about what’s working and what isn’t. Remember, an injection isn't usually the final step. As pain specialists often explain, injections can provide enough relief to allow you to fully participate in other therapies, like physical therapy, that address the underlying condition. The team at Laser Lab Therapy is here to be a part of your support system, helping you find natural solutions that complement your medical care.
Designing Your Personal Pain Management Plan
Once you have your team in place, it’s time to map out your plan. This plan should cover what happens right after your injection and what you’ll do in the weeks and months that follow. Immediately after, your doctor will likely recommend taking it easy for a day or two and avoiding heat on the injection site. From there, your plan should focus on proactive care. This is the perfect time to integrate physical therapy to strengthen supporting muscles and improve flexibility. It’s also an ideal opportunity to explore gentle, non-invasive treatments like light therapy, which can help reduce inflammation and support your body’s natural healing processes. Your personal pain management plan is a living document—it should evolve as you get stronger and feel better.
Frequently Asked Questions
Are the injections themselves painful? This is a very common and understandable question. Your doctor will take steps to make the procedure as comfortable as possible. They start by cleaning the area and then using a local anesthetic to numb your skin and the tissue underneath. While you might feel a bit of pressure or a brief stinging sensation when the numbing medication is applied, the injection itself shouldn't be sharply painful. Most people find the process very manageable.
How soon can I return to my regular activities, like exercise? It’s best to plan on taking it easy for the rest of the day after your procedure. Most doctors recommend avoiding strenuous activities for at least 24 to 48 hours to let the medication settle in and begin working. After that, you can typically start to gradually resume your normal routine. It's important to listen to your body and follow the specific instructions from your healthcare provider, especially when it comes to reintroducing exercise.
If the injection provides relief, why do I need other therapies like light therapy or physical therapy? Think of the injection as a tool that quiets the pain and inflammation, creating a valuable window of opportunity. That period of relief is the perfect time to address the underlying issues. Physical therapy helps you build strength and stability to better support your spine, while natural treatments like light therapy can help manage inflammation on an ongoing basis. Using these therapies together helps you get more lasting results from the injection and builds a stronger foundation for long-term health.
Will a spinal injection cure my spinal arthritis? Spinal injections are a highly effective tool for managing pain, but they are not a cure for arthritis. Arthritis is a chronic condition, and the goal of an injection is to provide temporary relief from a painful flare-up. This relief can last for several months, giving you a break from discomfort and allowing you to engage in other therapies that can improve your condition over the long term.
How do I know which type of injection is right for me? The specific type of injection you receive depends entirely on the exact source of your pain. Your doctor will use a combination of your symptoms, a physical exam, and imaging tests like X-rays or an MRI to pinpoint which joints or nerves are causing the problem. This diagnosis determines whether a facet joint, epidural, or another type of targeted injection will be the most effective approach for you.
Frequently Asked Questions
Is light therapy safe for athletes?

Yes, light therapy is completely safe and highly beneficial for athletes. It promotes faster muscle recovery, reduces inflammation, and supports performance without the risks of medication or downtime. That’s why professional and amateur athletes worldwide rely on it to train smarter and recover quicker.
How many sessions will I need?

The number of sessions varies depending on the type and severity of your condition. Many patients notice improvement after 3–5 sessions, while chronic conditions may require ongoing care for best results. During your initial consultation, we’ll design a personalized treatment schedule tailored to your body’s response and recovery goals.




